Health is not the same for everyone
Health changes throughout our lives and also differs within population groups.
This section looks at health for selected life stages—such as infancy, young adulthood and among the very old—and also highlights some of the health inequalities faced by people in low socioeconomic groups; Aboriginal and Torres Strait Islander Australians; people living in regional and remote areas; and Australians with disability.
Many factors affect health during pregnancy
Many factors—such as a mother's age and where she lives; her access to antenatal care; and whether she smokes, drinks alcohol or is obese during pregnancy—influence health outcomes for her and for her baby.
In 2013, nearly all mothers had antenatal care at some point in their pregnancies, but women from the lowest socioeconomic areas, Aboriginal and Torres Strait Islander people, and mothers who were born overseas tended to begin antenatal care later in pregnancy and had fewer visits overall.
Around 1 in 8 (12%) expectant mothers smoked at some time during pregnancy in 2013, which was less than the 15% who did so in 2009.
Some mothers were more likely to smoke during the first 20 weeks of their pregnancy than others:


In 2013, more than half (56%) of pregnant women consumed some alcohol before they knew they were pregnant and about 1 in 4 (26%) of these women continued to drink after they found out about their pregnancy. Most pregnant women drank monthly or less often, usually consuming 1-2 standard drinks.
Not all babies have the same start
Around 309,000 babies were born in 2013, but not all babies have the same start to life.
Factors such as a baby's gestational age and birthweight can influence their chance of survival and their health outcomes. The proportion of low birthweight babies was higher among:
female babies (6.9%) compared with male babies (5.9%)
twins (56%) and other multiples (98%) compared with singletons (4.8%)
babies of Aboriginal and Torres Strait Islander mothers (12.2%) compared with babies of non-Indigenous mothers (6.1%)
babies whose mothers smoked during pregnancy (12%) compared with babies whose mothers did not smoke (5.7%)
In 2012, Australia had a slightly lower proportion of low birthweight babies than the OECD average (6.2% compared with 6.6%, respectively), ranking in the middle third of all OECD countries. We also rank in the middle third for our infant mortality rate.
Mixed news for children
The early years of a child's life provide the foundation for future heath, development and wellbeing. Good health during childhood can influence participation in many aspects of life, including education, recreation and relationships.
Many factors affect health in childhood, including overweight and obesity and physical activity.
In 2014-15, about two-thirds (68%) of Australian children aged 5-14 were in the normal weight range, 19% were overweight and 7% were obese.
In 2011-12, fewer than one-quarter (23%) of Australian children aged 5-14 met the national physical activity recommendations every day (at least 60 minutes of moderate to vigorous intensity physical activity).
The most common long-term conditions in children are asthma and allergic rhinitis (hay fever).
In 2014-15, just over 1 in 10 (11%) of children were diagnosed with asthma. In 2014-15, the prevalence of allergic rhinitis (hay fever) was also 11%.
Internationally, Australian girls rank in the worst third out of 33 OECD countries for overweight/ obesity rates, and boys are in the middle third.
...and for teenagers and young adults
Substantially fewer young people aged 15-24 are smoking now, with daily smokers almost halving—from 21% in 2001 to 11% in 2013.
The leading cause of death for young people aged 15-24 in 2011-13 was suicide (11 per 100,000).
In 2013-14, there were more than 80,000 hospitalisations (2,572 per 100,000) of young people due to injury and poisoning.
The most common cause of hospitalisation for females aged 15-24 was intentional self-harm (410 per 100,000), while this ranked 8th for males in the same age group (147 per 100,000). Males were most likely to be hospitalised for transport accidents (613 per 100,000).
Very old Australians in good health or better
Improvements in life expectancy have resulted in a growing number of Australians in the 'very old' age group. Today, nearly half a million Australians are aged 85 and over, and this number is expected to more than double to 1 million over the next 20 years.
The majority (65%) of Australians in this age group consider themselves to be in 'good', 'very good' or 'excellent' health, and 9.0% reported 'high' or 'very high' levels of psychological distress—the lowest rate in any age group.
The three most common health conditions reported by people aged 85 and over in 2014-15 were long-sightedness (61%), deafness (57%) and arthritis (49%).
As with younger age groups, common risk factors for the older age group include being overweight (39%) or obese (18%), and not doing any physical activity (45%), and only 6.2% of people aged 85 and over eat adequate serves of fruit and vegetables each day.
However, fewer than 4.0% of people aged 85 and over were daily smokers in 2013, compared with 13% of all adults.
Socioeconomic disadvantage associated with poorer health
People living in the lowest socioeconomic areas are more likely to have poor health and to have higher rates of illness, disability and death than people who live in the highest socioeconomic areas. If all Australians had the same death rates as the 20% of Australians living in the highest socioeconomic area, there would have been about 54,200 fewer deaths in 2009-2011.
Adults living in the lowest socioeconomic areas are more likely than adults living in the highest socioeconomic areas to have:
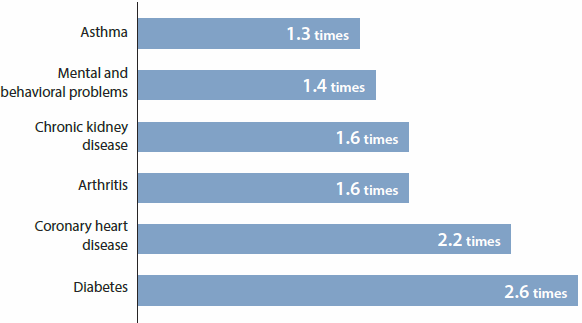
Rates of potentially avoidable deaths were also 1.8 times higher in the lowest socioeconomic areas than in the highest socioeconomic areas.
Progress in Indigenous health, but still room to improve
There have been some improvements in Aboriginal and Torres Strait Islander health in recent years, including decreases in smoking and infant mortality and in avoidable deaths from circulatory and kidney diseases. However, there is still a significant gap in health outcomes, including life expectancy at birth, between Indigenous and non-Indigenous Australians. The causes of this gap are complex, and include differences in the social determinants of health, risk factors, and access to appropriate health care.
The size of the health gap
Compared with the non-Indigenous population, Indigenous Australians:
- have a lower life expectancy—the gap is 10.6 years for males and 9.5 years for females
- are 3.5 times as likely to have diabetes and 4 times as likely to be hospitalised with it or to die from it
- are 5 times as likely to have end-stage kidney disease
- are twice as likely to die from an injury and 1.9 times as likely to be hospitalised with an injury
- are twice as likely to have coronary heart disease.
Indigenous Australians have higher prevalence of risk factors
The prevalence of major health risk factors, such as smoking and physical inactivity, is generally higher for Indigenous Australians than for other Australians.
While the smoking rate for Indigenous Australians declined from 51% in 2002 to 44% in 2012-13, they were still 2.6 times as likely to smoke daily as non-Indigenous Australians (15%).
In 2012-13, after adjusting for differences in the age structure, for those living in non-remote areas, Indigenous adults were more likely than non-Indigenous adults to not have undertaken the recommended level of physical activity in the last week (64% compared with 56%).
Obesity was also more common among Indigenous Australian adults aged 18 and over. After adjusting for differences in age structure, Indigenous adults were 1.6 times as likely to be obese as non-Indigenous adults (43% compared with 27% for non-Indigenous adults in 2012-13).
Health declines with distance
In 2013, 29% of the Australian population lived in regional and remote areas: 18% in Inner regional areas, 8.9% in Outer regional areas, 1.4% in Remote areas and 0.9% in Very remote areas. Australians living outside Major cities tend to have higher rates of disease and injury than people in Major cities, and they are also more likely to engage in health behaviours that can lead to adverse health outcomes.
| Areas | Arthritis | Diabetes | Cardiovascular Disease |
Mental health conditions |
Current daily smoker |
No/low levels of exercise |
Lifetime risky drinking |
|---|---|---|---|---|---|---|---|
Major cities |
14% | 4.7% | 4.7% | 17% | 13% | 64% | 16% |
Inner regional |
20% | 6.0% | 6.7% | 19% | 17% | 70% | 18% |
Outer regional/ Remote |
18% | 6.7% | 5.8% | 19% | 21% | 72% | 23% |
Disability adds to health inequality
Just under 1 in 5 Australians (4.2 million people) reported having a disability in 2012.
People with disability experience significantly poorer health than people without disability. Over half (51%) of people aged 15-64 with severe or profound limitation(s) in communication, mobility or self-care reported 'poor' or 'fair' health compared with 5.6% of those without such limitations.
A higher proportion of people aged 15-64 with these limitations had mental health conditions (50% compared with 7.7% for those without). They were also more likely to:
- be obese (43% versus 25%)
- report doing no physical exercise (46% versus 31%)
- smoke daily (31% versus 15%)
- report a very high level of psychological distress (22% versus 1.2%).



