Hospital safety and quality
Regulatory systems and arrangements to ensure the safety and quality of hospital services in Australia include those for:
- medicines and devices
- health facilities
- the health workforce
- clinical standards and guidelines
- clinical governance arrangements.
Monitoring and improvement of care quality for particular illnesses and procedures also occurs, for example, through research projects, clinical quality registers and routinely collected health system data, such as the AIHW’s National Hospital Morbidity Database (NHMD). Patient experience surveys can also provide an indication of the quality of care provided from the patient’s perspective.
Hospital safety and quality measures reported include:
- Staphylococcus aureus bloodstream infections (SABSI) acquired in hospital
- hospital-acquired complications such as birth trauma
- patient experience survey results.
Staphylococcus aureus bloodstream infections
Staphylococcus aureus (also S. aureus, or ‘Golden staph’) is a type of bacteria that can cause bloodstream infection.
SABSI can be acquired after a patient receives medical care or treatment in a hospital. Contracting a Staph. aureus bloodstream infection while in hospital can be life-threatening and hospitals aim to have as few cases as possible. The nationally agreed benchmark for healthcare-associated Staphylococcus aureus bloodstream infections is no more than 1 case of healthcare-associated SABSI per 10,000 days of patient care for public hospitals in each state and territory.
In 2021–22, there were 1,546 SABSI cases occurring during 21.1 million days of patient care under surveillance. This represents a rate of 0.73 SABSI cases per 10,000 patient days.
Most SABSI cases (85%) were methicillin-sensitive and therefore treatable with commonly used antimicrobials.
Hospital-acquired complications
A hospital-acquired complication is a complication that arises during a patient’s hospitalisation which may have been preventable, and which can have a severe impact on both the patient and the care required.
Hospital-acquired complications include pressure injuries, healthcare-associated infections, malnutrition, neonatal birth trauma, cardiac complications, and delirium. They may affect a patient’s recovery, overall outcome and can result in a longer length of stay in hospital. A patient may have one or more hospital-acquired complications during a hospitalisation.
In 2021–22, 112,000 hospitalisations (2.1 per 100 hospitalisations) in public hospitals had at least one hospital-acquired complication, and 35,000 hospitalisations (0.9 per 100 hospitalisations) in private hospitals had at least one hospital-acquired complication.
The highest rates were related to healthcare associated infections (affecting 64,000 hospitalisations in public hospitals and 17,000 hospitalisations in private hospitals), delirium (affecting 19,000 hospitalisations in public hospitals and 6,200 hospitalisations in private hospitals) and cardiac complications (affecting 16,000 hospitalisations in public hospitals and 7,700 hospitalisations in private hospitals).
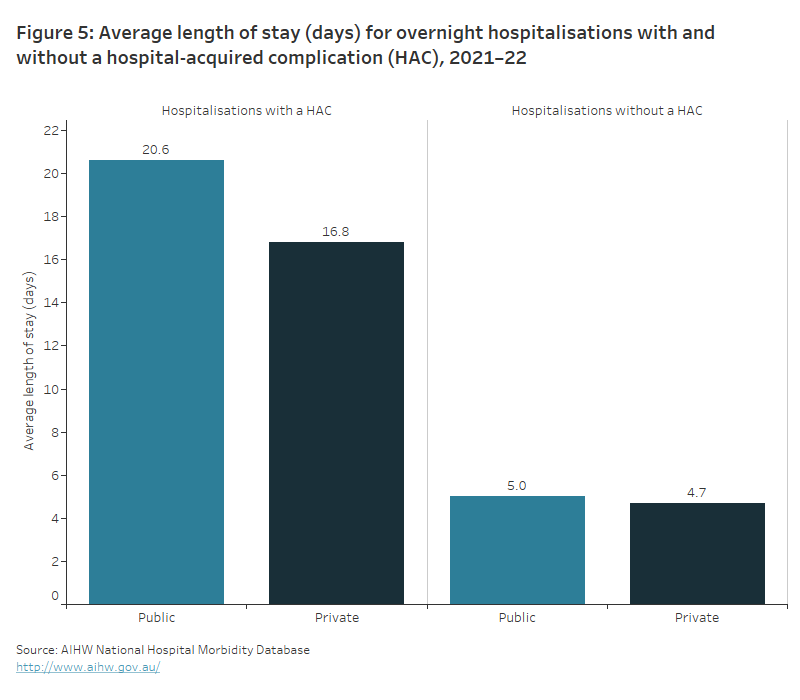
The bar chart shows the average length of stay in both public and private hospitals for overnight hospitalisations with and without a hospital-acquired complication in 2021–22. The average length of stay for overnight hospitalisations with a hospital-acquired complication was 20.6 days for public hospitals and 16.8 days for private hospitals. Whilst the average length of stay for overnight hospitalisations without a hospital-acquired complication was 5.0 days for public hospitals and 4.7 days for private hospitals.
What do patients say about their hospital experience?
The Australian Bureau of Statistics (ABS) conducts an annual survey, Patient Experiences, to monitor the experiences of Australians who use a range of healthcare services. People who have received hospital care or emergency department care are asked about their experiences with health professionals (ABS 2022).
Emergency department
Among people who attended an emergency department in 2022–23:
- 82% of patients responded that emergency department doctors ‘always’ or ‘often’ listened carefully to them.
- 85% of patients responded that emergency department doctors ‘always’ or ‘often’ showed respect.
- 77% of patients responded that emergency department doctors ‘always’ or ‘often’ spent enough time with them.
- 87% of patients responded that emergency department nurses ‘always’ or ‘often’ listened carefully to them.
- 89% of patients responded that emergency department nurses ‘always’ or ‘often’ showed respect.
- 82% of patients responded that emergency department nurses ‘always’ or ‘often’ spent enough time with them in the emergency department.
Admitted patients
Among people who received hospital care in 2022–23:
- 91% of patients responded that hospital doctors ‘always’ or ‘often’ listened carefully to them.
- 92% of patients responded that hospital doctors ‘always’ or ‘often’ showed respect.
- 86% of patients responded that hospital doctors ‘always’ or ‘often’ spent enough time with them.
- 92% of patients responded that hospital nurses ‘always’ or ‘often’ listened carefully to them.
- 93% of patients responded that hospital nurses ‘always’ or ‘often’ showed respect.
88% of patients responded that hospital nurses ‘always’ or ‘often’ spent enough time with them.
More information about the data
Australian Commission on Safety and Quality in Health Care
Patient Experiences, 2022-23 financial year | Australian Bureau of Statistics


