Assault hospitalisations
Why are assault hospitalisation rates important?
Both fatal and non-fatal assaults involving young people contribute significantly to the burden of premature death, injury and disability. Violence among young people affects the victims and their families, friends and communities, contributing to increased health and welfare costs, reduced productivity, decreased value of property and disrupted essential services (Krug et al. 2002). Harmful and hazardous alcohol use are risk factors both for being victimised and perpetrating youth violence, and are therefore priority areas for intervention (WHO 2006; Pilgrim et al. 2014).
Do rates vary across population groups?
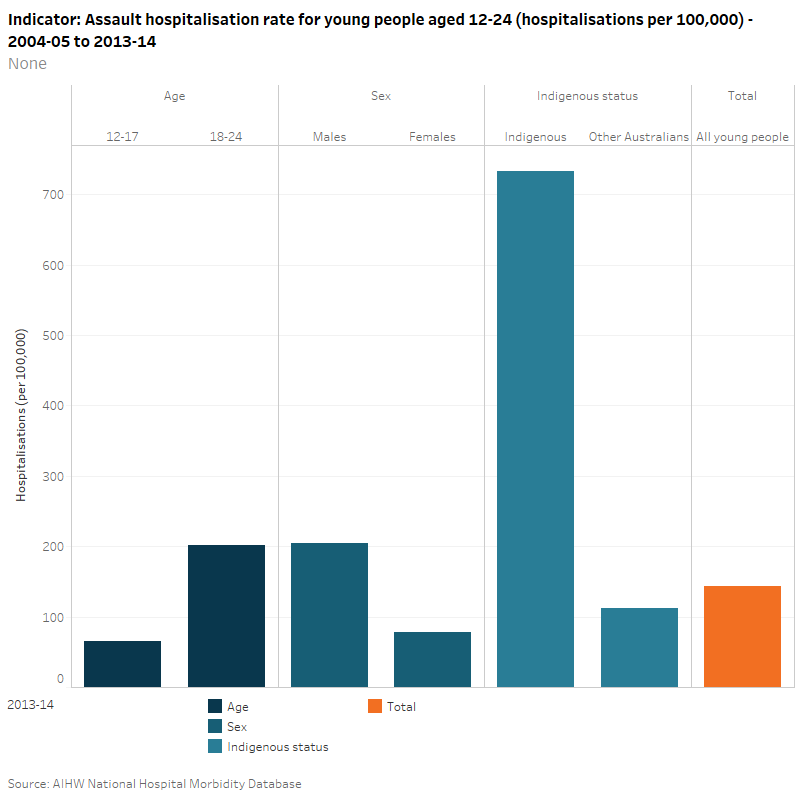
In 2013–14, the rate of hospitalisations due to assaults among all young people aged 12–24 in Australia was 143 per 100,000. Young people aged 18–24 had a rate of assault hospitalisation that was three times as high as the rate for 12–17 year olds (202 per 100,000 compared to 66 per 100,000). Males had a higher rate of hospitalisation than females, with 205 per 100,000 and 78 per 100,000, respectively. Indigenous young people were much more likely to be hospitalised due to assault with a rate 7 times as high as the rate for Other Australians (733 per 100,000 compared to 112 per 100,000).
Has there been a change over time?
Prior to 2007–08 there was a steady increase in the rate of assault hospitalisations for all young people aged 12–24, peaking at 223 per 100,000 in 2007–08. Since then there has been a decline in the rate of assault hospitalisations to 143 per 100,000 in 2013–14. Similar trends were evident for 12–17 year olds and 18–24 year olds.
Trends in assault hospitalisations among young males is similar to that of all young people, rising between 2004–05 to 2007–08, and declining from 358 per 100,000 in 2007–08 to 205 per 100,000 in 2013–14. There are no strong trends observed among young females with the rate of assault hospitalisations remaining steady at 80 per 100,000 from 2003 to 2013.
For young Indigenous Australians, the rate of assault hospitalisation has decreased in recent years, from 886 per 100,000 in 2009–10 to 733 per 100,000 in 2013–14. Over this period there has also been a decline in in the rate among Other Australians to 112.2 per 100,000 in 2013–14.
Injury hospitalisations are coded based on principal diagnosis, using the ICD-10-AM range S00-T75 or T79. Cases using this criterion are referred to as community injury. In 2013–14, diagnoses and external cause injury and poisoning were recorded using the 8th edition of the ICD-10-AM. Data from 2004–05 to 2012–13 were coded to earlier editions.
Assault hospitalisations includes injury cases in which the first reported external cause is Assault (ICD-10-AM X85-Y09) or Legal intervention and operations of war (Y35-Y36) as per AIHW: Pointer S 2013. Trends in hospitalised injury, Australia, 1999–00 to 2010–11. Injury research and statistics series no. 86. Cat. no. INJCAT 162. Canberra: AIHW.
Hospitalisations (referred to elsewhere as hospital separations) refer to episodes of admitted patient care which can be a total hospital stay or a portion of a hospital stay, beginning or ending in a change of type of care (for example, from acute care to rehabilitation). To reduce over-counting of injury cases, records have been omitted where the mode of admission is recorded as a transfer from another acute-care hospital.
Indigenous data is for 6 States (NSW, Vic, Qld, WA, SA and public hospitals in the NT) as these states are considered to have sufficient completeness of Indigenous identification for analysis from 2004–05 onwards. ACT and Tasmania are considered to have sufficient completeness of Indigenous identification from 2010–11 onwards; however, they are excluded for the purposes of time series analysis. Consequently, the Indigenous data may not necessarily be representative of the excluded jurisdictions.
Changes in the quality of the Indigenous identification over time may affect the time series for data presented for data by Indigenous status (i.e. categories ‘Indigenous’ and ‘Other Australians’).
‘Other Australians’ includes records for persons identified as not Indigenous as well as records where Indigenous status was not stated.
The hospitals admitted patient care data do not include non-admitted presentations to hospital (e.g. non-admitted patients in emergency departments).
AIHW National Hospital Morbidity Database
Data quality statement: AIHW METeOR
AIHW (Australian Institute of Health and Welfare): Pointer S 2014. Hospitalised injury in children and young people 2011–12. Injury research and statistics series no. 91. Cat. no. INJCAT 167. Canberra: AIHW.
Krug EG, Dahlberg LL & Mercy JA 2002. World Report on violence and health. Geneva: World Health Organization.
Pilgrim JL, Gerostamoulos D, Drummer OH 2014. “King hit” fatalities in Australia, 2000-2012: The role of alcohol and other drugs. Drug and Alcohol Dependence 135:119-132.
WHO 2006. Youth violence and alcohol. Geneva: World Health Organization.


