Major model category
Each maternity model of care in the Model of Care National Best Practice Data Set (MoC NBPDS) is grouped into one of 11 major model categories, based on its specific characteristics. The 11 different categories broadly describe the intent of the model of care, although not all women in a model of care will necessarily follow the same journey or receive the same care pathway as the model intends (or was designed for). See Major model category definitions.
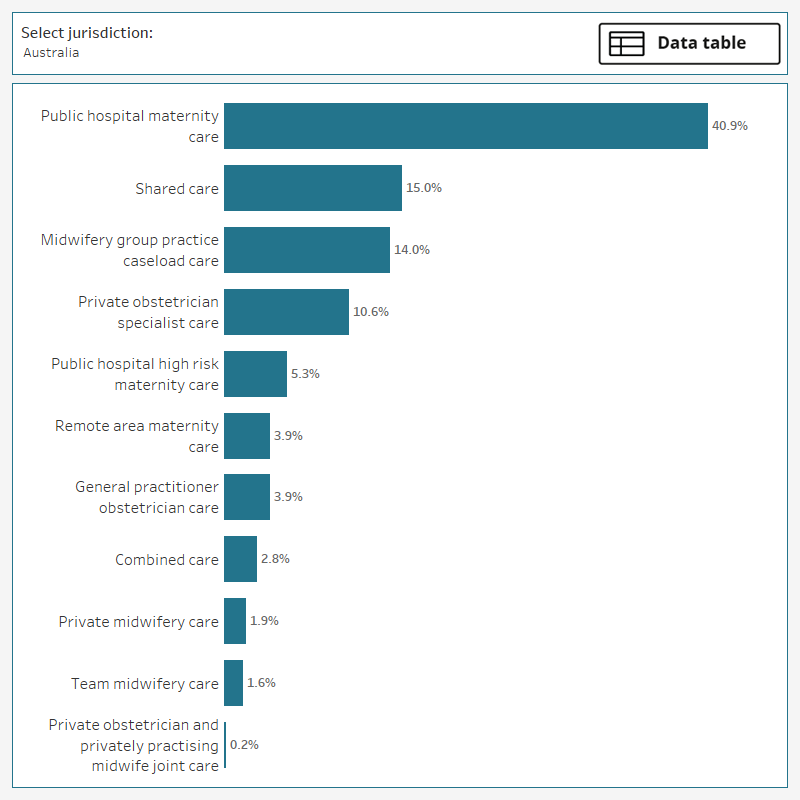
The most common major model category is public hospital maternity care with 41% of models of care falling into this category. This is followed by shared care (15% of models), midwifery group practice caseload care (14% of models), and private obstetrician specialist care (11% of models). Public hospital high risk maternity care is the model category for around 5.3% of models. Other, less common models include general practitioner (GP) obstetrician care (3.9%), combined care (2.8%), private midwifery care (1.9%) and team midwifery care (1.6%).
It is important to note there may still be differences between models of care with the same major model category. Public hospital maternity care is the model category with the most variation (Donnolley et al 2017). It broadly describes a model of care where antenatal care is provided by midwives and/or doctors in onsite or outreach clinics. Intrapartum (labour and birth) and postnatal care is provided in hospital by midwives in collaboration with doctors as needed. This category is used to describe models that cover a range of clinics, from those run by midwives that target low risk women, to those led by public specialist obstetricians for women with obstetric complexities such as gestational diabetes, multiple pregnancy, or next birth after caesarean section. Around three-quarters (76%) of models classified as public hospital maternity care target a specific group of women, compared with 63% of models overall.
In contrast, models classified as midwifery group practice caseload care have less variation. This category describes models where antenatal, intrapartum, and postnatal care are provided within a publicly funded caseload model by a known primary midwife, with secondary backup midwives providing cover and assistance, and collaboration with doctors in the event of identified risk factors. Antenatal care and postnatal care are usually provided in the hospital, community, or home with intrapartum care in a hospital, birth centre or home. This model category, by definition, has a public midwife as the designated carer and continuity of carer for the whole duration of maternity care. It is also more likely to target low risk or normal pregnancy (35%, compared with 19% overall) and to provide residential postnatal care (100%, compared with 75% overall).
A shared care model category describes models of care where antenatal care is provided by a community maternity service provider (doctor and/or midwife) in collaboration with hospital medical and/or midwifery staff, under an established agreement. It can occur in the community and in hospital outpatient clinics. This would usually include an agreed schedule of antenatal care between the 2 providers. Intrapartum and early postnatal care usually takes place in the hospital, by hospital midwives and doctors, often in conjunction with the community doctor or midwife (particularly in rural settings). Just over half (54%) of models of care in this category target a specific group of women, compared with 63% overall, and 28% have a target group of low risk or normal pregnancy.
Public hospital maternity care is the most common model category in all states and territories, except the Northern Territory where shared care (25% of models) and remote area maternity care (25% of models) are more common. Queensland and South Australia have a relatively high proportion of models of care classified as midwifery group practice caseload care (24% and 21%, respectively).
The data visualisation below (Figure 2) shows maternity models of care by their major model category. Select the drop-down menu to filter by jurisdiction (state or territory). Use the button to access the data table.
Figure 2: Proportion of models of care, by major model category, Australia, 2023
The bar chart shows that public hospital maternity care is the most common model category in Australia (representing 41% of maternity models of care).
Notes
- Analyses are based on the models of care being used by maternity services with birthing facilities that were classified in the MoC NBPDS in June 2023.
- Some model categories are not represented in some jurisdictions. This is because health system structures and care frameworks differ between jurisdictions. There may also be a small number of models of care that are not included because they have not yet been classified by maternity services or are state-wide models of care that do not sit under a specific service.
Source: AIHW analysis of the MoC NBPDS.
References
Donnolley NR, Chambers GM, Butler-Henderson KA, Chapman MG & Sullivan EA 2017. 'More than a name: Heterogeneity in characteristics of models of maternity care reported from the Australian Maternity Care Classification System validation study'. Women and Birth 30(4): 332–341. doi:10.1016/j.wombi.2017.01.005


