Technical notes
The main source of information for this web report is the AIHW’s Disease Expenditure Database. It contains estimates of spending by Australian Burden of Disease Study condition, age group, and sex for admitted patient, emergency department, and outpatient hospital services, out-of-hospital medical services, and prescription pharmaceuticals.
The methods used for estimating disease spending is a mixture of ‘top-down’ and ‘bottom-up’ approaches, where total spending across the health system is estimated and then allocated to the relevant conditions based on the available service use data.
Although this approach produces consistency, good coverage and totals that add up to known expenditure, it is not as comprehensive for any specific disease as a detailed ‘bottom-up’ analysis, which would include the actual costs incurred for that disease. A lack of amenable data sources means that a more granular ‘bottom-up’ analysis is not possible.
Estimates in the Disease Expenditure Database have been derived by combining information from the:
- National Hospital Morbidity Database (NHMD)
- National Public Hospitals Establishments Database (NPHED)
- National Non-admitted Patient Emergency Department Care Database (NNAPEDC)
- National Non-admitted Patient Databases (aggregate, NAPAGG, and unit record, NAPUR)
- National Hospital Costs Data Collection (NHCDC)
- Private Hospital Data Bureau (PHDB) collection
- Bettering the Evaluation and Care of Health (BEACH) surv
- Medicare Benefits Schedule (MBS)
- Pharmaceutical Benefits Scheme (PBS)
- Health Expenditure Database.
It is not technically appropriate or feasible to allocate all spending on health goods and services by disease. For example, neither administration expenditure nor capital expenditure can be meaningfully attributed to any particular condition due to their nature. For the purposes of this report, $134 billion, or 72% of recurrent spending, was attributed to specific diseases and injuries. This expenditure includes payments from all sources of funds, such as the Australian and State and Territory Governments, Private Health Insurance, and out of pocket payments by patients.
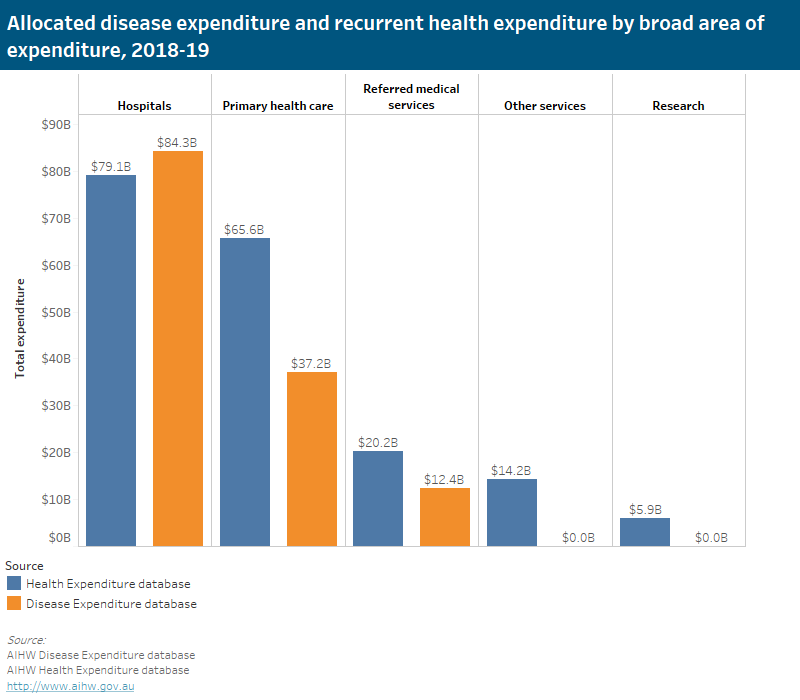
Some components of recurrent expenditure are allocated differently between the health expenditure Australia database, and the disease expenditure study. This approach was taken to reflect patterns of healthcare use for particular conditions, which is the focus of this body of work, rather than health funding arrangements. Spending estimates in hospitals are slightly higher than in the Health Expenditure Database, while spending on referred medical services are lower. This is discussed further in the Disease Expenditure 2018–19 Study: Overview of analysis and methodology report.
Figure D1 comparison HEA-DEX: Allocated disease expenditure and recurrent health expenditure by broad area of expenditure, 2018-19. This bar chart shows allocated and recurrent expenditure by broad area of expenditure in 2018-19 in the Health Expenditure and Disease Expenditure databases. Total recurrent health expenditure in 2018-19 was $ 185 billion in the Health Expenditure database, 72.43% ($134 billion) of which was able to be attributed to specific diseases and injuries. Approximately 63% of this allocated spending was related to hospital services, 28% ($37.2 billion) related to primary health care, and 9% ($12.4 billion) related to referred medical services, as opposed to these categories accounting for 43% ($79.1 billion), 35% ($65.6 billion), and 11% ($20.2 billion) of total recurrent spending, respectively.
Expenditure information is added to hospital activity data for every admitted patient record in the NHMD, all emergency department presentations in the NNAPEDC, and all service events in the National Non-admitted Patient Databases. Data sets have been constructed for all private hospital admitted patient separations. Aggregated data sets by sex, age group, state/territory and SA3 geographical area, including patient copayments, have been created for MBS services by provider specialty and subgroup, and pharmaceuticals by Anatomical Therapeutic Classification (ATC). All of the data sets include expenditure estimates for each ABDS condition.
The AIHW continually seeks to improve the methods used to produce these estimates. Estimates for the disease expenditure are subject to revision. Hence the most recently published results are not directly comparable with previously published data.
The February 2022 update incorporates the following additional changes: a revised mapping of ICD-10 codes to ABDS conditions for the kidney and urinary diseases group; an updated mapping file used to map MBS item numbers to ABDS; updated 2018–19 data reported in Health expenditure Australia 2019–20.


