Data sources
The AIHW National Mortality Database (NMD) contains records for deaths in Australia from 1964 to 2022. The database comprises information about causes of death and other characteristics of the person, such as sex, age at death, area of usual residence and Indigenous status.
The AIHW sources causes of deaths data from the Registries of Births, Deaths and Marriages in each state and territory and the National Coronial Information System (managed by the Victorian Department of Justice). The cause of death data are compiled and coded by the Australian Bureau of Statistics (ABS) to the International Statistical Classification of Diseases and Related Health Problems (ICD) and maintained at the AIHW in the NMD. Registration of deaths is the responsibility of the Registry of Births, Deaths and Marriages in each state and territory.
To improve the quality of data, the ABS annually revises the causes of death for coroner-referred deaths to reflect the latest available information. This process applies to deaths registered after 1 January 2006. Deaths registered between 2006 and 2019 are finalised. Deaths registered in 2020 are revised, deaths registered in 2021 are preliminary revised, and 2022 registered deaths are preliminary. Revised, preliminary revised, and preliminary data are subject to further revision by the ABS. For a more detailed description of the coverage and processing of deaths data, including deaths certified by the coroner, refer to the ABS Causes of death, Australia methodology, Australia (ABS Catalogue No. 3303.0).
In the NMD, the year the death occurred, the year the death was registered with the state and territory registry, and the in scope year the death was lodged with the ABS (ABS reference year) are provided. Year of registration has been used for the purposes of monitoring deaths by suicide. Deaths based on the year the death occurred have also been presented; however, as some deaths at the end of each calendar year may not be registered until the following year, year of death information for the latest available year (2022) is generally an underestimate of the actual number of deaths that occurred in that year. While not as significantly impacted, it should be noted that latest data by year of registration is also an underestimate and subject to revision.
In more recent years, there have been occasions where the ABS has received a large number of deaths, which were registered in Victoria in earlier years. For detailed information on this issue, see Technical Note: Victorian additional registrations and time series adjustment and Technical Note: Victorian additional registrations (2013-2016).
Deaths (such as those from suicide) that are referred to a coroner can take time to be fully investigated, which can influence what information is available to assign a cause of death code during the ABS coding process. Each year, some coroner cases are coded by the ABS before the coronial proceedings are finalised. Coroner cases that have not been closed or had all information made available can impact on data quality as less specific ICD-10 codes often need to be applied. At the time of coding both 2021 and 2022 data there was a higher proportion of open coroner cases at preliminary coding than seen in previous years (67.2% in 2021 versus and 65.2% in 2022 versus a 5-year average for 2015-2019 of 56.2%). This is reflected in the 2021 and 2022 preliminary datasets by a higher rate of deaths due to 'other ill-defined and unspecified causes of mortality' (R99). In consideration of this, the ABS conducted an early revision of 2021 coroner certified deaths that had ill-defined causes. Therefore, data for 2021 are now considered preliminary revised. The ABS will apply the full revisions process for 2021 data and an early revision of 2022 data during the 2024 revisions cycle.
It is expected that deaths due to intentional self-harm will increase through the revisions process. For further information surrounding the revisions process, see Coding of suicide in the Deaths on the ABS Causes of Death, Australia, 2022 methodology page.
The data quality statements underpinning the AIHW NMD can be found on the following ABS internet pages:
- ABS Quality declaration summary for Causes of death, Australia methodology (ABS cat. no. 3303.0).
- ABS Quality declaration summary Deaths, Australia
For more information on the AIHW NMD see National Mortality Database and About National Mortality Database.
Quality of Indigenous status data
The Indigenous status of a deceased person is captured through the death registration process; however, it is recognised that not all such deaths are captured through these processes, leading to under-identification. The Aboriginal and Torres Strait Islander (First Nations) origin of a deceased person is noted on the Death Registration Form (DRF) and the Medical Certificate of Cause of Death (MCCD).
For 2022 for New South Wales, information from the MCCD has been used for the first time. Using both sources (the DRF and MCCD) resulted in a greater proportion of deaths of First Nations origin, compared to 2021. This change has introduced a break in time series in First Nations death statistics in NSW and Australia. Therefore caution should be used when making comparisons with previous years. For more information on this change and the impacts refer to the Technical Note: The impact of using two sources for deriving the Indigenous status of deaths in NSW in 2022.
Data on deaths by suicide in Indigenous people have been compiled by jurisdiction of usual residence for New South Wales, Queensland, Western Australia, South Australia and the Northern Territory only. Data for Victoria, Tasmania and the Australian Capital Territory have been excluded in line with national reporting guidelines.
Data for patients who were hospitalised with intentional self-harm injuries are sourced from the AIHW’s National Hospital Morbidity Database (NHMD). Most of the data used for the monitoring of hospitalisations for intentional self-harm are from 2008–09 to 2021–22. For each reference year, the NHMD includes all hospitalisations for patients who were discharged between 1 July and 30 June.
The NHMD is a compilation of episode-level records from admitted patient morbidity data collection systems in Australian hospitals. It is a comprehensive data set that has records for all episodes of admitted patient care from essentially all public and private hospitals in Australia.
The data supplied are based on the National Minimum Data Set (NMDS) for Admitted Patient Care and include administrative, demographic, clinical and length of stay data, as well as data on the diagnoses of the patients, the procedures they underwent in hospital and external causes of injury and poisoning.
The purpose of the NMDS for Admitted Patient Care is to collect information about care provided to admitted patients in Australian hospitals. The scope of the NMDS includes episodes of care for admitted patients in all public and private acute and psychiatric hospitals, free standing day hospital facilities, and alcohol and drug treatment centres in Australia. Hospitals operated by the Australian Defence Force, corrections authorities and in Australia’s off-shore territories are not in scope but may be included. Hospitals specialising in dental, ophthalmic aids and other specialised acute medical or surgical care are included.
episode of care: The period of admitted patient care between a formal or statistical admission and a formal or statistical separation, characterised by only one care type (see care type and separation). METeOR identifier: 268956.
separation: The process by which an episode of care for an admitted patient ceases. A separation may be formal or statistical. METeOR identifier: 327268.
formal separation: The administrative process by which a hospital records the cessation of treatment and/or care and/or accommodation of a patient.
statistical separation: The administrative process by which a hospital records the cessation of an episode of care for a patient within the one hospital stay.
The criteria used to describe intentional self-harm hospitalisations reported in Suicide & self-harm monitoring is described in the Codes and classifications section.
Data limitations
States and territories are primarily responsible for the quality of the data they provide. However, the AIHW undertakes extensive validations on receipt of data, checking for valid values, logical consistency and historical consistency. Where possible, data in individual data sets are checked with data from other data sets. Potential errors are queried with jurisdictions, and corrections and resubmissions may be made in response to these queries. Except as noted, the AIHW does not adjust data to account for possible data errors or missing or incorrect values.
The most recent Data quality statement for Admitted Patient Care is available in METeOR. The Data Quality Statement contains information on other changes that may affect interpretation of the data for the relevant year.
Quality of Indigenous status data
The Indigenous status data in the NHMD for all states and territories are considered to be of sufficient quality for statistical reporting. In 2011–12, an estimated 88% of Indigenous patients were correctly identified in public hospitals (AIHW 2013). The overall quality of the data provided for Indigenous status needs some improvement and varied between states and territories. It is unknown to what extent Indigenous Australians might be under-identified in private hospital admissions data.
The National Ambulance Surveillance System (NASS) is a public health monitoring system, which aims to provide timely and comprehensive data on intentional self-harm (including suicidal behaviours with self-injurious intent), mental health, and alcohol and drug harms in the community. Data for the National Ambulance Surveillance System (NASS) are compiled by Turning Point in partnership with Monash University and are sourced from paramedic electronic patient care records provided by Australian state and territory-based ambulance services in New South Wales, Victoria, Queensland, Tasmania, and the Australian Capital Territory. As part of the National Suicide and Self-harm Monitoring Project, the AIHW has contracted Turning Point through Monash University to develop and maintain the National Ambulance Surveillance System (NASS) for self-harm related ambulance attendances. Self-harm (suicidal ideation, suicide attempt, self-injury) related modules from the NASS are reported here.
Information is obtained and coded through manual scrutiny of de-identified electronic patient care records (ePCRs), including paramedic clinical assessment, patient self-report, information from third parties and other evidence at the scene, such as written statements of intent (including social media, text messages and written notes), as recorded by paramedics. Intent of self-harm behaviours derived from the ePCR may be from either stated or physical evidence, or where there is evidence but the patient may have denied the behavioural intent (Lubman et al. 2020).
Self-harm related ambulance attendances are included if self-harm occurred in the preceding (past 24 hours) or during the ambulance attendance, with 4 categories of self-harm related ambulance attendances defined and coded as:
- self-injury (non-fatal intentional injury without suicidal intent)
- suicidal ideation (thinking about killing oneself without acting on the thoughts)
- suicide attempt (non-fatal intentional injury with suicidal intent, regardless of likelihood of lethality)
- suicide (fatal intentional injury with suicidal intent).
Suicide, suicide attempt and suicidal ideation are considered mutually exclusive; however, self-injury could be simultaneously coded with any other self-harm case category.
The number of attendances related to suicide is under-represented as ambulances do not attend all deaths. Furthermore, when they do attend there may be insufficient information to determine suicidal intent at the scene.
A modified ICD-10 coding framework is used to code the methods of suicide, suicide attempt or suicidal ideation, methods of self-injury and categories of suicidal ideation preparation (planned, unplanned and unknown if planned).
For more information see Lubman et al.2020.
Data limitations
Data are collected for operational rather than monitoring or research purposes with paramedics only recording information that they either observe or is provided to them by the patient or bystanders, and which they deem clinically relevant to patient care. It is possible that relevant information with respect to self-harm or mental health variables is not recorded, or similar events may not be recorded consistently by different paramedics over time.
The Multi-Agency Data Integration Project (MADIP) is a partnership among Australian Government agencies to develop a secure and enduring approach for combining information on healthcare, education, government payments, personal income tax, and demographics (including the Census) to create a comprehensive picture of Australian populations over time (ABS 2018). The key MADIP datasets used in analysis published on the Suicide and Self-Harm Monitoring site were:
- Person Linkage Spine (Australian Bureau of Statistics)
- 2011 Census of Housing and Population (Australian Bureau of Statistics)
- Causes of Death (Australian Bureau of Statistics)
- Personal Income Tax (Australian Taxation Office)
- Social Security and Related Information (Department of Social Services)
- Synthetic income data developed by the Australian National University using personal income tax data, social security payment information and Census (for more information see Biddle & Marasinghe 2021).
Linkage approach
In order to identify socioeconomic factors associated with deaths by suicide in Australia, 2011 Census and 2011 to 2017 Causes of Death data were linked to the ABS Person Linkage Spine (Spine). The Spine is comprised of all persons in the Medicare Enrolments Database, Personal Income Tax or Social Security and Related Information data sets at any point between 2006 and 2016 (ABS 2019). As the baseline population, 2011 Census was considered a closed population and several assumptions were made about this population. These include:
- everyone in the 2011 Census who did not die over the period were still in the population up to the end of 2017, that is, no migration occurred
- person information in the 2011 Census were held constant over the analysis period. However, in the modelling analysis conducted, time varying age and income of the year before suicide were calculated and applied.
Table 1 shows the linkage coverage of Census 2011 and deaths by suicide from the ABS Causes of Death. The Estimated Residential Population of Australia at 30 September 2011 was 22.43 million people (ABS 2021). Of these, 20,739,159 were accounted for in the Census 2011, noting that the Census 2011 started in August 2011. In total, the linked Census 2011 population was 16,700,062 (74.4% of the total Australian population of September 2011). According to the National Deaths Index, there are 17,306 deaths by suicide from September 2011 to December 2017, of which 11,580 (67%) deaths by suicide were linked to the linkable Census 2011 data. Suicide was defined by ICD-10 external cause codes X60–X84 and Y87.0
Total (n) | Linked (n) | Linked (%) | |
|---|---|---|---|
ERP(a) at Sept 2011 | 22,432,771 | 16,700,062 | 74 |
Deaths by suicide(b) | 17,306 | 11,580 | 67 |
- Estimated resident population. Linked records are from 2011 Census population.
- Linked deaths by suicide weighted to all deaths by suicide from September 2011 to December 2017.
Estimated suicide risk by educational attainment and employment method
Imputing weights for unlinked suicide deaths and 2011 Census
To address the issue of unlinked deaths by suicide and 2011 Census records, an imputation weighting technique was used. This section describes the method used to develop these weights, which involved a three-staged approach.
First stage: imputing weights to scale up the Census population. The ABS historical ERP for 31 December 2011 by states, sex and 5-year age groups were used to derive weights by these demographic characteristics, based on the assumption that there were no significant differences in the age distribution of the population. The derived weight was applied at the person level for each record of Census that has ABS Person Linkage Spine (Spine) information to enable analysts to weight the analyses to the 31 December 2011 total ERP.
Unlike the original ABS research paper (ABS 2016) describing the creation of a linked data set between 2011 Census and deaths registered in the following 13 months, the imputation method did not calculate weights by Indigenous and non-Indigenous populations. Also, note that Diplomatic personnel resident in Australia have not been excluded from total ERP.
Second stage: suicide weights were calculated by using all deaths by suicide from 2011 to 2017 by states and territories, sex and 5-year age groups. Suicide weights were then applied at person level to only those linked Census records with suicide information. This made it possible to weight the analyses to all deaths by suicide (18,848) from 2011–2017.
An issue with applying suicide weights is that suicide weights are slightly higher when compared with population weights applied in the first stage. As such, the combined weights of the linked records with both 2011 Census and suicide information when aggregated, the weighted ERP will be slightly higher than that of 31 December 2011. Hence the need for a scale down adjustment factor.
Third stage: Finally, a scale down adjustment factor, derived based on total ERP, linked deaths by suicide and all deaths by suicide, was applied at the person level to only Census records without linked death by suicide information. Hence the weights of the Census population with or without linked death by suicide information, aggregated to the 31 December 2011 ERP (22,340,025).
Cumulative suicide incidence
Australian residents in the 2011 Census, weighted to 31 December 2011 estimated resident population (ERP) and linked to ABS Causes of Death data from 2011 to 2017 created a binary outcome of either died by suicide (ICD 10 external cause codes X60–X84, Y87.0) or not. Note that deaths by suicide used in this analysis are based on year of occurrence. These may differ from deaths by suicide data used in other AIHW publications which are based on year of registration. In addition to the closed population assumptions noted above, due to data quality issues the age in this analysis is at the time of the 2011 Census except for those who have died by suicide.
Over the period 2011 to 2017, Australia recorded more than 18,800 deaths by suicide of people who were in the 2011 Census. This resulted in a cumulative incidence of about 84 per 100,000 people during the 7-year period. The cumulative number and incidence of deaths by suicide that occurred over the 7 years varies considerably by sex, educational attainment and labour force status.
Uncertainty in the estimates
All data are subject to some level of uncertainty. For the data presented in this analysis the sources of uncertainty include:
Linkage error: Uncertainty is introduced when there is error in linking data sets. The data used in this report carries some risk of linkage error. An attempt has been made to reduce this error through imputation weighting process but some uncertainty remains.
Timeliness of data: Some of the data used in this analysis is Census data collected in August 2011. A person’s education status and employment status can change over time, particularly for certain population groups. The use of out-of-date information introduces a source of error to the analysis.
Randomness in the number of deaths by suicide that occur in a given time period, 2011–2017: The number of deaths by suicide that occur in a given time period fluctuate, even if the underlying population risk remains the same. The exact distribution of the counts is unknown. With deaths by suicide being a rare event it is often assumed that the counts follow a Poisson distribution. If this is the case then the relative level of uncertainty due to randomness decreases as the number of deaths by suicide increase.
Regression risk models for selected census variables
The MADIP datasets used in this modelling are outlined in the Data section of these Technical notes. In this analysis, only people aged 25 to 64 years in the linked 2011 Census have been included, representing, over 9 million people in the 2011 Census and 7,000 deaths by suicide from 2011 to 2017. This age group was chosen because most deaths by suicide occur between these ages and because of the relative stability of socioeconomic factors over time (such as level of education) among this age group. While suicide is the leading cause of death among people aged 15 to 24 years, people in this age group were excluded from the modelling because of their lack of socioeconomic stability.
Missing values have been excluded from this analysis. Educational attainment has the highest proportion of missing values (5.5%). Unlike with the cumulative suicide risk estimations, the data used in the regression modelling has not been weighted.
To identify modelling predictors and explore their association with suicide deaths, an extensive literature review of social factors was carried out. This included earlier analyses published by AIHW, which showed deaths by suicide varied by factors such as employment and educational attainment.
Socioeconomic factors identified from the 2011 Census were used as predictors and deaths by suicide as the outcome variable. A total of 10 factors were included:
- Age (10-year age groups)
- Sex
- Indigenous status
- Registered marital status
- Family household composition
- Highest level of educational attainment
- Labour force participation
- Occupation
- Synthetic total income (quartiles, see Biddle & Marasinghe 2021)
- Need for assistance with core activities of daily living.
Method
Two modelling approaches were tested: Poisson regression and competing-risks regression (as described by Fine & Gray 1999). For Poisson regression, counts of the outcome variable with the value 1 for deaths by suicide and 0 for those who did not die by suicide were created and data aggregated by socioeconomic factor.
For the competing-risks regression, the influence of other causes of death is considered. This is because people who died from any other causes (such as cancer and coronary heart disease) are no longer at risk of dying by suicide.
Sex-stratified and Indigenous-stratified multivariate models were also fitted to investigate the associations within males and females, and within Indigenous and non-Indigenous people. Due to data quality issues including small sample sizes, Indigenous-stratified models have not been published. Univariate and multivariate models (including quasi-Poisson to deal with slight overdispersion) were also refitted. The coefficients obtained were back transformed so they could be interpreted as rate ratios (for Poisson models) and subhazard ratios (for competing-risks models). Analysis was conducted using R (glm package) and Stata (version 16) software.
Of the models tested, competing-risks regression, a method that accounts for people being censored from the risk set because of a competing cause, was used to estimate the risk of death by suicide and the selected socioeconomic factors. Univariate, multivariate and sex-stratified competing-risks models were developed. Generally, competing-risks regression models can be regarded as an extension of the Cox proportional hazards model, where subjects who experience competing events (deaths from other causes) are adequately counted as not having any chance of dying by suicide.
Estimated coefficients of competing-risks models can be interpreted in a similar way as coefficients estimated from a Cox model, except that they estimate the effect of certain covariates in the presence of competing events. Note that the transformed coefficients are known as subhazard ratios, similar to hazard ratios estimated in Cox regression. The subhazard ratio can be interpreted as a rate ratio (Henan 2010), but here we are considering the relative change in rates of the event in those subjects who are either currently event-free or who have previously experienced a competing event (Austin & Fine 2017). For simplicity and ease of understanding, coefficients in this report are referred to as hazard ratios.
Social and economic factors associated with suicide in Australia: a focus on individual income
Researchers from the Australian National University’s Centre for Social Research and Methods (CSRM), in close collaboration with the AIHW, have extended the analysis Regression risk models for selected census variables. An extract from the Multiagency Data Integration Project (MADIP) was used. For this analysis, the following MADIP datasets were utilized. 2011 Census information, 2011-2016 Personal income tax (PIT) records, 2011-2016 Social security and related information (SSRI) and 2011-2016 cause of death data. The data linkage process was identical to the linkage process described in the Data section of these Technical notes.
The following set of explanatory variables were used to capture the social and economic factors. More specifically, the CSRM used the time-invariant 2011 Census data to capture social factors and time-variant PIT and SSRI to capture economic factors of suicide.
Variable | Source | Type |
|---|---|---|
1. Highest level of education | 2011 Census | Social |
2. Age | 2011 Census | Social |
3. Sex | 2011 Census | Social |
4. Indigenous status | 2011 Census | Social |
5. Need for assistance with core activities | 2011 Census | Social |
6. Household composition | 2011 Census | Social |
7. Total income | 2011 – 2016 PIT | Economic |
8. SSRI | 2011 – 2016 SSRI | Economic |
In addition to the variables presented in Table 1, the following variables were derived using Census, PIT and SSRI data.
- A synthetic measure of income – A measure of income that was derived using a machine learning algorithm. This income variable provides a representative measure of income of the entire Australian population (Biddle and Marasinghe 2021). This measure was then divided into quintiles to obtain a relative measure of income.
- Coefficient variation of income (relative standard deviation) – Coefficient of variation of income was used to capture the income uncertainty of each individual. The measure was defined such that it captured income uncertainty between the current year and the previous year (i.e. variation between t and t-1). This measure was then divided into quintiles. An income uncertainty of quintile 1 implied an individual had low-income variation relative those in higher income uncertainty quintiles. Furthermore, since this measure uses data from t-1, the scope of the study was limited to 2012 January to 2016 December.
- Proxy for unemployment – Unemployment status of an individual was captured using SSRI information. More specifically, if an individual received Newstart allowance and Youth allowance, the individual was then classified as being unemployed that period.
Methods
Longitudinal (panel) regression
The MADIP dataset is a longitudinal dataset therefore, utilizing longitudinal regression methods allows us to control for unobserved individual heterogeneity across the time period. For example, longitudinal regression methods would allow us to control for unobserved measures such as behavioural differences and cultural differences across individuals. Given that suicide is a complex individual decision and may not be entirely explained by observed variables, controlling for these unobserved heterogeneity would allow us to obtain unbiased estimates.
In this analysis, two competing longitudinal regression methods were tested – a random effects logistic model and a population-averaged logistic model. Both models were estimated with robust standard errors to account for heteroskedasticity.
Given that the random effects logistic model is dependent on the strong assumption that the underlaying variation have no serial correlation, the population-averaged logistic model was selected as the primary regression method due to its robustness to serial correlation (Hill et al., 2010). Furthermore, a likelihood-ratio test was also undertaken to decide between the two models. The result suggested that the population-averaged model was more appropriate than the Random effects model. Equation (1) and (2) outline the population-averaged model.
Setting up the dataset as a panel allowed us to account for individual heterogeneity. However, given that suicide is a rare event, explanatory variables with large number of categories (for example – occupation) were excluded from the longitudinal analysis. This was primarily due the low number of suicides each year, which in turn made the models more sensitive to variables with a large number of categories. Given this drawback of panel data, a cross-sectional analysis was also conducted as a part of the sensitivity analysis.
Figure 1 - Annual suicide counts1
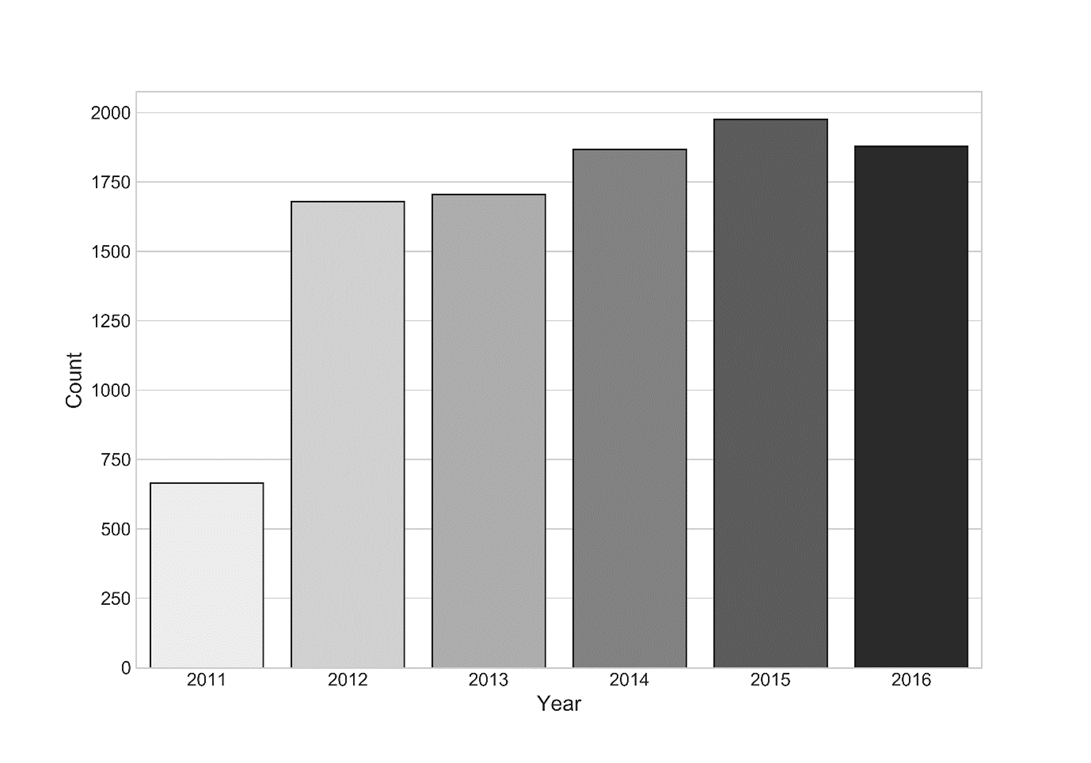
1 Year 2011 was not included in the analysis.
Reference
Hill, R.C., Griffiths, W.E. and Lim, G.C., 2010. Principles of econometrics. pp 537-560. John Wiley & Sons.
In addition to the NMD, the Australian Defence Force (ADF) suicide monitoring analysis used the following data sources:
National Death Index (NDI)
The NDI is managed by the AIHW and contains person-level records of all deaths in Australia since 1980 obtained from the Registrars of Births, Deaths and Marriage in each state and territory. Its use is confined to data linkage studies approved by the AIHW Ethics Committee for health and medical research. NDI records are supplemented with cause of death information from the NMD. In this study, the NDI is linked with Defence payroll data to create the linked Defence payroll–NDI data set used in analysis of suicide in the ADF population.
Department of Defence personnel system data
The Department of Defence compiled a file of current and historical Defence personnel systems covering ADF members who have served since 1 January 1985. This combines PMKeyS, Core HR system, D1, CENRESPAY (for reservists), ADFPAY (for permanent members) and other historical payment systems. The Department of Defence and AIHW assessed the resulting file for completeness and duplicates. Comparisons were made with records from Department of Defence annual reports and other sources to validate the list. Data from the National Archives was also investigated for its suitability in validation, however as the majority of records are electronic files based on photos of paper records, this was not usable.
For further information see Technical notes of Serving and ex-serving Australian Defence Force members who have served since 1985: suicide monitoring 1997 to 2021.
Estimates of fatal (years of life lost, YLL) and non-fatal burden (years lived with disability, YLD) were sourced from the Australian Burden of Disease Study (ABDS) 2015. The ABDS 2015 used burden of disease analysis to measure the impact of 216 diseases and injuries on the health of the Australian population. The study provides a detailed picture of the burden of disease and injury in the Australian population in 2003, 2011 and 2015. It also includes estimates of the contribution made by selected risk factors on the disease and injury burden in Australia, and by socioeconomic areas for some risk factors.
The ABDS 2015 uses and adapts the methods of global studies to produce estimates that are more relevant to the Australian health policy context. The chosen reference period (2015) reflects the data availability from key data sources (such as the National Health Survey, deaths data, hospital admissions data and various disease registers) at the time of analysis.
Results from the study provide an important resource for health policy formulation, health service planning and population health monitoring. The results provide a foundation for further assessments.
Full details on the various methods, data sources and standard inputs used in the ABDS 2015 are available in Australian Burden of Disease Study 2015: methods and supplementary material.
New South Wales Suicide Monitoring System
The New South Wales (NSW) Suicide Monitoring System contains data on all suspected and confirmed suicide deaths from 2019 to present. Established in October 2020, the system is a collaboration between the NSW Ministry of Health, Department of Communities and Justice, the State Coroner and NSW Police.
The NSW Suicide Monitoring System contains initial police information of suspected suicide deaths from the JusticeLink information system, which is managed by NSW Department of Communities and Justice. The information is manually checked against other data sources, including coronial determination.
NSW Health publishes monthly reports on suspected deaths by suicide in NSW on their website NSW Suicide Monitoring System.
Victorian Suicide Register
The Victorian Suicide Register (VSR) contains data on all suicide deaths reported to the Coroners Court of Victoria (CCOV) from 2000 to present. The Coroners Prevention Unit, a specialist investigative service for Victorian Coroners, has managed the VSR since its implementation in 2012. The VSR operates with funding from the Victorian Department of Health.
VSR data are used to inform investigations into suspected suicides and support coronial recommendations to prevent similar deaths. VSR data are regularly shared with the Victorian Department of Health, AIHW, Victoria Police and other organisations involved in suicide prevention.
Data on the VSR are obtained and coded from materials gathered throughout the course of coronial investigation, including police notification of death, forensic reports (autopsy and toxicology), witness statements and medical records.
CCOV releases a range of suicide data reports from the VSR on their website, including information on suspected deaths by suicide on a monthly basis, and overviews of First Nations suicides in Victoria. CCOV has also published a report on suicide among LGBTIQ+ people in Victoria.
Queensland Suicide Register and interim Queensland Suicide Register
In Queensland, there are two systems that are used to monitor suicide deaths: the Queensland Suicide Register (QSR), which includes suicide data since 1990 and is used to monitor longer-term trends, and the interim Queensland Suicide Register (iQSR). The iQSR was established in 2011 to provide real-time information on suicide deaths.
Data on this website are from the iQSR. The iQSR contains interim data on suspected suicides in Queensland, recorded shortly after the death occurs. The data are based on initial police reports and other information that is available to police at the time when they refer the death to the coroner.
The QSR contains information on suicide deaths for which coronial investigations have been finalised. The QSR is based on more information than the iQSR, including toxicology reports, post-mortem examination and the finding from the coroner, including details on the context and circumstances of the death.
The QSR and iQSR are currently managed by the Queensland Mental Health Commission (QMHC) on behalf of the Queensland Government, with support from the Coroners Court of Queensland (CCQ) and Queensland Police Service (QPS). Prior to September 2023, the iQSR was managed by the Australian Institute for Suicide Research and Prevention (AISRAP) at Griffith University. The QMHC publishes monthly reports based on data from the iQSR, around eight weeks from the last day of the reporting month.
End of life service use for those who died from suicide in Australia
Data sources
Data are from the National Integrated Health Services Information Analysis Asset (NIHSI AA) version 0.5. This data asset includes mortality data together with information from hospital admissions, Medicare Benefits Schedule (MBS), Pharmaceutical Benefits Scheme (PBS) and residential aged care data.
The analysis population was those who had died between 1 July 2010 and 31 December 2017 in the linked National Deaths Index (NDI). Suicide was defined as the principal external cause of death in X60–X84 and Y87.0 based on the International Classification of Diseases, Tenth Revision (ICD-10) codes. Patient demographic information was taken from the NDI and is therefore accurate at the time of death not time of service. Only people whose age at death was between 15 to 64 years were included in the analysis. This was due to people in this age range making up the majority of those who die from suicide and to allow for better comparisons with deaths from other causes, which mostly occur in people older than 65 (AIHW 2022a). People without a primary cause of death and with sex not stated were also removed from the analysis due to small cell sizes.
Method
The analysis included MBS, PBS emergency department presentation and outpatient services in addition to hospital admissions datasets. For more information on MBS item classification and PBS item classification, drawn from the Anatomical Therapeutic Chemical (ATC) codes (AIHW 2022b), visit Mental health services in Australia – Data source and key concepts.
Hospitalisation data was taken from two sources: admitted patients and emergency department (ED) presentations. The method for counting hospital admissions in this analysis based on the method in a similar study by Clapperton et al. (2021).
Within the NIHSI AA v0.5, hospital data pertains to only New South Wales (NSW), Victoria (Vic) (excluding Albury-Wodonga), South Australia (SA) and Tasmania (Tas) public hospitals. Admitted patient information also contains information from private hospitals in Victoria. To ensure accurate comparisons with hospitals data, only deaths registered in NSW, Vic, SA and Tas are included in the analysis.
Admitted patient data refers to only acute admitted and mental health separations (Admitted Patient Care National Minimum Data Set care types of 1, 7.1, 7.2, and 11). In scope separations where the patient was transferred from another hospital or had a change of care type in the same hospital are not counted in the total to avoid duplication.
Any hospital episode (ED presentation, hospital admission) that ended in “death” was excluded as it was considered to be a result of the fatal (suicide) incident. The only exception to this were episodes where the intentional self-harm was coded as occurring in a health service area–these episodes were retained as they were most likely inpatient suicides (Clapperton et al. 2021).
For admitted patient data, the definitions for mental health and self-harm behaviours include:
- ‘Any mental health’ hospitalisations are defined as any diagnosis (principal, secondary, etc.) of a mental disorder (ICD-10-AM codes F00–F99).
- Intentional self-harm hospitalisations are defined based on the ICD-10-AM principal diagnosis in the range S00–T75 or T79 and has a principal external cause code in the range X60–X84 or Y87.0.
- Suicidal ideation hospitalisations (ICD-10-AM code R45.81) are grouped with ‘any mental health’ and intentional self-harm hospitalisations, as this code is usually coded in the absence of a mental health condition.
For ED presentation data, the definitions ‘mental health-related ED presentations’ refers to presentations that have a principal diagnosis that falls within the Mental and behavioural disorders chapter (Chapter 5) of ICD‑10‑AM (codes F00–F99). It should be noted that this definition does not encompass all mental health‑related presentations to ED. See Mental health services in Australia for further information.
Presentations to hospital emergency departments relating to suicide attempts or intentional self-harm cannot be easily identified in the current national emergency department data collection. Furthermore, ICD‑10‑AM diagnosis codes for intentional self-harm do not specify if there was suicidal intent or not— and therefore includes both suicide attempts and non-suicidal self-harming behaviours (AIHW 2022b). See Suicide & self-harm monitoring: Intentional self-harm hospitalisations for further information.
‘Any hospitalisation’ refers to any acute admitted/mental health care separation or ED presentation.
Limitations of this analysis includes:
- Mental health items could be miscoded or reported, for example, GP mental health services are typically billed under general GP consultations.
- Service use captured in the NIHSI is influenced by severity of condition, a person’s ability and desire to access a service, and the availability of alternative services not captured in the data (e.g. private community mental health services).
References
Australian Institute of Health and Welfare (AIHW) (2022a) Deaths in Australia, AIHW, Australian Government, accessed 11 October 2022.
Australian Institute of Health andAIHW Welfare (2022b) Mental health services in Australia, AIHW, Australian Government, accessed 09 September 2022
AIHW (2022c) Suicide and self-harm monitoring: Intentional self-harm hospitalisations, AIHW, Australian Government, accessed 14 October 2022.
Clapperton A, Dwyer J, Millar C, Tolhurst P and Berecki-Gisolf J (2021) ‘Sociodemographic characteristics associated with hospital contact in the year prior to suicide: A data linkage cohort study in Victoria, Australia’, PLoS ONE, 16(6): e0252682, doi:10.1371/journal.pone.0252682.



