Epilepsy burden and expenditure
Burden of epilepsy
People living with epilepsy may experience poor health or die prematurely as a result of their condition. Both the fatal (dying prematurely) and non-fatal impact (living with poor health or disability) of epilepsy can be measured by burden of disease analysis. Burden of disease analysis combines the years of healthy life lost due to living with ill health (YLD) with the years of life lost due to dying prematurely (YLL). Fatal and non-fatal burden combined are referred to as total burden, and are reported using the disability-adjusted life years (DALY) measure (AIHW 2020). The Australian Burden of Disease Study 2018 measured the burden of over 200 diseases and injuries in Australia, including epilepsy.
Box 2: Australian Burden of Disease Study 2018
The Australian Burden of Disease Study (ABDS) 2018 provides Australian-specific burden of disease estimates for the total population for 2018, 2015, 2011 and 2003, as well as estimates of the disease burden attributable to specific risk factors. The study utilised and adapted methods developed as part of the previous ABDS 2015 and 2011 (AIHW 2019; AIHW 2016). The ABDS uses Australian data sources and adapts the methods from global studies to produce estimates that are relevant to the Australian context.
The fatal burden estimates for epilepsy were derived from the AIHW National Mortality Database and are considered to be of high quality. National non-fatal burden estimates for epilepsy were based on self-reported prevalence data from the National Health Survey (NHS) 2017–18. Age–sex specific distributions (including by state/territory) were calculated using counts of hospital separations from the AIHW National Hospital Morbidity Database which were adjusted to account for readmissions using linked hospitalisation and deaths data from the NIHSI AA v0.5. The severity distribution for epilepsy was based on a study conducted in the United Kingdom by Moran and others (2004). Prevalence estimates by severity were then mapped to health states and disability weights to calculate YLD. For more information on the YLD calculation for epilepsy, refer to the Australian Burden of Disease Study: methods and supplementary material 2018 web report.
In 2018, epilepsy was ranked the 30th cause for disease burden in Australia. The total burden of disease for epilepsy was highest among 15–19 year olds (3,600 DALY). Non-fatal burden was highest among 5–9 year olds (3,000 YLD) and fatal burden was highest in the 35–39 year age group (930 YLL) (Figure 3.1).
Figure 3.1 includes estimates for:
- disability-adjusted life years (DALY) due to epilepsy
- years lived with disability (YLD) due to epilepsy
- years of life lost (YLL) due to epilepsy
- deaths due to epilepsy.
More information on how burden of disease is calculated is available on the Burden of disease webpages.
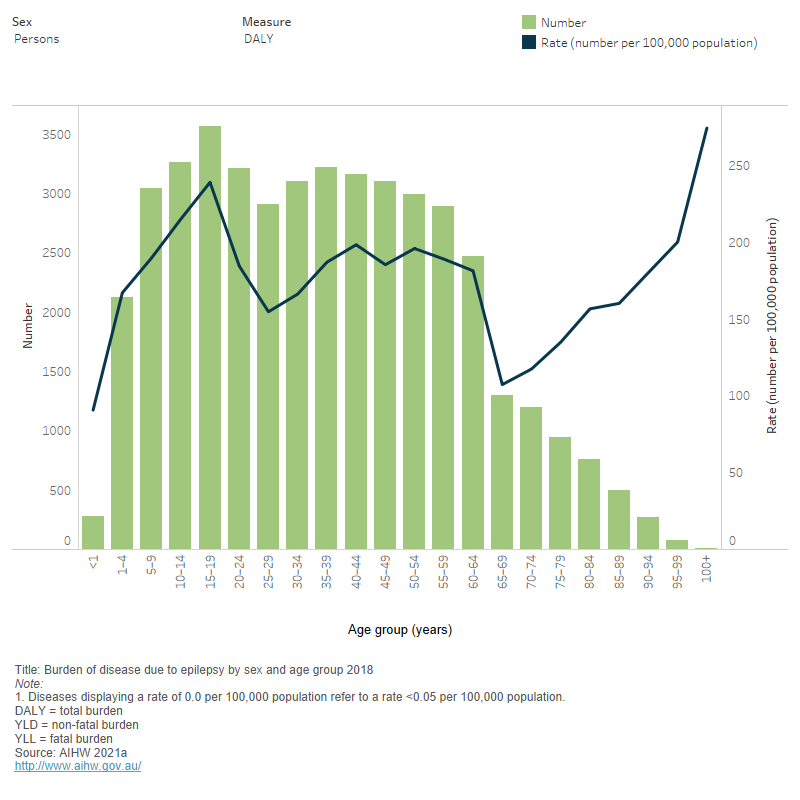
Figure 3.1: Burden of disease due to epilepsy, by measure, sex and age group 2018
This is a bar chart that displays the numbers and rates of the three measures of burden of disease due to epilepsy (DALY – total burden, YLD – non-fatal burden and YLL – fatal burden) by sex and age group. The non-fatal burden for persons shows a decline in the number of years lived with disability from age 5-9 onwards. The number of years lost due to fatal burden decreases with age from 55-59 years for persons. The total burden (DALY) decreases with age for persons from the age group 35-39.
Expenditure on epilepsy
Disease expenditure in Australia provides a broad picture of how health system resources are allocated directly to particular disease groups and conditions, and is a reference point for planners and researchers interested in costs and patterns for particular diseases. Around $134 billion of recurrent expenditure in 2018–19 could be attributed to specific disease groups. Expenditure directly attributable to epilepsy accounted for around $333 million of this expenditure, or 0.2%.
A number of different health system resources were utilised for epilepsy management across Australia in 2018–19. In terms of expenditure, the most utilised resource was public hospital admitted patient services, followed by use of the pharmaceutical benefits scheme and public hospital outpatient services.
Total epilepsy expenditure increased with age, peaking at over $22 million in the 50–54 year old age group. However, from the 55–59 year old age group, epilepsy expenditure declined with age.
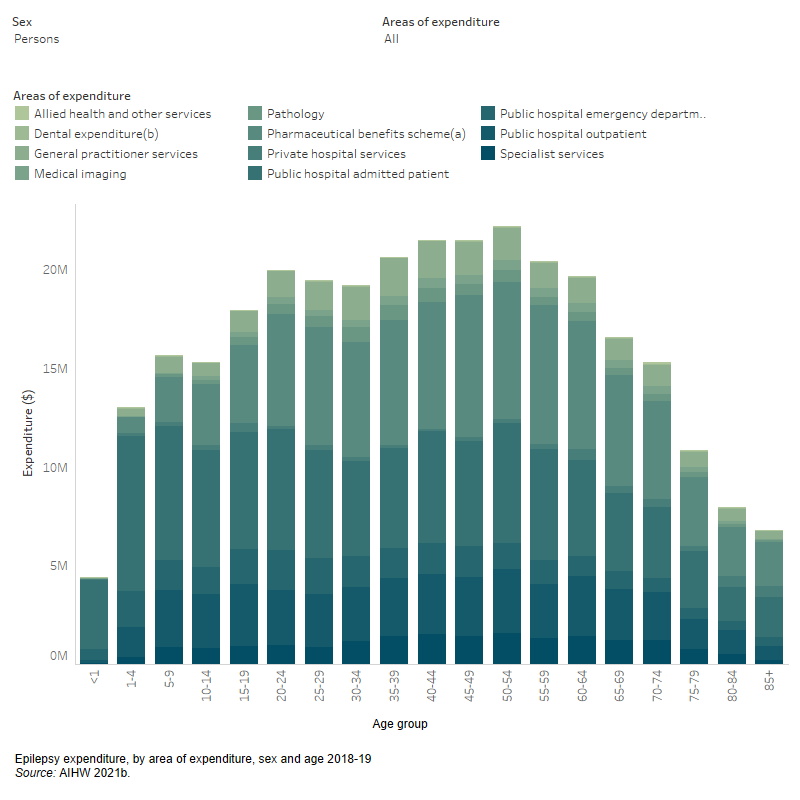
Total epilepsy expenditure was higher for males in the majority of age groups compared with females (Figure 3.2).
More information on how disease expenditure is calculated for health services is available on the Health and welfare expenditure webpages. This includes costs that are not included in this estimate such as provision of aged care services of people with epilepsy.
This is a bar chart that displays health system expenditure directly for epilepsy by 5-year age groups. It can also be filtered by sex and area of expenditure. Across all areas of expenditure, males aged 50-54 years had the highest expenditure directly for epilepsy while females aged 40-44 years old had the highest expenditure.
References
AIHW 2021a. Australian Burden of Disease Study: impact and causes of illness and death in Australia 2018. Australian Burden of Disease Study series no. 23. Cat. no. BOD 29. Canberra: AIHW.
AIHW 2021b. Disease expenditure in Australia 2018–19. Cat. no. HWE 81. Canberra: AIHW.


