Diabetes
Diabetes is a chronic condition marked by high levels of glucose in the blood. It is caused by the inability of the body to produce or effectively use insulin, a hormone made by the pancreas to control blood glucose levels.
Type 2 diabetes is the most common form. It involves a genetic component, but is largely preventable, and can be managed with changes to diet and physical activity, and with medications.
Diabetes is an independent risk factor for developing many forms of heart disease (Baker Heart & Diabetes Institute 2018, AIHW 2016). Over time, high blood sugar levels from diabetes can damage blood vessels in the heart, making them more likely to develop fatty deposits. Diabetes and elevated blood glucose are associated with an approximate doubling of the risk of cardiovascular disease (IDF 2019).
Diabetes and cardiovascular disease (CVD) also share risk factors. Many of the complications from having diabetes come from damage to blood vessels as a result of high blood pressure, abnormal blood lipids, and smoking.
In 2021, based on linked data from the National Diabetes Services Scheme (NDSS) and Australasian Paediatric Endocrine Group (APEG) state-based registers:
- more than 1 in 20 (1.3 million) Australians were living with diabetes. This includes people with type 1 diabetes, type 2 diabetes and other diabetes, but excludes gestational diabetes (AIHW 2023)
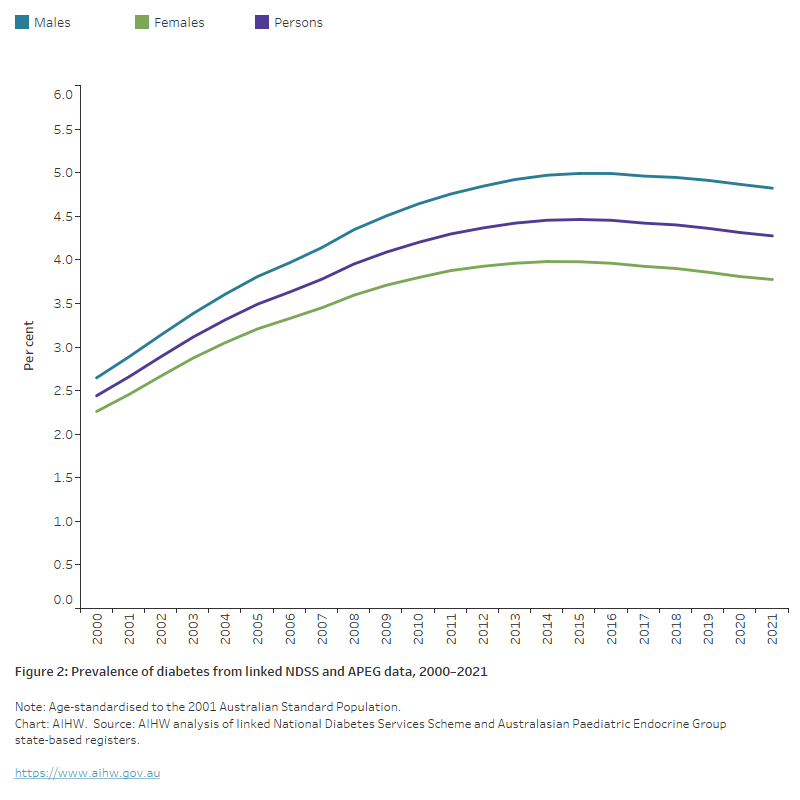
- diabetes was more common in males (4.8%) than females (3.8%) after controlling for age
- almost 1 in 5 (19.5%) Australians aged 80–84 were living with diabetes, which was almost 30 times as high as those aged under 40 (0.7%)
- age-standardised prevalence rose from 2.4% in 2000 to 4.3% in 2021. The diabetes rate remained has remained relatively stable since 2011 (Figure 1).
Information based on linked NDSS and APEG data underestimates prevalence as it does not include people with undiagnosed diabetes. The ABS 2011–12 Australian Health Survey, which included both measured and self-reported data, showed that for every 4 adults with diagnosed diabetes, there was 1 who was undiagnosed (ABS 2013).
Figure 1: Prevalence of diabetes from linked NDSS and APEG data, by sex, 2000–2021
This chart shows the estimated age–standardised proportion of people with diabetes based on data from the linked National Diabetes Services Scheme and Australasian Paediatric Endocrine Group between 2000 and 2021. The proportion increased from 2.4% in 2000 to 4.3% in 2021 and has remained relatively stable since 2014.
- both data sources are based on people who have received a formal medical diagnosis of diabetes. However, Australian studies have shown that many people are living with undiagnosed type 2 diabetes.
- registration with the NDSS is voluntary and eligible [BD1] people with type 2 diabetes are more likely to register if they access subsidised diabetes consumables to monitor their diabetes at home or require insulin. Some people may be diagnosed with diabetes and choose not to register with the scheme.
- Indigenous Australians are under-represented on the NDSS (see Using the NDSS for reporting on Indigenous Australians).
Despite these limitations, these data sources provide the best picture into the number of people living with diabetes in Australia to monitor changes in populations at risk and trends over time. Further research is required to examine whether the proportion of people with undiagnosed type 2 diabetes in Australia has changed over time and the impact of this on the prevalence of disease in Australia.
Variation between population groups
- Around 7.9% of Aboriginal and Torres Strait Islander people (64,100 people) were living with diabetes according to self-reported data from the ABS 2018–19 National Aboriginal and Torres Strait Islander Health Survey (ABS 2019). After controlling for differences in the age structures of the populations, Indigenous Australians were almost 3 times as likely to have diabetes as non-Indigenous Australians.
- The age-standardised prevalence rate of diabetes in 2021 was around 1.8 times as high among those living in the lowest socioeconomic areas as among those living in the highest socioeconomic areas. The variation in prevalence rates between the lowest and highest socioeconomic areas was slightly higher among females than males (2.0 and 1.7 times as high, respectively).
- The age-standardised prevalence rate of diabetes in 2021 was highest in Remote and very remote areas where people were 1.3 times as likely to be living with diabetes as those in Major cities. The disparity in Remote and very remote areas was more pronounced among females than males (1.6 and 1.1 times as high, respectively) (AIHW 2023).
ABS (Australian Bureau of Statistics) (2013) Australian Health Survey: biomedical results for chronic diseases, 2011–12, ABS, Australian Government.
ABS (2019) National Aboriginal and Torres Strait Islander Health Survey, 2018–19, ABS, Australian Government.
AIHW (2016) Diabetes and chronic kidney disease as risks for other diseases: Australian Burden of Disease Study 2011, AIHW, Australian Government.
AIHW (2021) Australian Burden of Disease Study 2018: interactive data on risk factor burden, AIHW, Australian Government, accessed 1 February 2022.
AIHW (2023) Diabetes facts, AIHW, Australian Government, accessed 30 June 2023.
ANZDATA (Australia and New Zealand Dialysis and Transplant Registry) (2021) ANZDATA 44th Annual Report 2021, ANZDATA, Adelaide, accessed 1 November 2021.
Baker Heart & Diabetes Institute (2018) The dark heart of type 2 diabetes, Melbourne: Baker Heart & Diabetes Institute.
IDF (International Diabetes Federation) (2019) IDF diabetes atlas, ninth edition 2019, Brussels: IDF.
Diabetes Australia (2022) What is diabetes, Diabetes Australia, accessed 12 April 2022.
Lim WH, Johnson DW, Hawley C, Lok C, Polkinghorne KR, Roberts MA et al. (2018) Type 2 diabetes in patients with end-stage kidney disease: influence on cardiovascular disease-related mortality risk. Medical Journal of Australia, 209:440–446, doi: 10.5694/mja18.00195.


