NMHSPF model
The National Mental Health Service Planning Framework (NMHSPF) model brings together the best available evidence and expert opinion on:
- the prevalence of mental illness and need for mental health services,
- the types and levels of mental health care required for different need groups, and
- efficient standards of health service operation to deliver this care.
Based on this information, the model determines the resources required to deliver adequate mental health services to specific population groups. These groups include a nominal population of 100,000 people for each age group, or selected population regions such as Australia, a state or territory, Local Hospital Networks or Primary Health Networks.
The NMHSPF model outlines how many people need mental health care (epidemiology), the types of services needed (taxonomy) and the volume of specific services required (care profiles and top-ups) by different groups of people.
This is combined with information on service staffing (workforce and funder type) and operations (modelling parameters) to produce resource targets such as the number of hospital beds required.
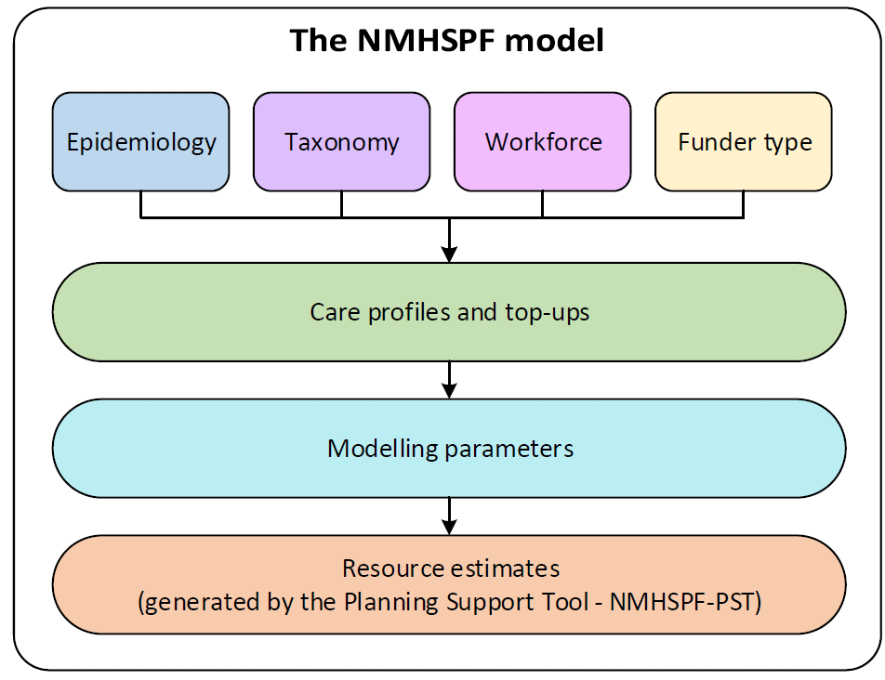
Chart: The University of Queensland
Source: Introduction to the NMHSPF V4.3
Epidemiology
The NMHSPF starts with classifying the Australian average population into ‘need groups’. Need groups are based on severity of mental health diagnosis or other identified mental health need, and functioning.
The epidemiology estimates the number of people within each need group who may require mental health services in a year, by age and level of severity. It sets service demand targets for those who require intervention.
The video below provides more information about the scope, definition of a need group, data sources, severity, demand for services and other additional factors. Detailed information is also available in the Support material section.
Video: Need for mental health services
Service and resource descriptions
Service and resource descriptions are essential to needs-based mental health planning. The model brings together epidemiology and care profiles to determine resource requirements to deliver adequate mental health care to Australia’s population. More information is provided within the video below and in the Support material section.
Video: Service and resource descriptions in the NMHSPF
Taxonomy
The NMHSPF describes the range of services required within a comprehensive mental health system, from self-help and digital treatments to specialist clinical care.
It uses an agreed national taxonomy of mental health services defining the range of service delivery, within 6 key streams. Each stream is further subdivided into service categories, service elements and activities. The 6 service delivery streams are:
- mental health promotion,
- mental illness prevention,
- primary and specialised clinical ambulatory mental health services,
- specialised mental health community support services,
- specialised bed-based mental health care services, and
- medications and procedures.
As each state and territory structures their mental health services differently, the taxonomy provides a common language and clear definitions of core mental health service components and functions.
Care profiles and top-ups
Care profiles are associated with specific need groups within each age group defined under the NMHSPF.
Care profiles bring together service elements and activities from the taxonomy, workforce categories and modelling parameters to describe the average type and quantity of mental health care needed for each need group over a 12-month period.
For each service element, the care profile specifies the proportion of the need group likely to require that service. It also includes the average number of times the service will be required, the average duration for each service, workforce and funder type.
There are also resource top-ups for services that are required by a range of unspecified people across need groups, for example, emergency department services. Across the 6 age groups, the NMHSPF defines 116 need groups, 45 of which are top-ups.
Watch the video for more information about care profiles for specific groups and top-ups for non-discrete groups.
Video: Care profiles and top-ups
Modelling parameters
The NMHSPF model estimates resources such as the number of beds or staff required based on a range of measures within each taxonomy item and workforce type.
This includes the workforce mix for team-based services and modelled operational parameters such as occupancy and annual readmission rates for bed-based services, staff working hours, staff salaries, salary on costs and overhead costs. NMHSPF parameters for each service element are modelled at desirable, efficient operational rates. Outputs are based on averaged national staffing profiles and salaries.
Funder type
The NMHSPF model considers the service functions required to meet the needs of people with mental illness, rather than service location, format or provider.
The NMHSPF Planning Support Tool (NMHSPF-PST) generates resource estimates by funder by drawing on default funder types that are applied to each service element in the care profiles. This helps planners identify areas of responsibility within the modelled benchmarks.
Funder types represent a national average of current services rather than an optimal model. It designates the entity with primary funding and administrative oversight for each aspect of the NMHSPF.





