HIV infection
Why are HIV infection rates important?
HIV can be transmitted by sexual contact with an infected person, through infected blood products, to the fetus during pregnancy and to infants through breastfeeding by an infected mother. Those infected can remain without symptoms for many years but are still able to infect others. In most untreated cases, the virus will progressively damage the immune system over many years (by destroying white blood cells), which can lead to a person becoming susceptible to a number of serious infections and cancers. This stage is known as the acquired immune deficiency syndrome (AIDS). The prevalence of HIV in Australia is very low compared with other countries, 0.12% compared with 17.3% in South Africa and 14.9% in Zimbabwe (The Kirby Institute, 2014).
Infection with HIV cannot be cured and currently there is no vaccine to prevent it, although research into a vaccine continues. However, a wider variety of more effective antiviral medications has allowed people with HIV to lead relatively normal lives.
Research on heterosexual couples has shown that HIV treatment also acts as prevention when the HIV-positive partner is receiving anti-retroviral therapy (cART) and has an undetectable viral load. In these situations the risk of transmitting HIV to their HIV-negative partner is greatly reduced. Preliminary results from research looking at whether this also applies to gay men are promising. However, more evidence is needed to better understand the risk involved in having sex without condoms when an HIV-positive partner has undetectable viral load (Grulich et al. 2015).
Do rates vary across population groups?
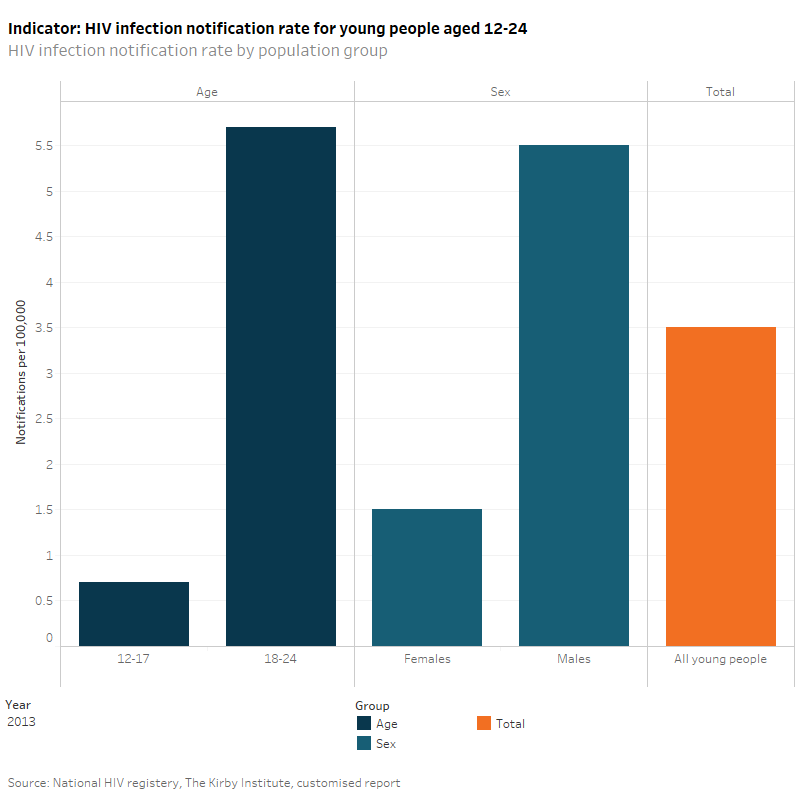
In 2013, there were 3.5 notifications per 100,000 reported for all young people aged 12–24 years, with rates rising with increasing age (0.7 per 100,000 for 12–17 year olds compared with 5.7 per 100,000 for 18–24 year olds). Males were more likely to be infected with HIV than females (5.5 per 100,000 compared to 1.5 per 100,000). For the period 2004–2013, non–Indigenous young people had higher rates of HIV infections notifications than Indigenous young people (2.9 per 100,000 compared to 2.5 per 100,000).
What is the most common mode of infection?
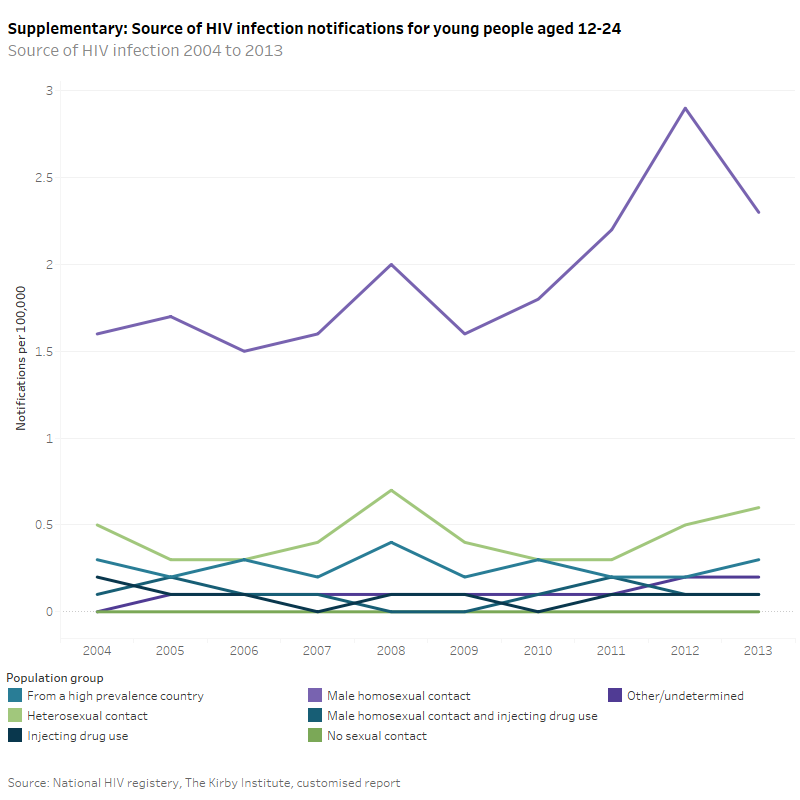
In 2013, the most common source of HIV infection was through male homosexual contact (2.3 per 100,000), followed by heterosexual contact (0.6 per 100,000) and coming from a high prevalence country (0.3 per 100,000).
Has there been a change over time?
From 2004 to 2013 the HIV notification rate has remained steady for young people aged 12–17 and females. From 2009 to 2012 there was an increasing HIV notifications rate for 18–24 year olds (4.2 per 100,000 to 6.8 per 100,000) and males (4.1 per 100,000 to 6.4 per 100,000). However, from 2012 to 2013 the HIV notification rate for young people aged 18–24 (5.7 per 100,000) and males (5.5 per 100,000) have declined. Although the 2013 HIV notification rates for young people aged 18–24 (5.7 per 100,000) and males (5.5 per 100,000) were lower than in 2012, it is too early to determine whether this constitutes a reversal of the trend.
The number of HIV infection notifications for Indigenous data were not large enough to be reported for individual years. Therefore, these data have been aggregated for 2004 to 2013.
Note that non-Indigenous includes both those born in Australia, and those born overseas. This is different to the non-Indigenous data in the Kirby Institute Annual Surveillance Report of HIV which includes non-Indigenous people born in Australia only.
National HIV Registry, The Kirby Institute, customised report
Data quality statement: Please refer to the Kirby Institute Annual Surveillance Report of HIV, viral hepatitis, STIs for further information
Grulich AE, Bavinton BR, Jin F, Prestage G, Zablotska I, Grinsztejn B, Phanuphak N, Moore R, Koelsch KK 2015. HIV transmission in male serodiscordant couples in Australia, Thailand and Brazil. Poster presentation at the Conference on Retroviruses and Opportunistic Infections (CROI 2015), Seattle, Washington 23-26 February 2015.
The Kirby Institute, 2014. HIV, viral hepatitis and sexually transmissible infections in Australia Annual Surveillance Report 2013. The Kirby Institute, The University of New South Wales, Sydney NSW 2052.


