Clients with a current mental health issue
On this page
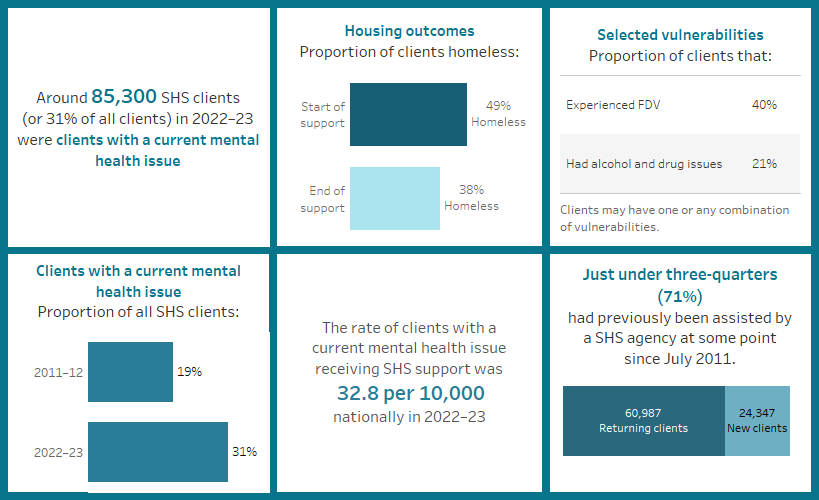
Key findings: Clients with a current mental health issue, 2022–23
Mental health is ‘a state of well-being in which an individual realises his or her own abilities, can cope with normal stresses of life, can work productively and is able to make a contribution to his or her community’ (WHO 2022). The term ‘mental health issues’ captures the entire range of mental health problems, from psychological distress to clinically diagnosed conditions. Mental health issues can both contribute to the risk of experiencing homelessness and develop in response to experiencing homelessness (Flatau et al. 2022).
The risk of or experience of homelessness can be devastating to mental health (Ong Viforj et al. 2022). The stress, trauma, isolation, instability, and stigmatisation that often comes with experiencing homelessness can trigger, maintain and exacerbate mental health issues, and the likelihood of experiencing homelessness can depend on the type of mental health condition (Moschion and Ours 2021, Batterham 2020, Johnson and Chamberlain 2016). In 2020–2022, around 2 in every 5 (39%) people aged 16–85 with a history of homelessness experienced a mental health condition within the past year, almost twice as high as the general Australian population (21%) (ABS 2023). While the environmental stressors of homelessness can contribute to mental health issues, mental health issues can also contribute to the risk of experiencing homelessness (Moschion and Ours 2021, Brackertz et al. 2020).
People with mental health issues are especially vulnerable to experiencing homelessness (Nilsson et al 2019). Mental health issues that increase psychological distress and impair decision-making in everyday life can contribute to employment issues, social support breakdown, and financial hardship (Johnstone et al. 2016, Kaleveld et al. 2018, Walter et al. 2016). These issues can lead to challenges with securing or maintaining housing (Brackertz et al. 2018).
Defining clients with a mental health issue in the Specialist Homelessness Services Collection (SHSC)
Specialist Homelessness Services (SHS) clients are identified as having a current mental health issue if they are aged 10 years or older and have provided any of the following information:
- They indicated that at the beginning of support they were receiving services or assistance for their mental health issues or had in the last 12 months.
- Their formal referral source to the SHS was a mental health service.
- They reported ‘mental health issues’ as a reason for seeking assistance.
- Their dwelling type either a week before presenting to an agency, or when presenting to an agency, was a psychiatric hospital or unit.
- They had been in a psychiatric hospital or unit in the last 12 months.
At some stage during their support period, a need was identified for psychological services, psychiatric services or mental health services.
Client characteristics
Clients with a current mental health issue (85,300 clients) were the second largest SHS client group in 2022–23, making up around a third (31%) of all SHS clients (Supplementary table CLIENTS.41).
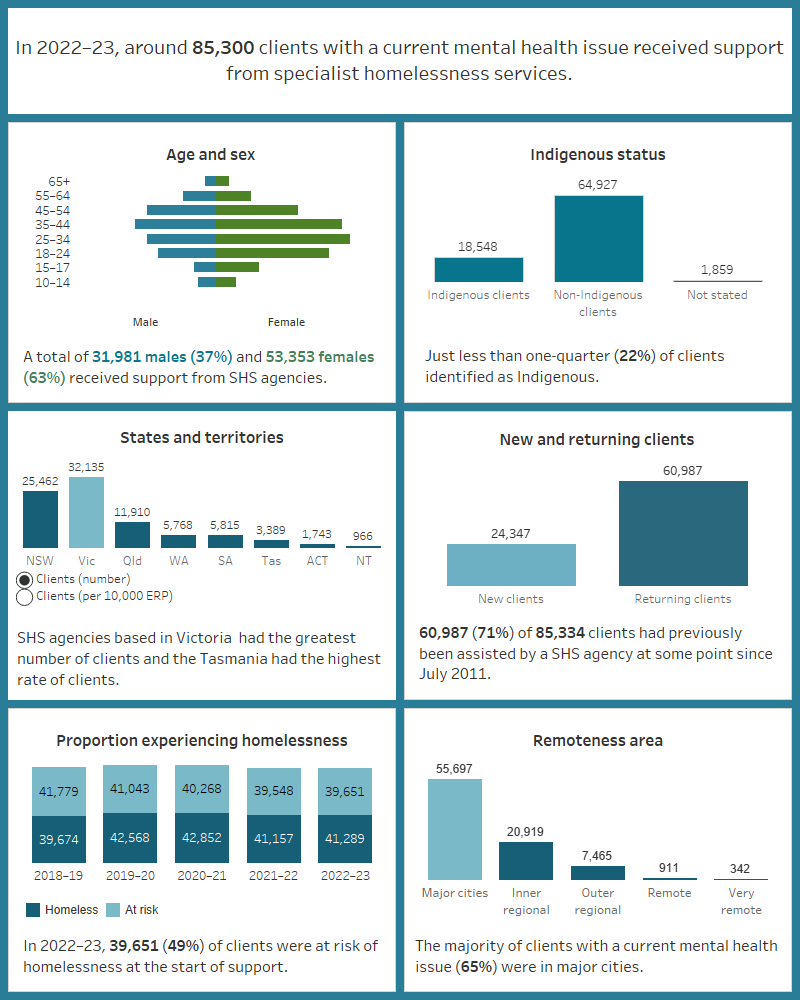
Figure MH.1: Key demographics, SHS clients with a current mental health issue, 2022–23
This image describes the characteristics of around 85,300 clients with a current mental health issue and received SHS support in 2022–23. Most clients were female, aged 18–44. Less than a quarter were Indigenous. Victoria had the greatest number of clients and Tasmania had the highest rate of clients per 10,000 population. The majority of clients had previously been assisted by a SHS agency since July 2011. Half were at risk of homelessness at the start of support. Most were in major cities.
Living arrangements and presenting unit type
Of the 85,300 clients with a current mental health issue in 2022–23, most clients presented to a SHS agency alone (82% or 69,700 clients) and lived alone at the beginning of support (48% or 40,300 clients). Around one-quarter of clients were living as a single parent with child/ren (24%) (Supplementary tables CLIENTS.44 and CLIENTS.45).
Labour force status
Around 9 in 10 clients with a current mental health issue (aged 15 and older) were not working in a paid job (85% or 64,800 clients) in 2022–23. More than half (53%) of clients were looking for work (that is, unemployed) and one-third (32%) were not in the labour force. Around 3 in 20 clients (15%) with a current mental health issue were employed (Supplementary table MH.7).
Selected vulnerabilities
More than half of clients with a current mental health issue (52% or 44,300 clients) experienced another type of vulnerability in 2022–23 (Supplementary table CLIENTS.47). Given clients with a current mental health issue often experience multiple different types of vulnerabilities, this highlights the value of an integrated service response to homelessness for these clients (Flatau et al. 2022).
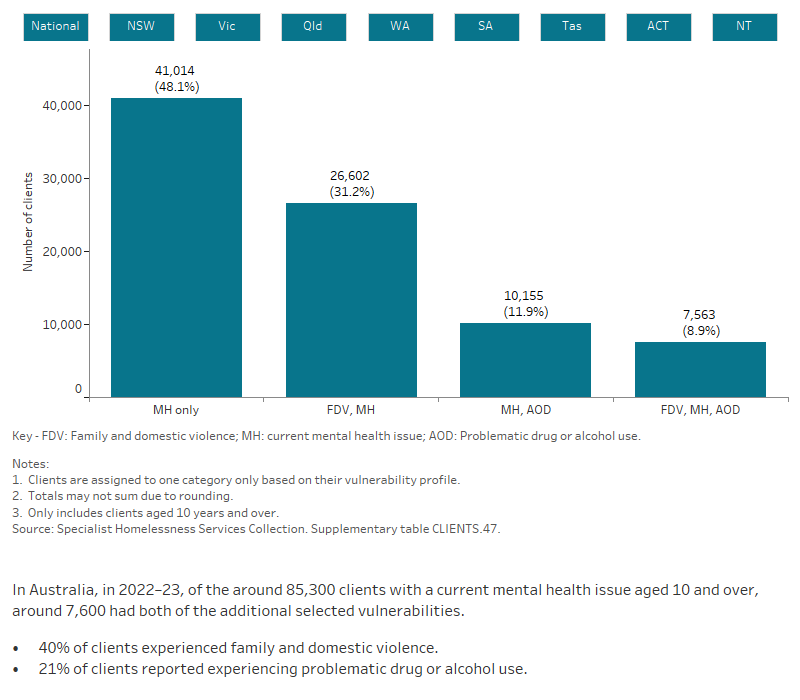
Figure MH.2: Clients with a current mental health issue, by selected vulnerability characteristics, 2022–23
The interactive bar graph shows proportions of clients with a current mental health issue also experiencing additional vulnerabilities, including experiencing family and domestic violence and problematic drug and/or alcohol use. The graph shows both the number of clients experiencing a single vulnerability only, as well as combinations of vulnerabilities, and presents data for each state and territory.
Service use patterns
The length of support that clients with a current mental health issue received in 2022–23 increased to a median of 88 days from 85 days in 2020–21. Similarly, the median number of nights accommodated increased to 49 nights in 2022–23 from 48 nights in 2020–21 (Supplementary tables MH.2 and CLIENTS.48).
Changes over time since 2011–12
The number and rate of SHS clients with a current mental health issue has increased at a rate faster than most other client groups, since the collection began in July 2011. As a proportion of all clients, those with a current mental health issue has increased with each successive year (Historical data table HIST.MH).
Between 2011–12 and 2022–23 (Supplementary table HIST.MH):
- The proportion of clients with a current mental health issue increased from around one-fifth (19%) to almost one-third (31%) of all SHS clients.
- The number of clients with a current mental health issue increased by an average of 6.0% with each year; an annual change more than 4.5 times higher than that for all SHS clients (1.3%) over the same period.
- The rate of SHS clients with a current mental health issue increased from 20.0 clients per 10,000 population to 32.8.
New or returning clients
In 2022–23, among SHS clients with a current mental health issue (Supplementary table CLIENTS.42):
- 7 in 10 (71% or 61,000 clients) were returning clients, that is, clients had received assistance from a SHS agency some time since July 2011 onwards.
- 3 in 10 (29% or 24,300 clients) were new to SHS agencies.
Main reasons for seeking assistance
In 2022–23, the main reason that clients with a current mental health issue sought assistance from a SHS agency was not commonly related to mental health issues (4.2% or 3,600 clients). Instead, the main reasons for seeking assistance were for (Supplementary table MH.5):
- housing crisis (21% or 18,000 clients)
- family and domestic violence (19% or 16,200 clients)
- inadequate or inappropriate dwelling conditions (13% or almost 11,100 clients).
The most common main reason(s) clients with a current mental health issue sought assistance differed slightly depending on whether the clients were at risk of homelessness or were experiencing homelessness when they first presented to a SHS agency. Among those experiencing homelessness, the main reason was housing crisis (24% or 9,800 clients), while for those at risk of homelessness it was family and domestic violence (23% or 9,000) (Supplementary table MH.6).
Services needed and provided
In 2022–23, most clients with a current mental health issue needed assistance with accommodation provision (70%), though other common assistance sought included general advice and advocacy. Assistance with accessing mental health services was also relatively common, with more than one-quarter (27% or 22,700) of clients with a current mental health issue needing assistance with mental health-based services (Supplementary table MH.2). Specifically:
- 24% (20,800 clients) needed mental health services; 47% (9,800 clients) of these clients were provided with this type of service.
- 8.5% (almost 7,200 clients) identified a need for psychological services; 34% (2,400 clients) of these clients had this need met.
- 5.6% (4,800 clients) identified a need for psychiatric services; 34% (1,600 clients) of these clients had this need met.
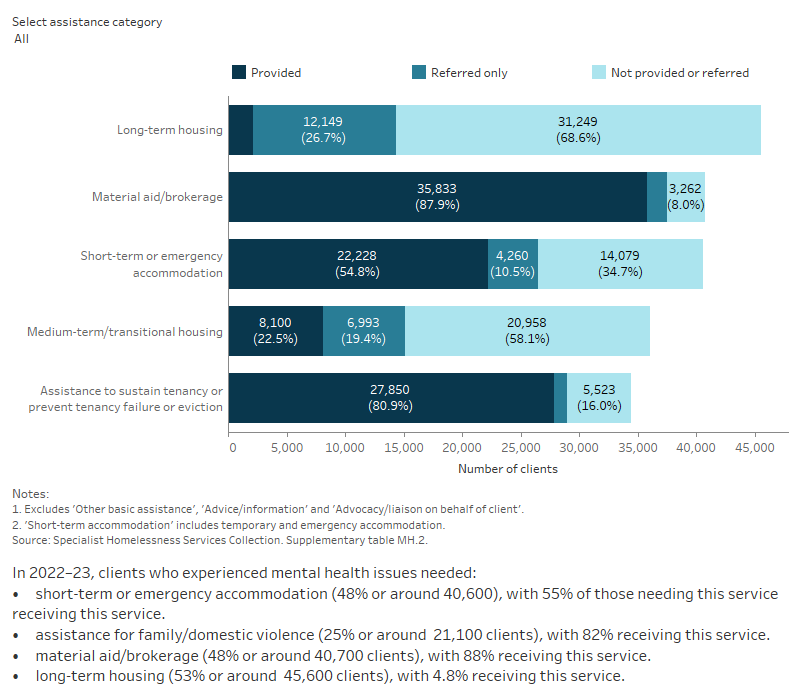
Figure MH.3: Clients with a current mental health issue, by services needed and provided, 2022–23
This interactive stacked horizontal bar graph shows the services needed by clients with a current mental health issue and their provision status. Material aid/brokerage and assistance to sustain tenancy or prevent tenancy failure or eviction were the most provided services. Long-term housing was the least provided service.
Housing situation and outcomes
Outcomes presented here highlight the changes in clients’ housing situation at the start and end of support. That is, the place they were residing before and after they were supported by a SHS agency. The information presented is limited only to clients who have stopped receiving support during the financial year, and who were no longer receiving ongoing support from a SHS agency. In particular, information on client housing situations at the start of their first period of support during 2022–23 is compared with the end of their last period of support in 2022–23. As such, this information does not cover any changes to their housing situation during their support period.
In 2022–23, half (49% or 25,800 clients) of clients with a current mental health issue were experiencing homelessness at the start of support; around 7,000 (13%) were rough sleeping – one of the highest proportions of this housing type among the SHS client groups (Supplementary table MH.3).
By the end of support, fewer clients with a current mental health issue were known to be experiencing homelessness (38%) (Supplementary table MH.4):
- Around 3 in 5 clients (58% or 28,300 clients) were living in stable accommodation, such as public or community housing or private housing.
- More than one-third (37% or 8,800 clients) of clients experiencing homelessness at the start of support were housed.
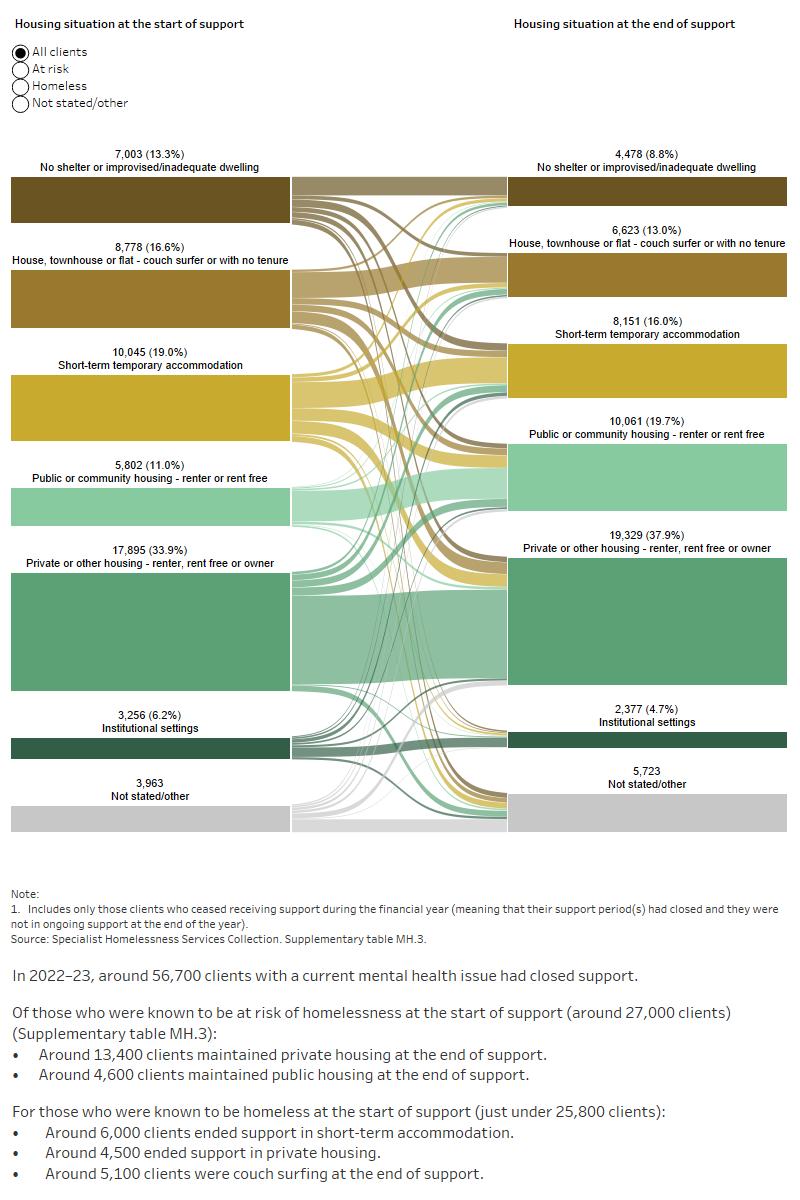
Figure MH.4: Housing situation for clients with a current mental health issue with closed support, 2022–23
This interactive Sankey diagram shows the housing situation (including rough sleeping, couch surfing, short-term accommodation, public/community housing, private housing and institutional settings) of clients with a current mental health issue with closed support periods at first presentation and at the end of support. The diagram shows clients’ housing situation journey from start to end of support. Most started and ended support in private housing.
Australian Bureau of Statistics (ABS) (2023) National Study of Mental Health and Wellbeing, ABS website, accessed 23 October 2023.
Batterham D (2020) Public Perceptions of Homelessness – a literature review, Launch Housing website, accessed 29 August 2023.
Brackertz N, Borrowman L, Roggenbuck C, Pollock S and Davis E (2020) Trajectories: the interplay between mental health and housing pathways: Final research report, Australian Housing and Urban Research Institute Limited (AHURI) and Mind Australia.
Brackertz N, Wilkinson A and Davison J (2018) Housing, homelessness and mental health: towards systems change, report to the Australian Government National Mental Health Commission, Australian Housing and Urban Research Institute Limited.
Flatau P, Lester L, Seivwright A, Teal R, Dobrovic J, Vallesi S, Hartley C and Callis Z (2022) Ending Homelessness in Australia: an evidence and policy deep dive, Centre for Social Impact, doi:10.25916/ntba-f006.
Johnson G and Chamberlain C (2016) ‘Are the Homeless Mentally Ill?’, Australian Journal of Social Issues, 46(1):29-48.
Johnstone M, Parsell C, Jetten J, Dingle G and Walter Z (2016) ‘Breaking the cycle of homelessness: Housing stability and social support as predictors of long-term well-being’, Housing Studies, 31(4):410-426, doi: 10.1080/02673037.2015.1092504.
Kaleveld L, Seivwright A, Box E, Callis Z and Flatau P (2018) ‘Homelessness in Western Australia: A review of the research and statistical evidence’, Government of Western Australia, Department of Communities.
Moschion J and Ours JC (2021) ‘Do transitions in and out of homelessness relate to mental health episodes? A longitudinal analysis in an extremely disadvantaged population’, Social Science & Medicine, 279 (2021), doi.org/10.1016/j.socscimed.2020.113667.
Nilsson SF, Nordentoft M and Hjorthøj C (2019) ‘Individual-Level Predictors for Becoming Homeless and Exiting Homelessness: a Systematic Review and Meta-analysis’, Journal of Urban Health, 96(5):741-750, doi: 10.1007/s11524-019-00377-x.
Ong ViforJ R, Singh R, Baker E, Bentley R and Hewton J (2022) ‘Precarious housing and wellbeing: a multi-dimensional investigation’, AHURI Final Report No. 373, Australian Housing and Urban Research Institute Limited, doi: 10.18408/ahuri8123801.
World Health Organization (2022) Mental Health, WHO website, accessed 29 August 2023.


