Methods
On this page:
NHS chronic condition definitions
The 10 chronic conditions included in this analysis are arthritis, asthma, back problems, cancer, selected cardiovascular diseases, chronic obstructive pulmonary disease (COPD), chronic kidney disease, diabetes, mental and behavioural conditions, and osteoporosis.
The NHS uses 3 factors to determine whether or not a person is counted as having a particular condition: whether the condition is current, whether it is long term and whether it was medically diagnosed. The combination of these factors required for a person to count as having the condition varies according to the nature of the condition (Table 2). For example, some conditions, such as diabetes and cardiovascular disease, once diagnosed, are seen to be lifelong. Even if a person no longer reports symptoms, they still count as having the condition. While other conditions, such as depression, asthma, cancer or back problems, can be lifelong, episodic or in complete remission.
Most conditions do not need the respondent to have been diagnosed by a doctor or nurse. The respondent is counted if they said they have the condition – that is, if they have self-reported the condition. However, in cases where the respondent said they had diabetes or cardiovascular disease and that the condition was not current, they need to have received a diagnosis to be counted. See the National Health Survey questionnaire, 2017–18 and the National Health Survey: Users’ Guide, 2017–18 for more information.
|
Condition |
Current |
Long term |
Has the condition been diagnosed by a doctor or nurse? |
|---|---|---|---|
|
Arthritis |
current |
long term |
no diagnosis required |
|
Asthma |
current |
long term |
no diagnosis required |
|
Back problems |
current |
long term |
no diagnosis required |
|
Cancer |
current |
long term |
no diagnosis required |
|
Selected cardiovascular diseases (heart, stroke and vascular disease) (2 combinations) |
current ever had |
long term not long term |
no diagnosis required diagnosis required |
|
Chronic kidney disease |
current |
long term |
no diagnosis required |
|
COPD |
current |
long term |
no diagnosis required |
|
Diabetes (2 combinations)
|
current ever had |
long term not long term |
no diagnosis required diagnosis required |
|
Mental and behavioural conditions |
current |
long term |
no diagnosis required |
|
Osteoporosis |
current |
long term |
no diagnosis required |
Grouping data for analysis
Remoteness area
Remoteness is classified according to the Australian Statistical Geography Standard (ASGS) 2016 Remoteness Areas structure based on area of residence. Remoteness Areas divide Australia into 5 classes of remoteness on the basis of a measure of relative access to services. The 5 remoteness areas are Major cities, Inner regional, Outer regional, Remote and Very remote. Refer to the ABS Remoteness structure for more information.
Very remote areas are not included in this analysis, as these areas are outside of the scope of the NHS 2017–18. For more information see the section ‘Scope of the survey’ in the ABS National Health Survey: First results methodology, 2017–18.
Socioeconomic area
Socioeconomic areas are classified according to the Socio-Economic Indexes for Areas (SEIFA), specifically the Index of Relative Socio-Economic Disadvantage (IRSD).
The IRSD classifies individuals according to the socioeconomic characteristics of the area in which they live. It scores each area by summarising attributes of the population, such as low income, low educational attainment, high unemployment and jobs in relatively unskilled occupations. Areas can then be ranked according to their score. In this analysis, the population living in the 20% of areas with the greatest overall level of disadvantage is described as the ‘lowest socioeconomic areas’. The 20% of areas with the lowest level of disadvantage – the top fifth – is described as the ‘highest socioeconomic areas’.
Note that the IRSD reflects the overall or average level of disadvantage of the population of an area; it does not show how individuals living in the same area differ from each other in their socioeconomic position. Refer to the ABS Socio-economic indexes for areas (SEIFA) 2016 for more information.
Family composition of household
Family composition of the household describes the members of the household to which the respondent belongs to. The following categories were used in this analysis:
- Couple family with dependent children
- Couple only
- Lone person
- One parent family with dependent children
- Other: includes other one family households, multiple family households and group households.
Analysis excludes cases where the family composition of the household could not be determined.
Tenure type of household
Participants were asked about the dwelling in which they were surveyed. In most cases this was their usual place of residence. Only those who indicated that they were in a dwelling that was owned (including partly owned or being paid off with a mortgage/secured loan) or being rented are included in analysis.
People who indicated the dwelling they were in was being purchased under a shared equity scheme, occupied under a life tenure scheme, occupied rent free or not stated were excluded due to small numbers for analysis.
Smoking status
Refers to the frequency of smoking tobacco, including manufactured (packet) cigarettes, roll-your-own cigarettes, cigars and pipes, but excluding chewing tobacco, electronic cigarettes (and similar) and smoking of non-tobacco products. Smoking status is categorised as:
- Current smoker: includes daily smokers (regularly smoked one or more cigarettes, cigars or pipes per day) and occasional smokers (smoked cigarettes, cigars or pipes, less frequently than daily).
- Ex-smoker: a respondent who reported that they did not currently smoke, but had regularly smoked daily, or had smoked at least 100 cigarettes, or smoked pipes, cigars, etc. at least 20 times in their lifetime.
- Never smoked: a respondent who reported they had never regularly smoked daily, had smoked less than 100 cigarettes in their lifetime and had smoked pipes, cigars, etc. less than 20 times.
Alcohol consumption
This report has classified alcohol consumption based on the 2009 National Health and Medical Research Council guidelines for the consumption of alcohol which were current at the time of survey. Only the 2009 lifetime risk guideline is used in this analysis, which considers average daily consumption of alcohol. A number of factors are included in the calculation of average daily consumption of alcohol:
- the type, brand, number and serving sizes of alcoholic beverages consumed
- the amount consumed on 3 most recent days of the week prior to interview (on which the respondent consumed alcohol), and
- the total number of days alcohol was consumed in the week prior to interview.
Respondents were classified as exceeding guidelines if more than 2 standard drinks were consumed per day on average. Respondents were classified as not exceeding guidelines if less than 2 standard drinks were consumed per day on average, or if they had not consumed alcohol in the last week. People that consumed alcohol at levels that put them at a lifetime risk of harm may or may not be considered to have an alcohol or drug problem (captured in the ‘mental and behavioural conditions’ group considered in this analysis).
Those for which the time since they last consumed alcohol was not known were excluded from analysis.
The 2009 guidelines were replaced in 2020, and the new guidelines recommend that healthy men and women should drink no more than 10 standard drinks a week and no more than 4 standard drinks in any one day (NHMRC 2020). Data on the new guidelines was not available for this report.
Physical activity
In this analysis physical activity includes walking for transport, walking for fitness, sport or recreation, moderate exercise and vigorous exercise, and workplace physical activity (moderate and vigorous) undertaken in the last week. Based on the current Australia’s Physical Activity and Sedentary Behaviour Guidelines (Department of Health 2019), insufficient physical activity is defined in this analysis as:
- adults aged 18–64 who did not complete 150 minutes of moderate intensity physical activity or 75 minutes of vigorous intensity physical activity, or an equivalent combination of both, across 5 or more days in the last week and did not do muscle strengthening activities on at least 2 days each week
- adults aged 65 and over who did not do some form of physical activity every day, and did not complete at least 30 minutes of moderate intensity physical activity per day on 5 or more days in the last week.
People for whom this measure was not stated are not included in analysis.
Body Mass Index
Body Mass Index (BMI) is commonly used to classify underweight, normal weight, overweight and obesity. It is calculated from height and weight information, using the formula weight (kg) divided by the square of height (m). The NHS uses measured height and weight to calculate the BMI of survey respondents. In 2017–18, 34% of respondents aged 18 and over did not agree to have their height and weight measured. For these respondents, height and weight was imputed and used to calculate a BMI. For more information see ‘Appendix 2: Physical measurements’ in the 2017–18 National Health Survey methodology.
In this analysis people were classified as ‘underweight/normal’ (based on a BMI of less than 25) or ‘overweight/obese’ (based on a BMI of 25 or greater).
Self-assessed health
Self-assessed health status reflects a person's subjective perception of his or her own health at the time of interview. In the 2017–18 NHS, survey participants were asked “In general would you say that your health is excellent, very good, good, fair or poor?” Those who rated their health as ‘fair’ or ‘poor’ were grouped in analysis under the label poor self-assessed health, and those who rated their health as ‘excellent’, ‘very good’ or ‘good’ formed another group labelled good self-assessed heath.
Bodily pain
Bodily pain refers to any bodily pain experienced (from any and all causes) in the 4 weeks prior to interview, based on a 6-point scale ranging from ‘none’ to ‘very severe’. Participants were classified as experiencing pain if they indicated any bodily pain (ranging from ‘very mild’ to ‘very severe’).
Analysis does not include people for whom this measure was not applicable or not stated.
Psychological distress
Psychological distress refers to unpleasant feelings or emotions that affect a person’s level of functioning and interfere with the activities of daily living. This distress can result in having negative views of the environment, others and oneself, and manifest as symptoms of mental illness, including anxiety and depression.
Psychological distress is measured using the Kessler Psychological Distress Scale (K10), which involves 10 questions about negative emotional states experienced in the previous 4 weeks. The scores are grouped into Low/Moderate: K10 score 10–21 and High/Very high: 22–50.
Analysis does not include people for whom this measure was not applicable, not asked, or unable to be determined.
Disability
Disability or a restrictive long-term health condition exists if a limitation, restriction, impairment, disease or disorder has lasted, or is expected to last, for six months or more, which restricts everyday activities. In the current report, a person was classified as having disability, restriction or limitation if any limitation or restriction was indicated. This included those with either profound, severe, moderate or mild limitation in core activities (mobility, self-care and communication) or restriction in schooling or employment.
Those who indicated that they had no difficulties with school, study or work and had not identified any chronic conditions were identified as having 'no disability, limitation or restriction'.
Labour force participation
People were classified as either in the labour force or not in the labour force based the following criteria:
- In the labour force includes two groups:
- those working: employed people who reported that in the preceding week they had worked in a job, business or farm, or who had a job but were absent during that week
- those seeking work: people who were not employed but actively looking for work in the four weeks prior to the survey, and were available to start work in the week prior to the survey.
- Not in the labour force: those who were not employed or seeking work, including those who were retired, no longer working, do not intend to work in the future, are permanently unable to work, or have never worked and never intend to work.
Labour force participation was not examined in people aged 65 and over.
Calculating the prevalence of multimorbidity and complex multimorbidity types
Prevalence refers to the number or proportion of cases of a particular characteristic (e.g. a specific chronic condition), that are present in a population at one point in time. This differs from incidence, which refers to the number of new cases of a particular characteristic occurring within a certain period.
Prevalence estimates are provided for people of all ages with:
- no chronic conditions
- 1 chronic condition
- multimorbidity (2 or more chronic conditions).
Prevalence estimates are also provided for people aged 45 and over with:
- no chronic conditions
- 1 chronic condition
- multimorbidity (2 or more chronic conditions).
Multimorbidity is then split into 2 groups of people aged 45 and over with:
- non-complex multimorbidity (defined as 2 or more chronic conditions affecting no more than 2 body systems)
- complex multimorbidity (3 or more conditions affecting 3 or more body systems).
Complex multimorbidity is then further split into 2 groups:
- people with moderately complex multimorbidity (3–4 chronic conditions affecting 3 or more body systems)
- people with highly complex multimorbidity (5 or more chronic conditions affecting 3 or more body systems).
Multimorbidity
The first step in calculating the prevalence of total multimorbidity is to count the number of chronic conditions each person in the population has.
Once the number of chronic conditions have been counted, the number of people with 2 or more chronic conditions (multimorbidity) is divided by the number of people in the whole population of interest to calculate the prevalence of total multimorbidity in that population.
When calculating the prevalence of total multimorbidity, the body systems affected by the 10 conditions are not considered in the calculation. As a result, a person with arthritis and osteoporosis is assessed as having 2 individual conditions and therefore as having multimorbidity, even though arthritis and osteoporosis are both musculoskeletal conditions.
Complex multimorbidity
Multimorbidity is split into 2 groups; complex and non-complex multimorbidity. The prevalence of complex multimorbidity is based on counting the number of body systems affected, as well as the number of chronic conditions. Complex multimorbidity is defined as the co-occurrence of 3 or more chronic conditions affecting 3 or more different body systems (Harrison et al. 2014).
In contrast, non-complex multimorbidity exists where 2 or more chronic conditions occur together and affect no more than 2 body systems.
The ABS NHS condition classification is based on the International Classification of Disease (10th revision; ICD-10) (ABS 2019). Chapter axes within the ICD-10 include body systems, aetiology and ‘others’. For consistency with the coding of NHS condition information, ICD chapters have been used in this work as a proxy for body system, while acknowledging that all conditions in some groups cannot be attributed to the same body system, for example ‘all cancers’. See Table 3 for the grouping of chronic conditions by body systems based on ICD-10 chapters.
Complex multimorbidity types
In this analysis, complex multimorbidity is further divided into 2 groups: moderately complex multimorbidity and highly complex multimorbidity.
People with moderately complex multimorbidity are defined as having 3–4 chronic conditions affecting 3 or more body systems. Those with highly complex multimorbidity have 5 or more chronic conditions, affecting 3 or more body systems.
In addition to considering how conditions across different body systems affect a person with multimorbidity, these groups allow us to explore differences when a large number of chronic conditions are present.
|
ICD-10 chapter |
Chronic condition |
Inclusions |
|---|---|---|
|
Circulatory |
Selected cardiovascular diseases (heart, stroke and vascular disease) |
|
|
Endocrine, nutritional and metabolic |
Diabetes |
|
|
Genitourinary |
Chronic kidney disease |
|
|
Malignant neoplasms |
Cancer |
|
|
Musculoskeletal |
Arthritis
Back problems
Osteoporosis |
|
|
Psychological |
Mental and behavioural conditions |
|
|
Respiratory |
Asthma COPD |
|
Crude, age-standardised and age-specific estimates
Unadjusted (crude) weighted prevalence estimates provide important information on the actual level of multimorbidity in the population under study. However, unadjusted estimates do not account for differences in the age structure between populations and it is known that the risk of having a chronic disease varies with age. This may make comparisons across sub-populations (such as between males and females, or between people with no chronic conditions and those with multimorbidity) misleading if they have different age structures.
Variations in age structure between populations can be adjusted for by a statistical procedure called age-standardisation. This procedure applies the age-specific prevalence estimates observed in the study population to a single standard population. The overall rates that would then occur if the study population had the same age structure as the standard population can then be calculated and compared. This allows for different sub-populations to be compared on an equal age basis.
Age-standardised estimates have been reported in the section ‘Who has multimorbidity and what are their experiences’, where all people aged 18 and over are included in analysis. Age-standardised estimates are directly age-standardised to the Australian population as at 30 June 2001 using the age groups: 0–17, 18–24, 25–29, 30–34, 35–39, 40–44, 45–49, 50–54, 55–59, 60–64, 65–69, 70–74, 75+.
In the section ‘What are the types of multimorbidity and how common are they', crude estimates for people aged 45 and over are presented unless otherwise stated. Due to insufficient numbers of cases available to ensure the results of standardisation are robust for each group/measure compared, age-standardised results are not published. Age-standardised estimates were produced as part of this analysis however, and compared with crude estimates. In most cases, little difference was found between age-standardised and crude estimates. This suggests that age is not confounding the comparison of crude estimates in these instances and that crude prevalence estimates provide sufficient information for comparison.
Age-specific estimates for people aged 45–64 and 65 and over are included in Data tables 3.3b and 3.3c. Age-specific estimates can be used, in comparison with total crude estimates, to help understand how results may vary by age.
Identifying patterns of multimorbidity
Two approaches were used to identify different patterns of multimorbidity:
- identifying pairs of chronic conditions occurring together with high prevalence
- identifying pairs of chronic conditions occurring together at a higher prevalence than expected.
All analysis was performed using SAS Enterprise Guide version 7.1. SAS PROC SURVEYFREQ was used to produce weighted estimates for each combination of 2 of the 10 selected chronic conditions (45 combinations in total). Sample weights were included in the procedure to account for survey sample design in the calculation of estimates, and replicate weights included to adjust for design effects in the calculation of variance and errors. Analysis included all people surveyed aged 45 and over.
Detail on the analysis performed to identify these patterns is outlined in the following sections.
1. Identifying pairs of chronic conditions occurring together with high prevalence
SAS PROC SURVEYFREQ was used to produce observed weighted prevalence estimates for each combination of 2 of the selected chronic conditions. 95% confidence intervals for the observed prevalence estimate were calculated using the PROC SURVEYFREQ procedure.
2. Identifying pairs of chronic conditions occurring together at a higher prevalence than expected
Identifying pairs of conditions that co-occur in individuals at a higher than expected prevalence involves comparison of observed and expected prevalence estimates.
The observed prevalence of 2 conditions co-occurring is the actual prevalence calculated from the number of cases of the 2 conditions occurring together among individuals in the population. In this analysis, the observed prevalence of co-occurrence is estimated based on self-reported condition information collected through the NHS.
Any 2 conditions may occur in the same person by chance. The expected prevalence of 2 conditions co-occurring is the prevalence that we would expect to see if the 2 conditions occurred together purely by chance. When two conditions occur together by chance, their expected co-prevalence is the product of their individual prevalence estimates (prevalence of condition A * prevalence of condition B) under the assumption that the 2 conditions are independent of each other (van den Akker et al. 2001).
The ratio of observed to expected prevalence can be used to study multimorbidity (van den Akker et al. 2001). It is a measure of how much the observed prevalence differs from the expected prevalence. If the ratio is greater than 1, then there are more cases of the 2 conditions co-occurring than would be expected by chance alone. This ratio can be used to describe the strength of the association between co-occurring conditions (Norén et al. 2013), and is described this way in the current report.
The weighted number of expected events can be computed by the PROC SURVEYFREQ procedure under the null hypothesis that the row and column variables (the 2 conditions) are independent (SAS 2019). As the prevalence of many chronic conditions increases with age, age-adjusted estimates of expected condition co-occurrence were produced in order to account for differences in condition prevalence by age group. This was performed using SAS PROC SURVEYFREQ to produce weighted numbers of observed and expected events for each combination of 2 chronic conditions, by age group: 45–54, 55–64, 65–74 and 75 and over. Counts were then summarised across age groups to calculate the weighted age-adjusted expected number of events (E), along with the weighted observed number of events (O). These counts were used to calculate the age-adjusted ratio of observed to expected prevalence of the 2 conditions co-occurring where N is the number of people in the total population of interest:
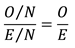
To identify pairs of conditions that co-occurred at a higher than expected prevalence, the age-adjusted ratio of observed to expected prevalence was assessed using a 95% confidence interval. If the lower limit of the 95% confidence interval is greater than 1, then the ratio is statistically significantly greater than 1. In such cases we can conclude that the number of cases of co-occurrence is greater than could be explained purely by chance and that there is a statistically significant association between the conditions.
The standard error (SE) of the estimated observed number of events is included in the output of the PROC SURVEYFREQ procedure. In order to take account of the variability arising from the sampling process and the survey design the SE is used to calculate the lower and upper limits of the 95% confidence interval around the observed number of events using the formulas:
Lower limit (OL) = O-1.96*SE
Upper limit (OU) = O+1.96*SE
The upper and lower limit are then substituted into the ratio, so the 95% confidence interval of the ratio of observed to expected prevalence is:
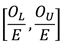
ABS (Australian Bureau of Statistics) 2019. National Health Survey: Users’ Guide, 2017–18. ABS cat. no. 4363.0.55.001. Canberra: ABS.
Department of Health 2019. Australia's Physical Activity and Sedentary Behaviour Guidelines and the Australian 24-Hour Movement Guidelines. Canberra: Department of Health. Viewed 19 November 2020.
Harrison C, Britt H, Miller G & Henderson J. 2014. Examining different measures of multimorbidity, using a large prospective cross-sectional study in Australian general practice. BMJ Open 4(7): e004694.
Norén GN, Hopstadius J & Bate A 2013. Shrinkage observed-to-expected ratios for robust and transparent large-scale pattern discovery. Statistical Methods in Medical Research 22(1): 57–69.
NHMRC (National Health and Medical Research Council) 2020. Australian guidelines to reduce health risks from drinking alcohol. Canberra: NHMRC.
SAS 2019. The SURVEYFREQ procedure. Viewed 23 November 2019.
Van den Akker M, Bunntinx F, Roos S & Knottnerus JA 2001. Problems in determining occurrence rates of multimorbidity. Journal of Clinical Epidemiology 54(7): 675–9.


