Hepatitis
Why are viral hepatitis infection notification rates important?
Hepatitis infections (inflammation of the liver) are a significant public health problem in Australia and can lead to a number of liver diseases including cirrhosis, cancer and liver failure. Hepatitis B and C are spread through exposure to infected body fluids or from parent to child. Hepatitis B and C disproportionately affects Indigenous people, those born overseas or those with a history of injecting drug use (The Kirby Institute, 2013).
In Australia, prevention of hepatitis B infection is primarily achieved through vaccination, which been routinely performed for infants since 2000 (DoH 2014a). Currently, there is no vaccine for hepatitis C and infection does not provide immunity to future infections. Preventative strategies are directed at minimising transmission of the virus through unsafe injecting practices (DoH 2014b).
In 2012 across all ages, of the newly-acquired hepatitis B cases that had at least one risk factor recorded, sexual exposure was the most frequently reported potential source of infection (around 41%), followed by injecting drug use (around 31%) (NNDSS 2012). For newly-acquired hepatitis C infection notifications, approximately 98% had a history of injecting drug use, of which almost 65% reported injecting drug use in the 24 months prior to diagnosis (NNDSS 2012).
Do rates vary across population groups?
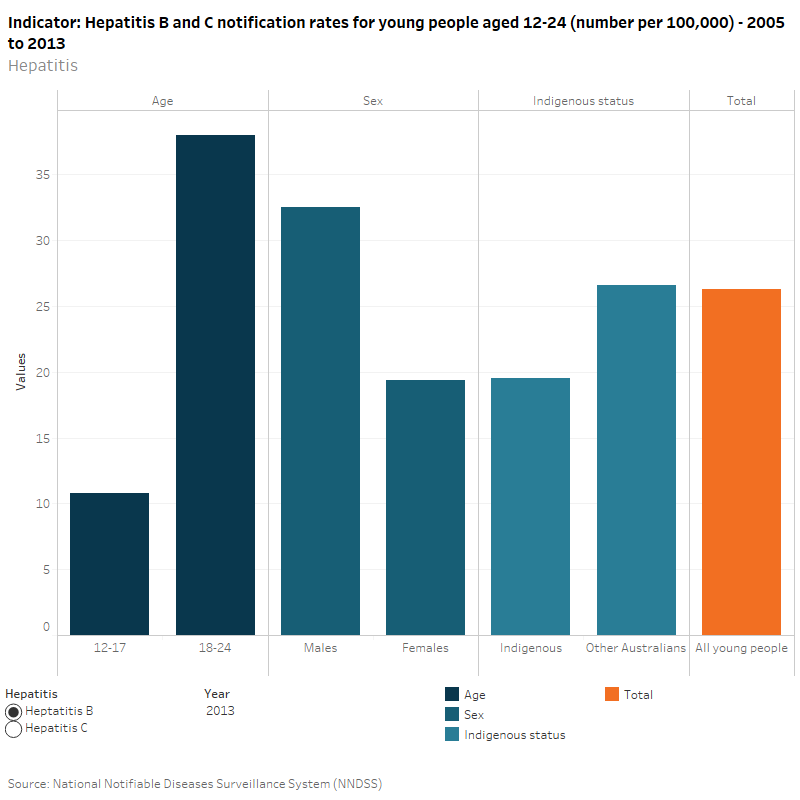
In 2013, there were 26 hepatitis B notifications per 100,000 young people. Hepatitis B notification rates for 18–24 year olds were almost 4 times as high as 12–17 years old (38 compared to 11 per 100,000). The notification rate for males was higher than the rate for females (33 compared to 20 per 100,000) and there were lower rates among Indigenous young people than Other Australian young people (20 compared with 27 per 100,000).
In 2013, the hepatitis C notification rate among all young people was 35 per 100,000. Hepatitis C notification rates were almost ten times as high in young people aged 18–24 compared to 12–17 year olds (56 per 100,000 compared to 6 per 100,000). The rate of hepatitis C infections for males was higher than females (43 per 100,000 compared to 26 per 100,000) and Indigenous young people had much higher rates than Other Australian young people (132 per 100,000 compared to 30 per 100,000).
Has there been a change over time?
The overall notification rate for hepatitis B has declined by almost 25% from 2005 to 2013 (35 per 100,000 compared to 26 per 100,000). Over this period, notification rates have declined for 18–24 year olds (from 53 per 100,000 to 38 per 100,000) whereas the rate has remained steady in 12–17 year olds at 11 per 100,000. The notification rates for males and females were similar until 2011 when the rate for males began to increase (from 26 per 100,000 to 33 per 100,000) and the rate for females continued to decrease to 19 per 100,000 in 2013. From 2005 to 2013, hepatitis B notification rate exhibited a steady decline in Other Australian young people from 33 per 100,000 to 27 per 100,000.
In 2013, the notification rate for Indigenous young people was much lower than in 2005 (20 per 100,000 compared with 72 per 100,000). Note that Indigenous coverage for years 2009 to 2011 was less than 50%, only years 2012 and 2013 are displayed in the ‘Trend by Indigenous status’ graph. Rates for years 2005 to 2008 can be seen by using the year drop down menu for the ‘Population group’ graph. The decline in hepatitis B notifications may be attributed to the national vaccination of newborns since 2000 and the adolescent vaccination program since 1997 (NNDSS, 2012).
The notification rate for hepatitis C also declined between 2005 and 2013. These trends appear to be largely driven by a decrease in the notification rate for 18–24 year olds from 86 per 100,000 to 56 per 100,000. Whilst there was a reduction in the notification rate for 12–17 year olds over this period, the rate has remained steady at 6 per 100,000 since 2008. The notification rates for males and females showed an overall decline between 2005 and 2013; however, since 2011 the rates have increased for males from 32 to 43 per 100,000 in 2013. The rate for females fluctuated between 2011 and 2013.
Between 2005 and 2013, hepatitis C notifications showed a steady decline in Other Australian young people from 47 per 100,000 to 30 per 100,000. Over this period the notification rate have been much more variable for Indigenous young people, but appear to have increased in recent years from 91 per 100,000 in 2009 to 132 per 100,000 in 2013.
Hepatitis B and C notification rates include both ‘newly acquired’ and ‘unspecified’ notifications.
In interpreting these data it is important to note that changes in notifications over time may not solely reflect changes in disease prevalence or incidence. Changes in testing policies; screening programs, including the preferential testing of high risk populations; the use of less invasive and more sensitive diagnostic tests; and periodic awareness campaigns, may influence the number of notifications that occur over time.
Determination of Indigenous status is by descent, self-identification and community. The ‘Other Australians’ population group includes both non-Indigenous youths and youths whose Indigenous status was unknown. For further information on the determination of Indigenous status, see Source data tables: NYIF indicators.
Indigenous status data were only presented in instances where the completeness of the data was greater than 50%. For more information see Source data tables: NYIF indicators.
National Notifiable Diseases Surveillance System, unpublished data
Department of Health (DoH), 2014a. The Second National Hepatitis B Strategy 2014–2017. Canberra: Commonwealth of Australia.
Department of Health, 2014b. The Fourth National Hepatitis C Strategy 2014–2017. Canberra: Commonwealth of Australia.
The Kirby Institute, 2013. HIV, viral hepatitis and sexually transmissible infections in Australia Annual Surveillance Report 2013. The Kirby Institute, The University of New South Wales, Sydney NSW 2052.
NNDSS (National Notifiable Diseases Surveillance System), 2012. NNDSS annual report writing group 2012. Australia’s notifiable disease status, 2012: annual report of the National Notifiable Diseases Surveillance System. Canberra: NNDSS.


