Caesarean section
Caesarean section describes a method of birth in which the baby is removed directly from the uterus through an incision in the mother’s abdomen. This procedure is generally performed when vaginal birth is likely to pose a risk to the health of the mother or baby, or in scenarios such as stalled labour or unsuccessful vaginal birth. For more information, see Clinical commentary.
This indicator looks at caesarean section for selected women giving birth for the first time.
Key findings
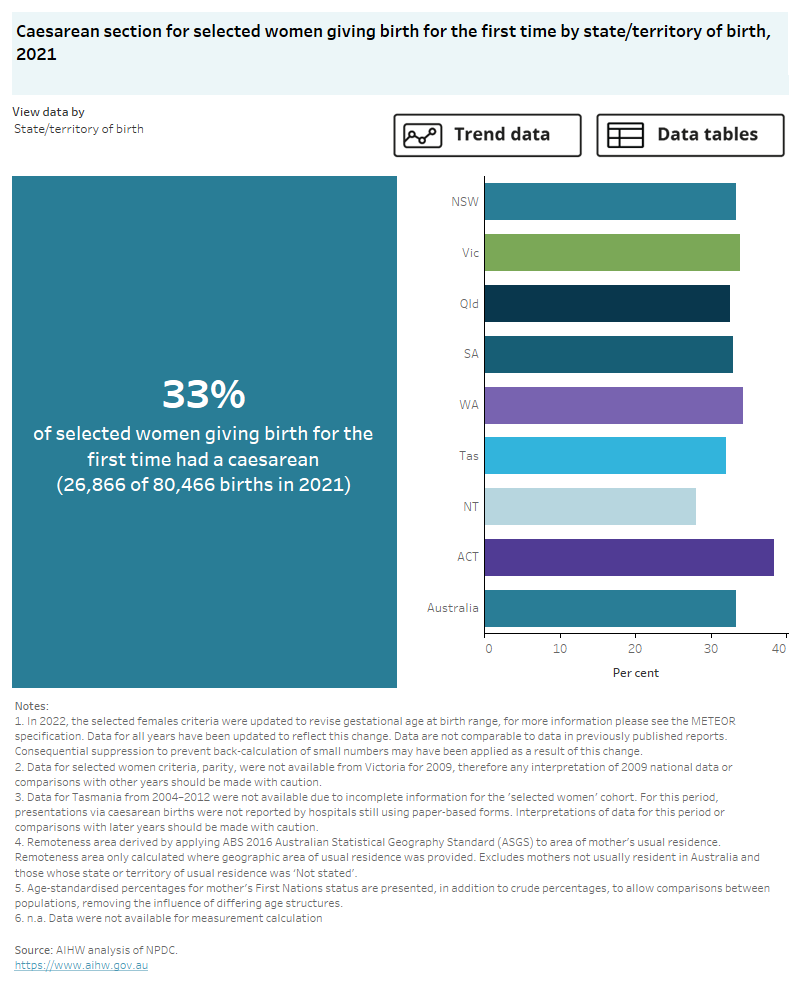
In 2021, one third (33%) of selected women giving birth for the first time had a caesarean section.
The proportion of selected women giving birth for the first time having a caesarean section birth:
- increased from 1 in 4 women (25%) in 2004, to 1 in 3 (33%) in 2021
- was higher in private hospitals than in public hospitals (43% compared with 29% in 2021)
- was slightly higher for women living in areas of least disadvantage (35% in 2021) than for women living in areas of most disadvantage (32% in 2021).
The interactive data visualisation (Figure 7) presents data on caesarean section for selected women giving birth for the first time by selected maternal characteristics. Select the trend button to see how data have changed between 2004 and 2021.
Figure 7: Caesarean section
Caesarean section for selected women giving birth for the first time, 2004 to 2021.
This chart shows the proportion of women receiving a caesarean section for selected women giving birth for the first time, for the current data 2021 and trend data from 2011 to 2021. The proportion for selected women giving birth for the first time receiving a caesarean section increased from 25% in 2004 to 33% in 2021.
Clinical commentary
A caesarean section is an operation where a baby is born through an incision made through the mother’s abdomen and the uterus (RANZCOG 2021). A caesarean section may be planned (elective), or unplanned (emergency) if complications develop and delivery needs to be hastened.
Caesarean section is one of the most common interventions in pregnancy and is safer now than in the past, however, a small risk of serious morbidity and mortality for both the mother and the baby remains and the benefits need to be weighed against the risks (ACSQHC 2018; Betran et al. 2016; Villar et al. 2007; Keag et al. 2018). Risks to the mother include postoperative infection, haemorrhage, and complications during future pregnancies. Risks to the baby for planned caesarean section at less than 39 weeks' gestation can include increased rates of neonatal respiratory issues, asthma, obesity and developmental issues (ACSQHC 2018).
Caesarean section rates have increased steadily worldwide over the last decades (WHO 2018, OECD 2019) however this trend has not been associated with significant maternal or perinatal benefits (WHO 2015). Caesarean section rates have increased across most OECD countries, from an average of 20% in 2000 to 28% in 2017. In 2021, 38% of all women giving birth in Australia had a caesarean section (AIHW 2023). The WHO states that at the population-level, caesarean section rates higher than 10% are not associated with reductions in maternal and newborn mortality rates (WHO 2015). The WHO also states that caesarean sections are effective at saving lives when required for medically indicated reasons, and every effort should be made to provide caesarean sections to women in need, rather than striving to achieve a specific rate (WHO 2015). The increasing rates of caesarean sections may be influenced by a number of maternal and clinical factors and medico legal concerns, however, the reasons for the steep rise remain unexplained. Besides this general increase in caesarean section, a large variation between countries, regions and hospitals has been documented (OECD 2019, Betran et al. 2016; Bragg et al. 2010; Librero et al. 2000).
Whether the operation is a planned elective procedure or an unplanned emergency procedure, receiving clear information on the benefits of the operation and the short and long-term risks is important to enable an informed decision as to whether to proceed with the caesarean section or not.
More information on caesarean section for all women giving birth can be found in Australia’s mothers and babies.
Indicator specifications and data
Excel source data tables are available from Data.
For more information refer to Specifications and notes for analysis in the technical notes.
ACSQHC (Australian Commission on Safety and Quality in Health Care) (2018) The second Australian atlas of healthcare variation, accessed 2 March 2023.
AIHW (Australian Institute of Health and Welfare) (2023) Australia’s mothers and babies, AIHW, Australian Government, accessed 29 June 2023.
Betran A, Ye J, Moller A, Zhang J, Gülmezoglu A and Torloni M (2016) ‘The increasing trend in caesarean section rates: global, regional and national estimates: 1990–2014’, Public Library of Science, 11(2):e0148343, doi:10.1371/journal.pone.0148343.
Bragg, F, Cromwell DA, Edozien LC, Gurol-Urganci I, Mahmood TA, Templeton A and van der Meulen JH (2010) ‘Variation in rates of caesarean section among English NHS trusts after accounting for maternal and clinical risk: cross sectional study’, British Medical Journal, 341:c5065, doi:10.1136/bmj.c5065.
Keag O, Norman J and Stock S (2018) ‘Long-term risks and benefits associated with cesarean delivery for mother, baby, and subsequent pregnancies: Systematic review and meta-analysis’, Public Library of Science: Medicine, 15(1): e1002494, doi:10.1371/journal.pmed.1002494.
Librero J, Peiro S and Calderon SM (2000) ‘Inter-hospital variations in caesarean sections. A risk adjusted comparison in the Valencia public hospitals’, Journal of Epidemiology and Community Health, 54:631-636, doi:10.1136/jech.54.8.631.
OECD (Organisation for Economic Co-operation and Development) (2019) Health at a glance 2019: OECD indicators, OECD Publishing, Paris, accessed 6 June 2023.
RANZCOG (Royal Australian and New Zealand College of Obstetricians and Gynaecologists) (2021)Caesarean section, accessed 17 August 2022.
Villar J, Carroli G, Zavalenta N, Donner A, Wojdyla D, Faundes A et al. (2007) ‘Maternal and neonatal individual risks and benefits associated with caesarean delivery: multicentre prospective study’, British Medical Journal, 335:1025, doi:10.1136/bmj.39363.706956.55.
WHO (World Health Organization) (2015) WHO statement on caesarean section rates, WHO, Geneva, accessed 20 March 2023.
WHO (World Health Organization) (2018) WHO recommendations: non-clinical interventions to reduce unnecessary caesarean sections, WHO, Geneva, accessed 20 March 2023.


