Contact with objects
Citation
AIHW (Australian Institute of Health and Welfare) (2025) Contact with objects, AIHW, Australian Government, accessed 5 June 2026.
This article is part of Injury in Australia
Unintentional causes
Intentional causes
-
Hospitalisations 2023–24
80,705 injury hospitalisations
14% of all injury hospitalisations
299.7 hospitalisations per 100,000 population
-
Deaths 2022–23
105 deaths
0.7% of all injury deaths
0.4 deaths per 100,000 population
-
Males
The highest rate of injury hospitalisations in 2023–24 was among males (435.5 hospitalisations and 0.7 deaths per 100,000 population)
-
Age group
The highest rates of injury hospitalisations in 2023–24 were among 15–24-year olds (367.3 hospitalisations per 100,000 population), while the highest rate of injury death was among those aged 65+ (0.7 deaths per 100,000 population)
-
Object type
The highest rate of contact with object injury hospitalisations was caused by contact with other sharp object* (54.1 hospitalisations per 100,000 population)
* this category includes all sharp objects except sharp glass
Contact with objects (or Exposure to inanimate mechanical forces in ICD-10-AM) includes harmful contact with every day or industrial objects such as knives, tools, machines, and sports equipment. It also includes unintentional injuries caused by guns and non-heat-related injuries caused by explosions. For heat-related injuries, see Thermal causes. Transport accidents are covered in their own category, and so are excluded here.
Hospitalisations where the cause of injury is W44 Foreign body entering into or through eye or natural orifice and the type of injury is a Foreign body in the respiratory tract (T17.2–T17.8) were included in this category until the June 2022 release of this report, after which they were re-classified into Choking and suffocation.
This article covers accidental cases of injury hospitalisation or death caused by contact with objects. Intentional injuries are included under Self-harm and suicide or Assault and homicide.
Injuries by type of object
There is a considerable diversity of inanimate objects that can cause injuries. Hospitalisations record the type of object responsible for the injury, classified according to ICD-10-AM codes in the W20-W49 range. In 2023–24, hospitalisations most often resulted from the following object types (Figure 1):
- contact with other sharp object(s) (54.1 per 100,000 population)
- striking against or struck by other object(s) (44.3 per 100,000 population)
- foreign body entering into or through eye or natural orifice (31.4 per 100,000 population).
Figure 1: Number and age-standardised rate of contact with object injury hospitalisations, by type of object involved, Australia, 2023–24

Notes:
- ASR is the age-standardised rate per 100,000 persons.
- Only object types causing more than 100 hospitalisations in 2023-24 are shown. For a comprehensive list of all object types, refer to supplementary data tables.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
For some object type categories, it is possible to provide further detail about the specific type of object responsible for the injury hospitalisation. Click on the categories below for more detail on injuries caused by:
Figure 1a: Number and age-standardised rate of contact with sharp glass injury hospitalisations, by type of sharp glass, Australia, 2023–24
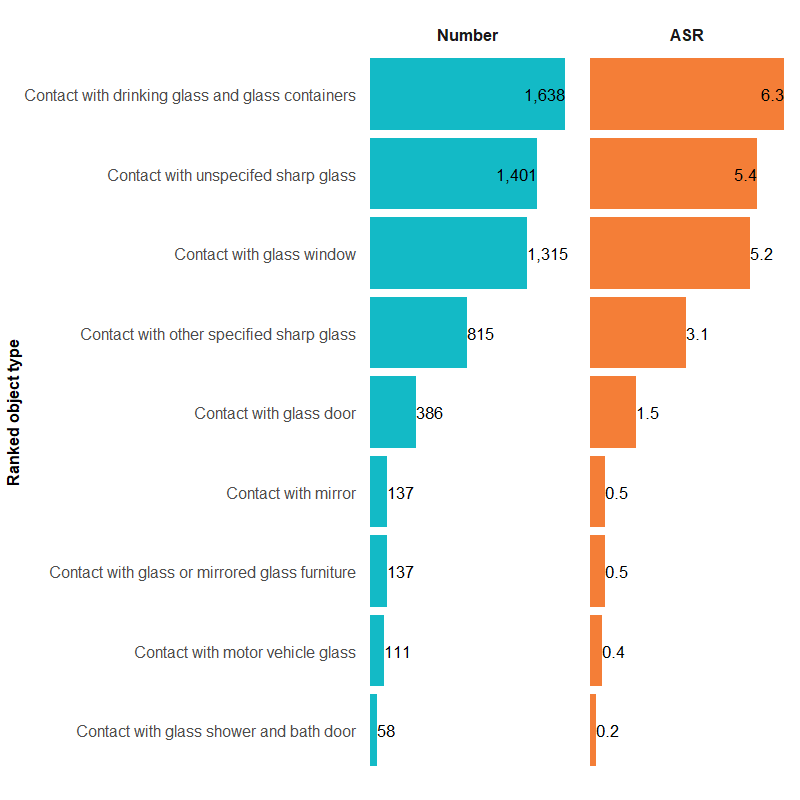
Figure 1b: Number and age-standardised rate of contact with sharp object injury hospitalisations, by type of sharp object, Australia, 2023–24

Notes:
- This category encompasses all sharp objects with the exception of sharp glass (see Figure 1a).
Figure 1c: Number and age-standardised rate of contact with powered hand tool and household machinery injury hospitalisations, by type of tool or machinery, Australia, 2023–24
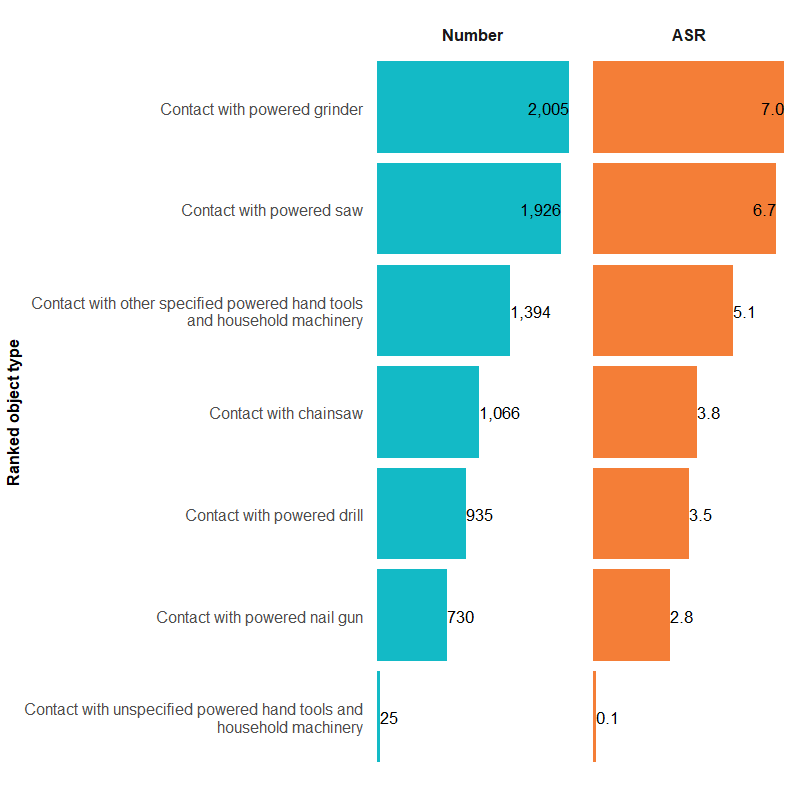
Figure 1d: Number and age-standardised rate of contact with other and unspecified machinery injury hospitalisations, by type of machinery, Australia, 2023–24
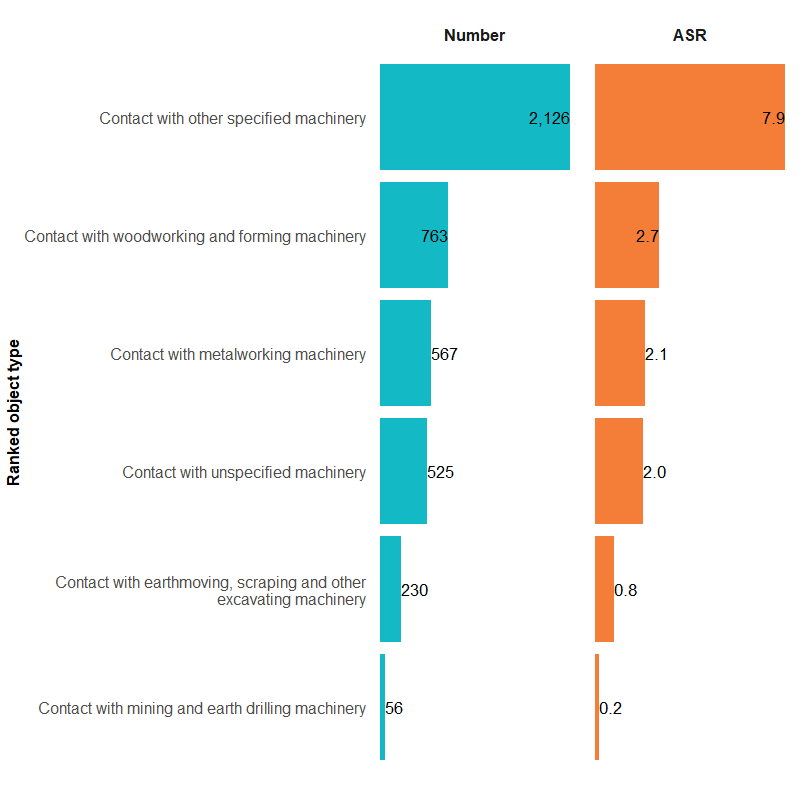
For more detail, see Supplementary Data tables.
Trends over time
There is a break in the time series for hospitalisations between 2016–17 and 2017–18 due to a change in data collection methods (see the technical notes for details).
The number of object injury hospitalisations has generally increased over the past decade, with the age-standardised rate ranging between 288.5 and 329.8 (Figure 3). Between 2017–18 and 2023–24, the rate increased by an annual average of 0.2%. There was a sharp increase in the rate in 2020–21, most likely resulting from high rates of object-related injuries at home during the COVID-19 pandemic (see What injuries occur? for more detail). Rates have since returned to their pre-pandemic levels.
Figure 3: Number and age-standardised rate of injury hospitalisations due to contact with objects, by financial year, Australia
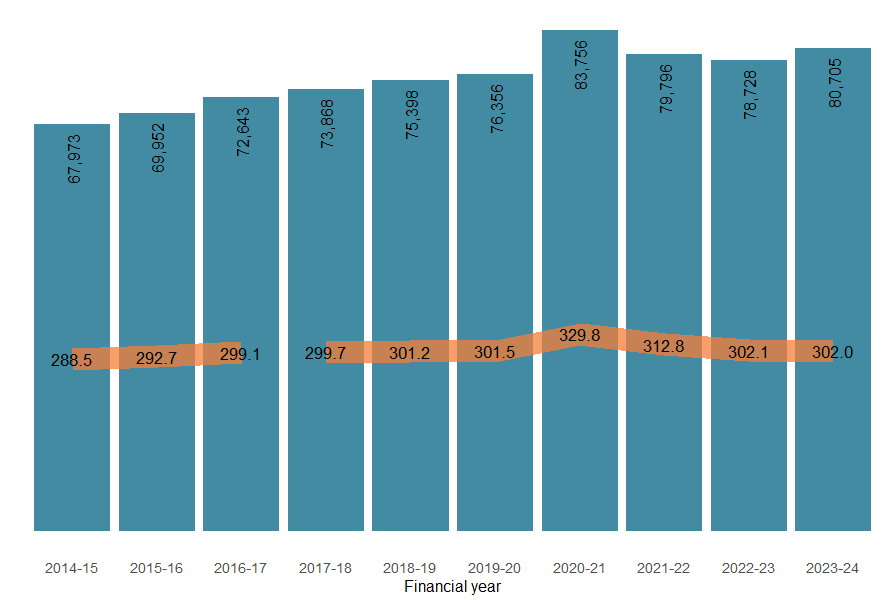
Notes:
- Bars represent numbers of hospitalisations, lines represent ASRs.
- ASR is the age-standardised rate per 100,000 population.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
The number of deaths caused by contact with objects has generally remained stable over time, with the exception of a peak in 2019–20 (Figure 4).
Figure 3: Number and age-standardised rate of injury hospitalisations due to contact with objects, by financial year, Australia
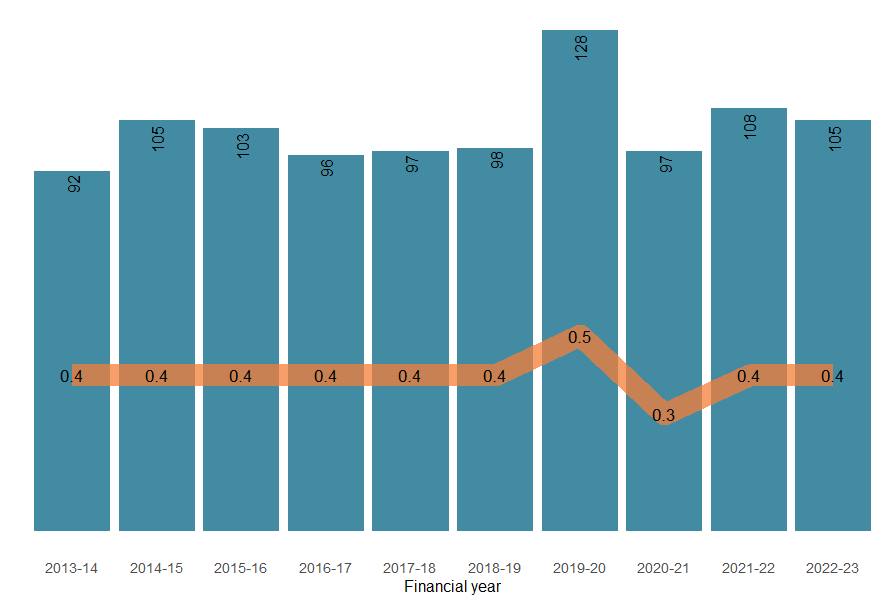
Notes:
- Bars represent numbers of hospitalisations, lines represent ASRs.
- ASR is the age-standardised rate per 100,000 population.
Sources: AIHW National Mortality Database and ABS National, state and territory population.
While all object types showed an increase in the rate of injury hospitalisations in 2020-21, detailed trends varied depending on the type of object involved (Figure 5). For example:
-
Rates of injury hospitalisations caused by contact with other sharp objects or contact with powered hand tools and household machinery have declined since their 2020–21 peak, and returned near their pre-pandemic levels
-
Rates of injury hospitalisations caused by contact with sharp glass or contact with other and unspecified machinery have declined more sharply since their 2020–21 peak, and are now less likely than they were before 2020
-
Rates of injury hospitalisations caused by being caught, crushed, jammed or pinched in or between objects have been increasing over the past decade, and rates remained higher in 2023–24 than they were before 2020
Figure 5: Age-standardised rates of object-related injury hospitalisation by type of object and financial year, Australia
Figure 5 shows that for most object types, the rate of injury hospitalisations has peaked in 2020-21.

Notes:
- Age-standardised rates per 100,000 population
- Due to a change in coding practices, data for the Contact with other sharp object(s) and Foreign body or object entering through skin are only presented from 2015–16.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
Seasonality
Injury hospitalisations due to contact with objects in 2023–24 followed similar patterns to the previous 5 years, with higher rates of injury hospitalisations during warmer months, from October to March (Figure 6).
Figure 6: Number of injury hospitalisations caused by contact with objects, by calendar month, 2023–24
Figure 6 shows the seasonal pattern of object injury hospitalisations by type of object.

Source: AIHW National Hospital Morbidity Database.
Some object types were associated with stronger seasonal patterns. For example, injury hospitalisations:
- caused by contact with other powered hand tools and household machinery or contact with non-powered hand tools are less likely to occur in summer months
- caused by contact with sharp glass are more likely in the summer months
- caused by contact with powered lawnmower are more likely to occur between October and March, and showed a sharp peak in January in 2023–24.
What injuries occur?
Body part injured and type of injury
In 2023–24, the three body parts most frequently injured in object injury hospitalisations (Figure 7) were:
-
Hospitalisations 2023–24
The 3 body parts most frequently injured in object injury hospitalisations were:
- wrist and hand (159.2 per 100,000 population)
- head and neck (39.3 per 100,000 population)
- ankle and foot (31.1 per 100,000 population)
Across different types of objects, wrist and hand injuries were the most common (Figure 7). Exceptions were:
- head and neck injuries were most common for injury hospitalisations caused by striking against or struck by other object, struck by thrown, projected or falling object, explosion and rupture of gas cylinder and explosion of other materials
- shoulder and upper limb injuries were most common for contact with hypodermic needle hospitalisations
- hip and lower limb injuries were most common for discharge from other and unspecified firearms hospitalisations.
Figure 7: Injury hospitalisations due to contact with objects by main body part injured, 2023–24

Notes:
- Main body part relates to the principal reason for hospitalisation.
- Number and percentage of injuries classified as Other, multiple and incompletely specified body regions or Injuries not described in terms of body region not shown.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
The most common types of injury for people who were hospitalised due to contact with objects were:
-
Hospitalisations 2023–24
The most common types of injury for people who were hospitalised due to contact with objects were:
- Open wounds (36.8%)
- Fractures (19.4%)
- Soft-tissue injuries (12.2%)
The most frequent injuries by body part were open wounds to the wrist and hand, and fractures to the wrist and hand (Figure 8).
Figure 8: Age-standardised rates of injury hospitalisations due to contact with objects, by type of injury and body part injured, Australia, 2023–24
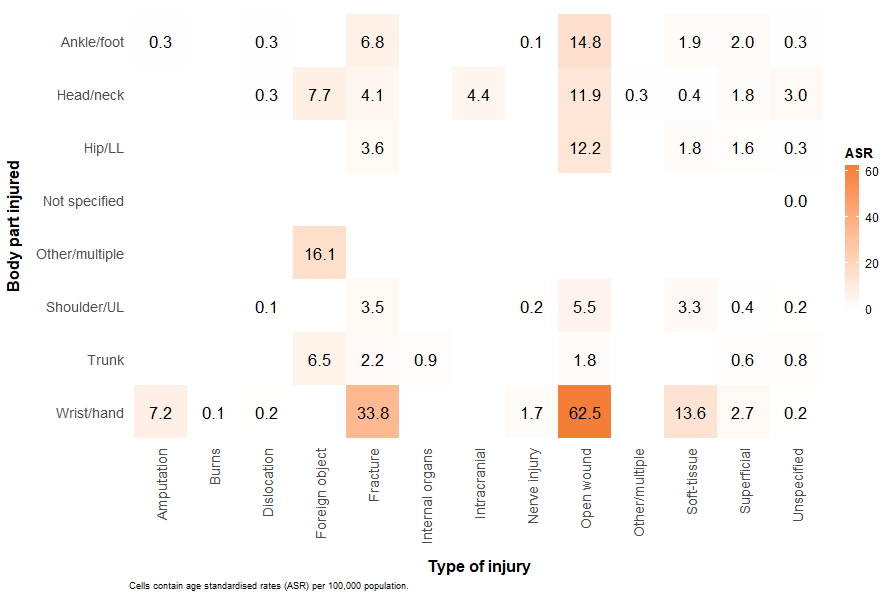
Notes:
- Matrix of age-standardised rates of body parts injured by type of injury.
- Age-standardised rates per 100,000 population.
- Rates under 1 are omitted.
- Body part injured: Trunk includes thorax, abdomen, lower back, lumbar spine & pelvis), Shoulder and upper limb excludes hand and wrist, Other includes multiple and incompletely specified body regions, Not specified includes injuries not described in terms of body location, Hip and lower limb excludes ankle and foot.
- Type of injury: Other/multiple includes other specified and/or multiple injuries.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
Activity while injured and place of occurrence
49.2% of activity records and 54.4% of place of occurrence records were missing for object-related hospitalisations. The figures below should therefore be used with caution.
-
Home was the most commonly specified place of occurrence (25.4%)
-
Unpaid work and learning was the most commonly specified activity undertaken when injured (14.4%)
Over the past decade, object-related injury hospitalisations have been most likely where the injury occurred during unpaid work and learning activities (Figure 9). Rates of injury hospitalisations caused by this type of activity peaked during the COVID-19 period, and have since returned to the overall pre-pandemic pattern of gradual year-on-year increase. The other type of activity exhibiting a pandemic period peak in injury hospitalisations is construction work.
Figure 9: Age-standardised rate of injury hospitalisations due to contact with objects, by recorded activity at the time of injury, Australia, 2014–15 to 2023–24
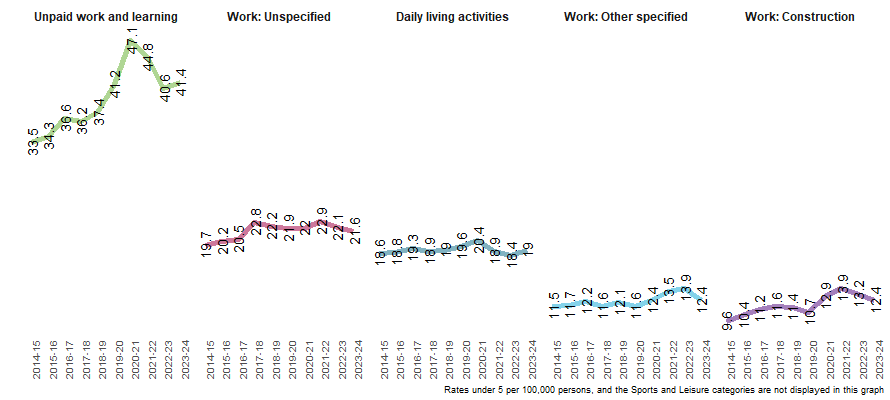
Note: Rates are age-standardised per 100,000 population
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
Object-related injury hospitalisation rates were highest in the home over the past decade, with rates increasing over the decade from 65.8 to 75.2 per 100,000 population (Figure 10). Minimal observable changes in rates of injury hospitalisations occurred at other places of occurrence.
Figure 10: Age-standardised rate of injury hospitalisations due to contact with objects, by recorded place of occurrence, Australia, 2014–15 to 2023–24
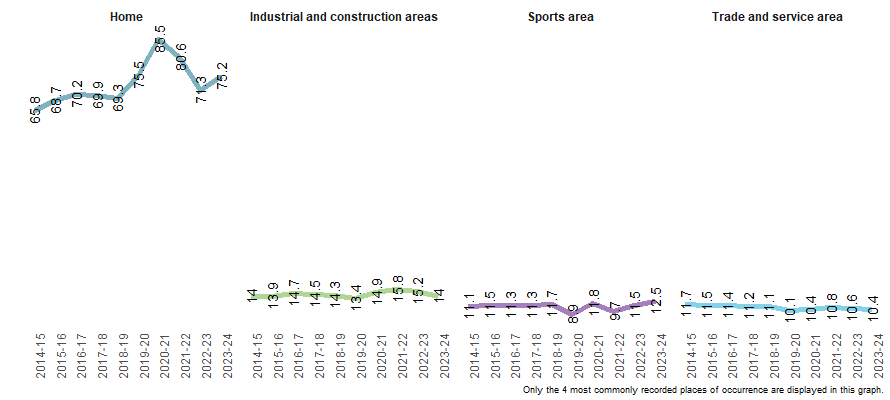
Note: Rates are age-standardised per 100,000 population.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
Rates of injuries occurring at home and associated with unpaid work and learning activity peaked during the pandemic period before returning to pre-pandemic trends of a gradual year-on-year increase. This is likely related to increased time spent on personal activities at home during the COVID-19 pandemic.
Severity
There are many ways that the severity, or seriousness, of an injury can be measured. Some of the ways to measure the severity of hospitalised injuries are:
- number of days in hospital
- time in an intensive care unit (ICU)
- time on a ventilator
- in-hospital deaths.
Object injury hospitalisations were less severe than the average of all hospitalised injuries in 2023–24 (Table 1).
Severity measure | Contact with objects | All injuries |
|---|---|---|
Average number of days in hospital | 1.7 | 3.4 |
Percentage of cases with time in an ICU (%) | 0.4 | 2.1 |
Percentage of cases with time on ventilator (%) | 0.2 | 1.2 |
In-hospital deaths (per 1,000 cases) | 0.7 | 5.9 |
Note: Average number of days in hospital (length of stay) includes admissions that are transfers from one hospital to another or transfers from one admitted care type to another within the same hospital, except where care involves rehabilitation procedures.
Source: AIHW National Hospital Morbidity Database.
Age and sex
Males were overall much more likely to be hospitalised with injuries from contact with objects (Figure 11).
-
Object-related injury hospitalisations 2023–24
- the highest number of cases was for males (58,032 cases, 71%)
- the age-standardised rate for males (435.5 per 100,000) was 2.6 times that for females (168.9 per 100,000)
- people aged 15–24 had the highest injury hospitalisation rate.
-
Object-related injury deaths, 2022–23
- the highest number of deaths was for males (91 deaths, 86%)
- people aged 65+ had the highest rate of injury death.
Figure 11: Age-standardised and crude rates of injury hospitalisations caused by contact with objects, by age group, sex and financial year, Australia
Figure 11 is a line chart of object injury hospitalisations by sex and age over the last decade. Rates were higher in males and in persons aged 15 to 24.

Notes:
- Rates by sex are age-standardised per 100,000 population, rates by age group are crude rates per 100,000 population.
- Due to a change in coding practices, data for the Contact with other sharp object(s) and Foreign body or object entering through skin are only presented from 2015-16.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
-
For all types of objects, rates of injury hospitalisation were higher in males compared to females
-
Injury hospitalisations caused by being caught, crushed, jammed or pinched in between objects were almost twice as common in children aged 0-4 (72.4 per 100,000) as in any other age group
-
Injuries caused by striking against or struck by sports equipment are most common in people aged 5-14 and 15-24 (around 35 per 100,000), with rates decreasing sharply in older age groups
-
Injuries caused by contact with sharp glass have been most likely in people aged 15-24, and the hospitalisation rate within that age group has been decreasing since 2020-21 (from 59.9 to 39.4 per 100,000)
-
- Other powered hand tools & household machinery injuries are commonest among 45-64 year olds (41 per 100,000)
- Other adults have similar rates (33-35 per 100,000)
- Children aged under 15 years have substantially lower rates (< 4 per 100,000)
First Nations people
Among Aboriginal and Torres Strait Islander (First Nations) people:
- there were 5,421 injury hospitalisations due to contact with objects in 2023–24 (a crude rate of 526.1 per 100,000)
- males were twice as likely as females to be hospitalised (693.7 and 356.7 per 100,000 population)
- hospitalisation rates were highest among people aged 25–44 (Figure 12)
- there were 5 injury deaths due to contact with objects in 2022–23.
Figure 12: Injury hospitalisations due to contact with objects among First Nations people, by age and sex, Australia, 2023–24

Note: Crude rates per 100,000 population.
Source: AIHW National Hospital Morbidity Database and ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
Comparison between First Nations people and non-Indigenous Australians
-
Hospitalisations 2023–24
First Nations people, when compared with non-Indigenous Australians, were 1.8 times as likely to be hospitalised for object-related injuries
Figure 13: Age-standardised rates of injury hospitalisations caused by contact with objects, Indigenous status and financial year, Australia
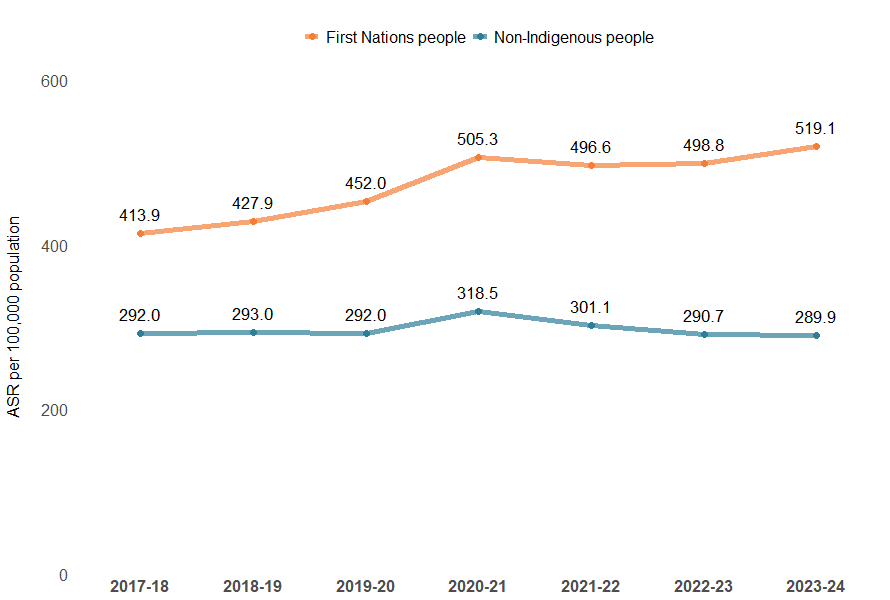
Notes:
- Age-standardised rates per 100,000 population.
- ‘Non-Indigenous people’ excludes cases where Indigenous status is missing or not stated.
Sources: AIHW National Hospital Morbidity Database and ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
The rate of object injury hospitalisations was highest among the 25–44 age group for First Nations people, and the 15–24 age group for non-Indigenous Australians (Figure 14).
Figure 14: Injury hospitalisations due to contact with objects, by Indigenous status and age group, Australia, 2023–24
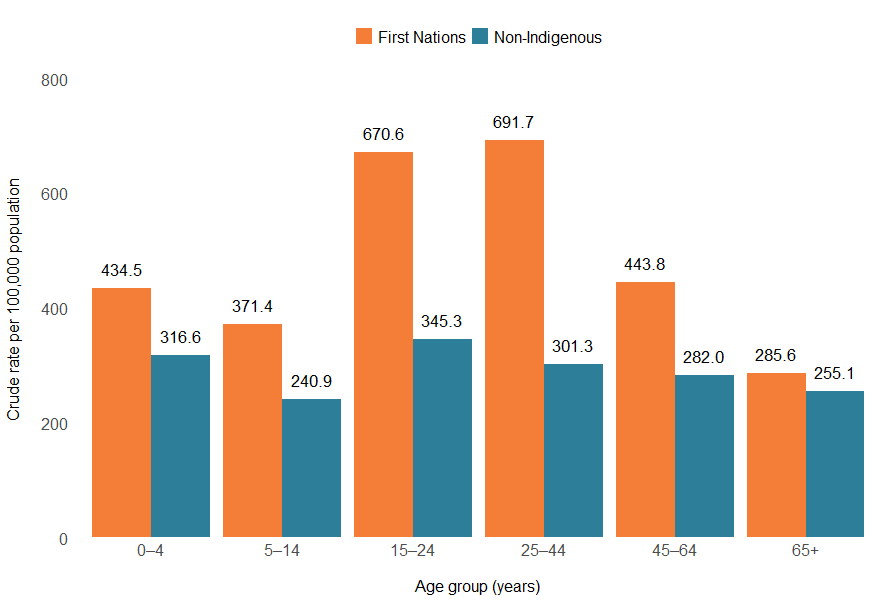
Notes:
- Crude rates per 100,000 population.
- ‘Non-Indigenous’ excludes cases where Indigenous status is missing or not stated.
Sources: AIHW National Hospital Morbidity Database and ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
For more detail, see Supplementary Data tables.
State and territory
The states and territories with the highest rates of object-related injury hospitalisation in 2023–24 were:
- Northern Territory (500.8 per 100,000)
- Queensland (343.8 per 100,000)
- Australian Capital Territory (311.2 per 100,000) (Figure 15).
Rates of injury death cannot be reliably calculated in most states due to low numbers. In Figure 15, we show the number of object-related injury deaths in each state and territory in 2022–23.
Figure 15: Age-standardised rate of injury hospitalisations (2023–24), and number of injury deaths (2022–23), due to contact with objects, by state of usual residence, Australia
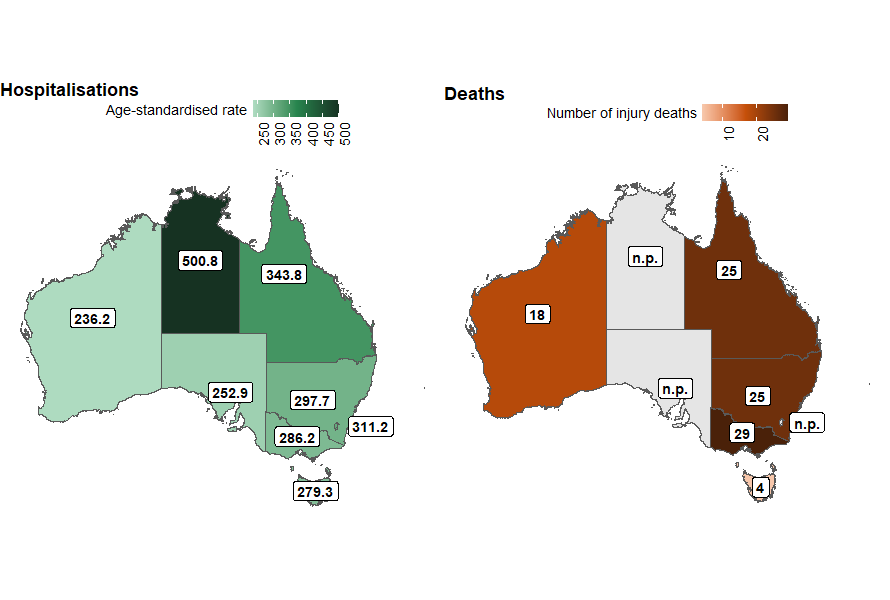
Notes:
- Injury hospitalisation rates are age-standardised per 100,000 population
- The number of injury deaths in each state is presented, as numbers are too low for a reliable rate calculation.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database and ABS National, state and territory population.
There are some differences in trends across states by type of contact with objects involved (Figure 16). As compared to the previous 5-year average, 2023–24 saw a decrease in overall contact with objects across all states and territories except for Tasmania. Contact with other and unspecified machinery injuries decreased across all states and territories. Other decreases that were seen across most states and territories include:
- Contact with other powered hand tools and household machinery
- Contact with other shard objects
- Contact with sharp glass
- Foreign body or object entering through skin
- Striking against or struck by other objects
- Struck by thrown, projected or falling object.
Figure 16: Percentage difference in age-standardised rates of injury hospitalisations due to contact with objects, compared to the previous 5-year average, by state or territory of usual residence, Australia, 2023–24
Map of Australia showing trends in age-standardised rate of hospitalisation due to contact with objects by state or territory by type of object.

Notes:
- State and territory refers to the state and territory of usual residence for the individual.
- Age-standardised rates per 100,000 population.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
For more information see the state supplementary data tables and the geography dashboard.
Remoteness
Areas of Australia which are more remote tend to have higher rates of hospitalisation and death from injury than less remote areas.
-
Hospitalisations 2023–24
People living in Very remote areas, when compared with people living in Major cities, were twice as likely to be hospitalised for object-related injuries.
Rates shown are age-standardised per 100,000 population
While most types of objects cause higher rates of hospitalisation in more remote regions, some object types exhibit different patterns (Figure 17):
- Remote areas had the highest rate of injuries caused by foreign body entering into or through eye or natural orifice or foreign body or object entering through skin
- Outer regional areas had the highest rate of contact with other and unspecified machinery-related hospitalisations
- Inner regional areas had the highest rate of contact with other powered hand tools and household machinery
Figure 17: Age-standardised rates of injury hospitalisations due to contact with objects, by remoteness, type of object and financial year, Australia

Notes:
- Age-standardised rates per 100,000 population.
- Due to a change in coding practices, data for the Contact with other sharp object(s) and Foreign body or object entering through skin are only presented from 2015–16.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
For information on how statistics are calculated by remoteness, see the technical notes.
Socioeconomic areas
-

People living in the most socioeconomically disadvantaged areas of Australia, compared to the least socioeconomically disadvantaged, were 1.4 times as likely to be hospitalised for object-related injuries in 2023–24.
Most object types are associated with higher rates of injury hospitalisation in more socioeconomically disadvantaged areas (Figure 18). The only exception concerns injuries caused by striking or being struck by sports equipment, with rates highest in least disadvantaged areas (22.7 per 100,000), and decreasing with socioeconomic disadvantage.
Figure 18: Age-standardised rates of injury hospitalisations due to contact with objects, by socioeconomic areas, type of object and financial year, Australia

Notes:
- Age-standardised rates per 100,000 population
- Due to a change in coding practices, data for the Contact with other sharp object(s) and Foreign body or object entering through skin are only presented from 2015–16.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
For more detail, see Supplementary data tables.
The following are recent publications. Search Reports for older publications.


