Accidental poisoning
Citation
AIHW (Australian Institute of Health and Welfare) (2025) Accidental poisoning, AIHW, Australian Government, accessed 10 June 2026.
This article is part of Injury in Australia
Unintentional causes
Intentional causes
Accidental poisoning is caused by exposure to a substance in an amount that unintentionally causes harm. It is the ninth leading cause of injury hospitalisations and the fifth leading cause of injury deaths.
Accidental poisoning resulted in:
-
Hospitalisations 2023–24
10,121 hospitalisations
1.8% of all injury hospitalisations
Age-standardised rate of 37.1 per 100,000 population
-
Deaths 2022–23
1,399 deaths
9.1% of all injury deaths
Age-standardised rate of 5.4 per 100,000 population
Definitions
This article describes accidental cases of poisoning resulting in hospitalisation or death. Intentional poisoning injuries are included under Self-harm injuries and suicide or Assault and homicide. Poisoning cases where intent cannot be determined are described in the article on Undetermined or other unintentional causes. As intent is often difficult to ascertain in cases of poisoning, a substantial number of hospitalisations and deaths related to poisoning are categorised as Undetermined intent.
Injury hospitalisations due to accidental poisoning mostly involve pharmaceutical substances as the harmful substance. In this article, we only describe the type of substance responsible for the accidental poisoning, without consideration for the means through which the substance was obtained (including regular prescriptions, over-the-counter medication, or illicitly obtained substances). We note however that the adverse side effects of correctly prescribed medication consumed at the correct dosage are not in the scope of this report.
For more information on the health impact of alcohol and other drugs, see the AIHW reports on Alcohol, tobacco and other drugs in Australia, and on Illicit use of drugs.
Hospitalised injury cases are described using ICD-10-AM. ICD-10-AM external cause codes define the following 10 categories for accidental poisoning:
- Non-opioid analgesics, antipyretics and antirheumatics, including (but not limited to) nonsteroidal anti-inflammatory drugs (NSAIDs)
- Antiepileptics, sedatives and psychotropics, including (but not limited to) antidepressants, psychostimulants and tranquilisers
- Narcotics, opioids and hallucinogens, including (but not limited to) opioids such as codeine, morphine and heroin
- Other drugs acting on the autonomic nervous system
- Other and unspecified drugs and biological substances, including pharmaceutical and biological substances not classified elsewhere, such as anaesthetics, antibiotics and other anti-infectives, hormones and their synthetic substitutes and antagonists, and others. This category is also used in mortality data (but not in hospitalisations data) to record cases of deaths caused by multi-drug toxicity
- Alcohol
- Organic solvents, including (but not limited to) petroleum and its derivatives, and including vapours from organic solvents
- Other gases and vapours, including (but not limited to) carbon monoxide and exhaust fumes
- Pesticides
- Other and unspecified noxious substances, including (but not limited to) chemicals not elsewhere classified such as paints or corrosive substances.
This report mostly refers to these 10 categories to describe the type of substance(s) responsible for cases of accidental poisoning injury hospitalisations or deaths. Some hospitalisation records include further detail of substances in the primary diagnosis codes. Where available, these are further described for selected substances of interest.
Substances involved in accidental poisoning
In 2023–24, other and unspecified drugs and biological substances, antiepileptics, sedatives and psychotropics and narcotics, opioids and hallucinogens were the categories of substances most often associated with accidental poisoning injury hospitalisations (Figure 1a).
Figure 1a: Number and age-standardised rate of accidental poisoning injury hospitalisations, by type of substance involved, Australia, 2023–24
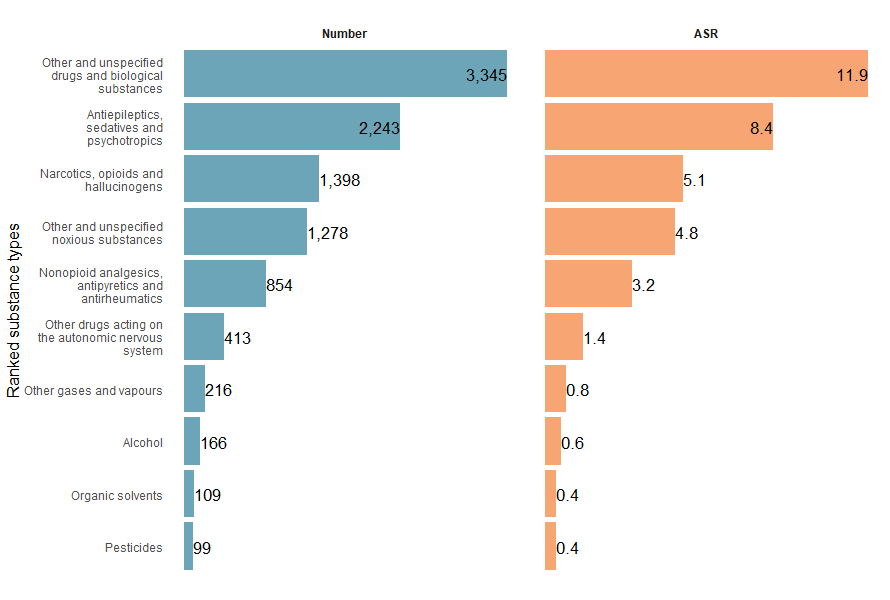
Note: ASR is the age-standardised rate of hospitalisations per 100,000 population.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
In 2023–24, gamma hydroxybutyrate (GHB), agents primarily affecting the cardiovascular system and salicylates, aminophenols & pyrazolones were the detailed substances most often recorded in accidental poisoning injury hospitalisations (Figure 1b).
Figure 1b: Number and age-standardised rate of accidental poisoning injury hospitalisations, by detailed substance involved, Australia, 2023–24
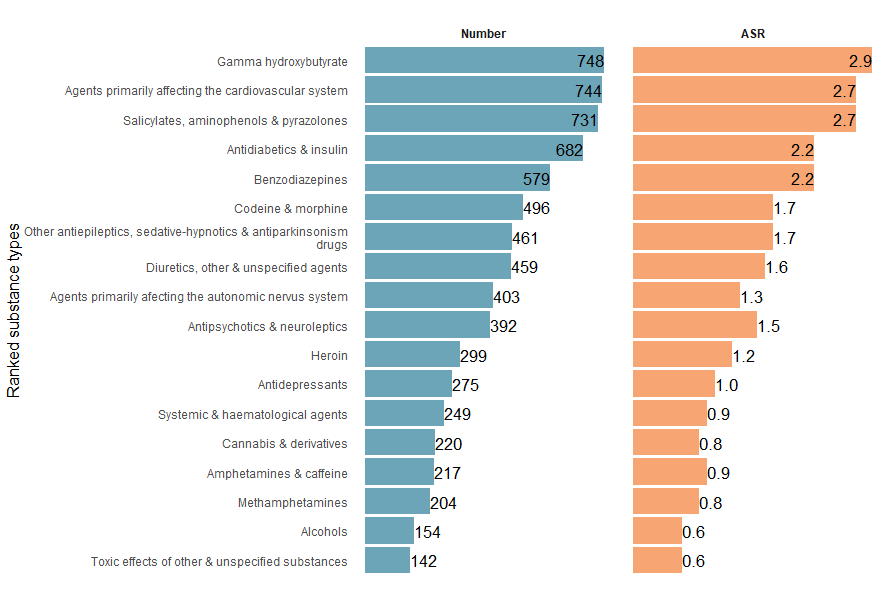
Notes:
- ASR is the age-standardised rate per 100,000 population.
- Only substances where more than 100 hospitalisations were recorded are displayed.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
In 2022–23, most accidental poisoning deaths were caused by other and unspecified drugs and biological substances (Figure 2). It should be noted, however, that the scope for this specific category differs between hospitalisations and deaths data. In both cases, this category includes cases of morbidity or mortality caused by drugs or biological substances not classified elsewhere. However, for mortality coding specifically, this category also includes poisoning deaths caused by multiple drugs or biological substances. Due to this difference in coding practices, the relative contributions of this specific substance category cannot be compared between hospitalisations and deaths data.
In 2022–23, most accidental poisoning deaths were caused by other and unspecified drugs and biological substances, antiepileptic, sedative and psychotropic drugs and narcotics, opioids and hallucinogens (Figure 2).
Figure 2: Number and age-standardised rate of accidental poisoning deaths by type of substance involved, Australia, 2022–23

Notes:
- ASR is the age standardised rate per 100,000 population.
- ASRs where the numerator is less than 20 are not shown due to data volatility.
Sources: AIHW National Mortality Database and ABS National, state and territory population.
For more detail, see accidental poisoning supplementary data tables.
Trends over time
There is a break in the time series for hospitalisations between 2016–17 and 2017–18 due to a change in data collection methods (see the technical notes for details).
The number of accidental poisoning hospitalisations has generally decreased over the past decade although 2023–24 saw an increase from the previous 2 years (Figure 3). Between 2017–18 and 2023–24, the rate decreased by an annual average of 1.9%. In 2023–24 however, the hospitalisation rate increased by 11% compared to the previous year
Figure 3: Number and age-standardised rate of accidental poisoning injury hospitalisations, by financial year, Australia
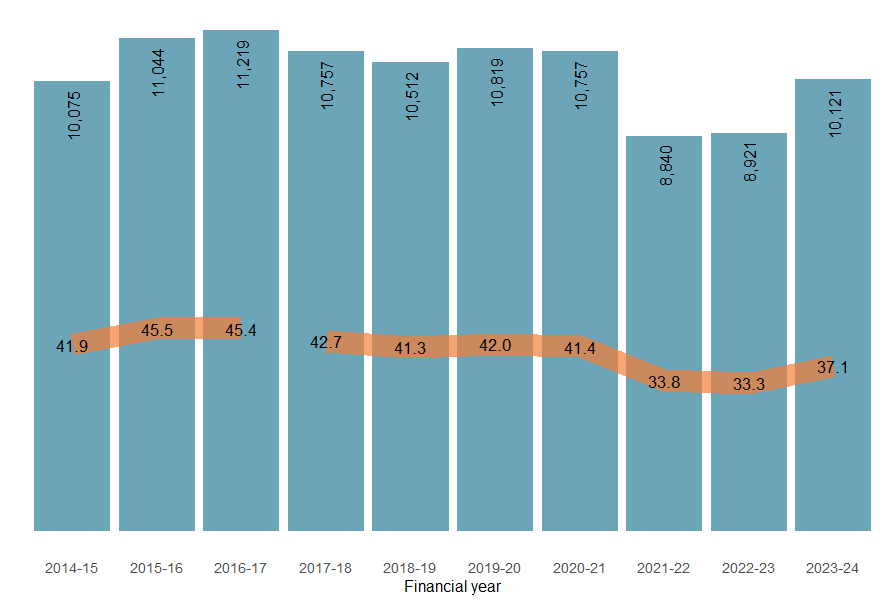
Notes:
- Bars represent numbers of hospitalisations, lines represent ASRs.
- ASR is the age-standardised rate per 100,000 population.
Source: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
The number of deaths caused by accidental poisoning have generally increased over time, although fewer were recorded in 2022–23 as compared to the previous year (Figure 4). For accidental poisoning deaths between 2013–14 and 2022–23, the age-standardised rate decreased marginally by an annual average of 0.5% (Figure 4). However, in 2022–23, the rate of accidental poisoning deaths has decreased by 11% compared to the previous year.
Figure 4: Number and age-standardised rate of accidental poisoning injury deaths, by financial year, Australia
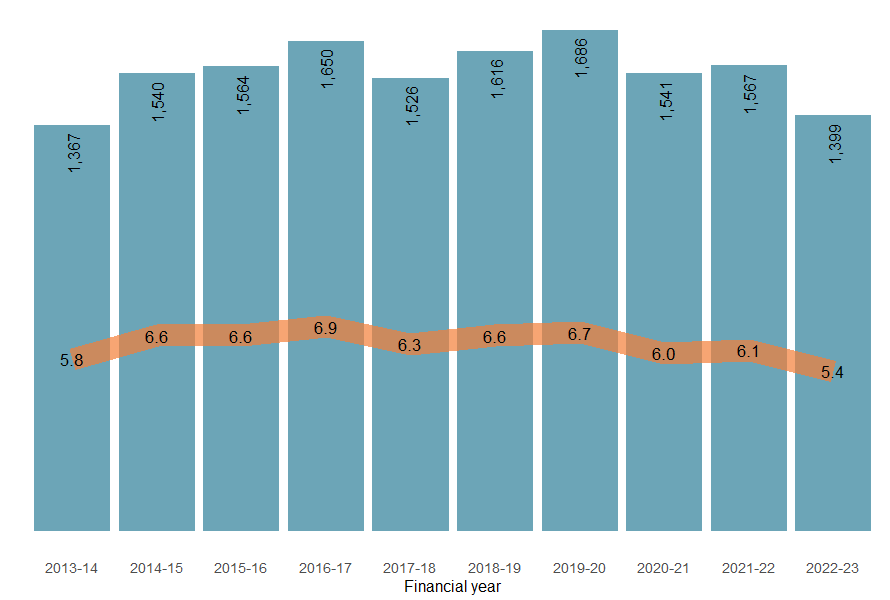
Notes:
- Bars represent numbers of hospitalisations, lines represent ASRs.
- ASR is the age-standardised rate per 100,000 population.
Source: AIHW National Mortality Database.
Among the top causes of accidental poisoning compared to the previous 5-year average, hospitalisation rates due to narcotics, opioids and hallucinogens changed the most (18% decrease) followed by other and unspecified drugs and biological substances (16% increase) (Figure 5a).
Figure 5a: Age-standardised rates of accidental poisoning hospitalisations (2014–15 to 2023–24) and deaths (2013–14 to 2022–23) by type of substance, Australia
Rates of hospitalisation have decreased for most poison types over the last decade, while mortality rates have remained mostly stable.
Notes:
- ASR is the age-standardised rate per 100,000 population.
- ASRs where the numerator is less than 20 are not shown due to data volatility.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database and ABS National, state and territory population.
Widely varying trends of injury hospitalisation are observed over the past decade for different kinds of substances (Figure 5b). One of the biggest recent changes in accidental injury hospitalisations is observed where gamma-hydroxybutyrate (GHB) is recorded as the primary cause of injury. This has increased notably since 2021–22 to 748 injury hospitalisations (an age-standardised rate of 2.9 per 100,000 population) in 2023–24. Other illicit substances where numbers and rates of accidental poisoning injury hospitalisations have recently increased include cocaine, ecstasy/MDMA and methamphetamines. For pharmacological substances, the highest number of accidental poisoning injury hospitalisations in 2023–24 were due to agents primarily affecting the cardiovascular system, with 744 hospitalisations.
Figure 5b: Numbers and age-standardised rates of accidental poisoning hospitalisations by detailed substance, Australia, 2014–15 to 2023–24
Interactive graphs showing the ranking and trends of different substances recorded in the primary diagnoses as causing accidental poisoning hospitalisations over the past decade

Notes: This figure only presents cases where the substance was identifiable within the primary diagnosis of injury ICD-10-AM code.
Source: AIHW National Hospital Morbidity Database.
For more detail, see accidental poisoning supplementary data tables.
Seasonality
Injury hospitalisations due to all poisons during 2023–24 were similar to the previous 5-year average, being slightly higher in spring and summer than autumn and winter (Figure 6). In the category with the largest numbers of hospitalisations (other and unspecified drugs, medicaments and biological substances) higher numbers of cases were hospitalised in every month of 2023–24 as compared to the previous 5-year average. Alcohol poisoning hospitalisations peaked in summer as per previous years, but a second peak was observed in July 2023. Accidental poisoning injury deaths were lower than the previous 5-year average across most months of 2022–23.
Figure 6: Number of accidental poisoning injury hospitalisations (2023–24) and deaths (2022–23), by calendar month
Interactive graph showing the number of accidental poisoning injury hospitalisations by month in the latest year compared to the previous 5-year average, by substance category.]
Notes:
- The number of hospitalisations in the most recent financial year is shown by the bars, and the previous 5-year average by the dotted line graph.
- Month is based on month of hospital admission.
- Hospitalisation counts in June of the most recent financial year may be an underrepresentation of the true number of admissions - see technical notes for details.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database and ABS National, state and territory population.
Severity
There are many ways that the severity, or seriousness, of an injury can be measured. Some of the ways to measure the severity of hospitalised injuries are:
- number of days in hospital
- time in an intensive care unit (ICU)
- time on a ventilator
- in-hospital deaths.
More accidental poisoning injury cases require intensive care while hospitalised than other injury cases. The average number of days in hospital for accidental poisoning was lower than the average for all hospitalised injuries in 2023–24, while the percentages of cases that included time in an ICU and cases that involved continuous ventilatory support were both much higher. The rate of in-hospital deaths was lower for accidental poisoning compared to all injury causes (Table 1).
Severity measure | Accidental poisoning | All injuries |
|---|---|---|
Average number of days in hospital | 2.4 | 3.4 |
Percentage of cases with time in an ICU (%) | 9.9 | 2.1 |
Percentage of cases with time on ventilator (%) | 8.1 | 1.2 |
In-hospital deaths (per 1,000 cases) | 3.0 | 5.9 |
Note: Average number of days in hospital (length of stay) includes admissions that are transfers from one hospital to another or transfers from one admitted care type to another within the same hospital, except where care involves rehabilitation procedures.
Source: AIHW National Hospital Morbidity Database.
Over the past 10 years, the percentage of hospitalisations for accidental poisoning requiring either admission to an ICU, or time on CVS, has increased (Figure 7). The magnitude of increase has varied by category of substance. In 2023–24, over 1 in 5 accidental poisoning hospitalisations involving narcotics, opioids and hallucinogens resulted in time in an ICU. Just under 1 in 5 cases involving alcohol spent time in an ICU, but out of all substance categories alcohol poisoning hospitalisations had the highest proportions of cases requiring ventilatory support (15.7% in 2023–24).
Figure 7: Percentage of accidental poisoning hospitalisations requiring CVS or time in ICU, Australia, 2014–15 to 2023–24
Interactive graphs showing the percentage of accidental poisoning injury hospitalisations requiring ICU or CVS over the past decade, by type of substance

Note: The denominator for percentage calculations is the number of accidental poisoning injury hospitalisations related to a selected substance category in a given year.
Source: AIHW National Hospital Morbidity Database.
For more detail, see accidental poisoning supplementary data tables.
Age and sex
Rates of hospitalisation and death caused by accidental poisoning differ between males and females, and by groups of substances (Figure 8).
-
Accidental poisoning Hospitalisations 2023–24
- the highest number of cases was for males (5,402 cases, 53%)
- the age-standardised rate for males was 1.2 times that for females
- people aged 0–4 had the highest rate.
Bars show age-standardised rates per 100,000 population.
-
Accidental poisoning Deaths 2022–23
- the highest number of deaths was for males (971 deaths, 69%)
- the age-standardised rate for males was 2.4 times that for females
- people aged 45–64 had the highest mortality rate.
Bars show age-standardised rates per 100,000 population.
Figure 8: Number and age-standardised rate of accidental poisoning injury hospitalisations and deaths, by age group, sex and financial year, Australia
interactive graphs displaying age and sex trends over the past decade for accidental injury hospitalisations by selected substance type.
Notes:
- Age groups where the count is less than 5 are not displayed
- Crude rates where the numerator is less than 10, and age-standardised-rates where the numerator is less than 20 are not shown due to data volatility.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database and ABS National, state and territory population.
Most types of poison caused more hospitalisations and deaths in males compared to females over the past decade (Figure 8). Hospitalisations caused by nonopioid analgesics, antipyretics and antirheumatics were the notable exception that were more common in females.
Alcohol poisoning death rates were highest among males and 45-64 year olds, and rates have generally increased over time in these groups.
Accidental poisoning in children aged 0–4
Children aged 0-4 years have consistently exhibited the highest rates of accidental poisoning hospitalisation over the last decade for multiple substance groupings, including (Figure 8):
- Pesticides
- Unspecified drugs, medicaments, biological substances, chemicals or noxious substances
- Organic solvents, halogenated hydrocarbons and their vapours
- Nonopioid analgesics, antipyretics and antirheumatics
- Antiepileptic, sedative-hypnotic, antiparkinsonism and psychotropic drugs not elsewhere classified
However, hospitalisation rates in this age group have decreased in recent years, falling from about 94 per 100,000 in 2017–18 to about 77 per 100,000 in 2022–23 (an 18% decrease).
The most common causes of accidental poisoning in children aged 0–4 involve pharmaceutical substances. From 2017–18 to 2022–23 hospitalisation rates have decreased for all types of substances:
- a 17% decrease for other and unspecified drugs and biological substances (from 32.3 to 26.7 per 100,000)
- a 22% decrease for antiepileptics, sedatives and psychotropics (from 17.9 to 13.9 per 100,000)
- a 46% decrease for nonopioid analgesics, antipyretics and antirheumatics (from 12 to 6.5 per 100,000)
In contrast, looking at non-pharmaceutical substances, hospitalisation rates among children aged 0–4 for poisoning caused by other and unspecified chemicals and noxious substances have increased by 12% over the same period (from 14.9 to 16.7 per 100,000).
For more detail, see accidental poisoning supplementary data tables.
First Nations people
Among Aboriginal and Torres Strait Islander people (First Nations people):
- there were 887 hospitalisations due to accidental poisoning in 2023–24 (86.1 per 100,000 population)
- females and males had similar hospitalisation rates (86.5 and 85.5 per 100,000 population)
- hospitalisation rates were highest among people aged 0–4 (Figure 8)
- the commonest substances causing hospitalisations were the same as in the general population, being other and unspecified drugs and biological substances, antiepileptics, sedatives and psychotropics and narcotics, opioids and hallucinogens.
- there were 114 deaths due to accidental poisoning in 2022–23 (12.6 per 100,000 population)
- males were 2.8 times as likely as females to die (18.6 and 6.6 per 100,000 population) (Table 2).
The rate of hospitalisation differed across the lifespan. For both First Nations males and females, children aged 0–4 experienced the highest rate of hospitalisations due to accidental poisoning (Figure 9).
Figure 9: Accidental poisoning injury hospitalisations among First Nations people, by age and sex, Australia, 2023–24

Note: Columns are number of hospitalisations, and the line graph represents crude rate per 100,000 persons.
Source: AIHW National Hospital Morbidity Database, ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
Sex | Number of injury deaths | Crude mortality rate (per 100,000 population) |
|---|---|---|
Males | 84 | 18.6 |
Females | 30 | 6.6 |
Persons | 114 | 12.6 |
Note: Numbers and rates are reported for the following 5 jurisdictions combined: New South Wales, Queensland, Western Australia, South Australia and the Northern Territory. These jurisdictions are considered to have adequate levels of Indigenous identification in mortality data.
Sources: AIHW National Mortality Database, ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
For more detail, see accidental poisoning supplementary data tables.
Comparison between First Nations people and non-Indigenous Australians
First Nations people, when compared with non-Indigenous Australians, were:
- 2.6 times as likely to be hospitalised due to accidental poisoning in 2023–24
- 5.5 times as likely to die from accidental poisoning in 2022–23 (Figure 10).
Figure 10: Age-standardised rates of accidental poisoning injury hospitalisations and deaths by Indigenous status and financial year, Australia
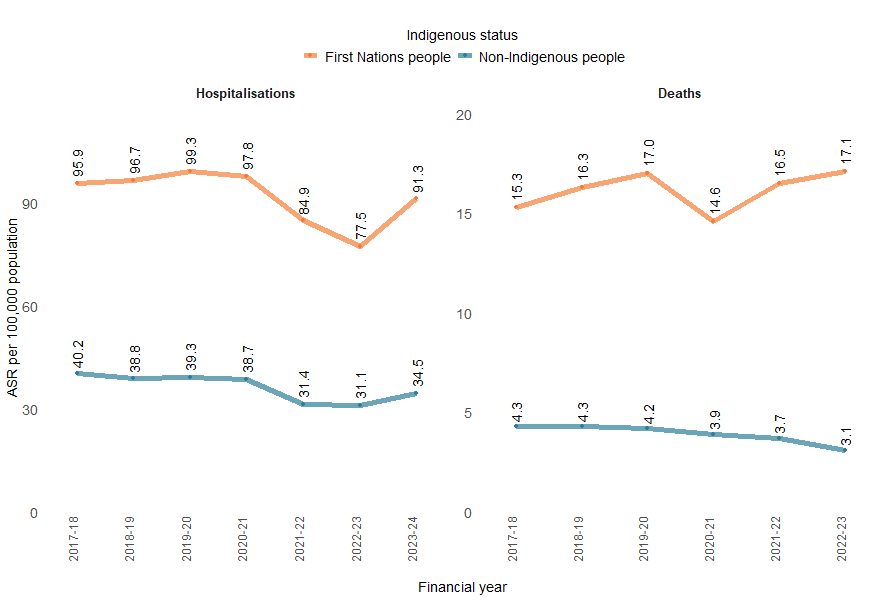
Notes:
- Age-standardised rate per 100,000 population.
- ‘Non-Indigenous people’ excludes cases where Indigenous status is missing or not stated.
- Deaths data only includes data for people whose usual residence was New South Wales, Queensland, Western Australia, South Australia, and the Northern Territory, as these jurisdictions are considered to have adequate levels of Indigenous identification in mortality data.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database, ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
The rate of accidental poisoning hospitalisations was highest among the 0–4 age group for both First Nations and non-Indigenous Australians (Figure 10). The commonest substances causing hospitalisations were the same as in the general population, being other and unspecified drugs and biological substances, antiepileptics, sedatives and psychotropics and narcotics, opioids and hallucinogens.
Deaths data are not presented because of small numbers.
Figure 11: Accidental poisoning hospitalisations, by Indigenous status, by age group, Australia, 2023–24
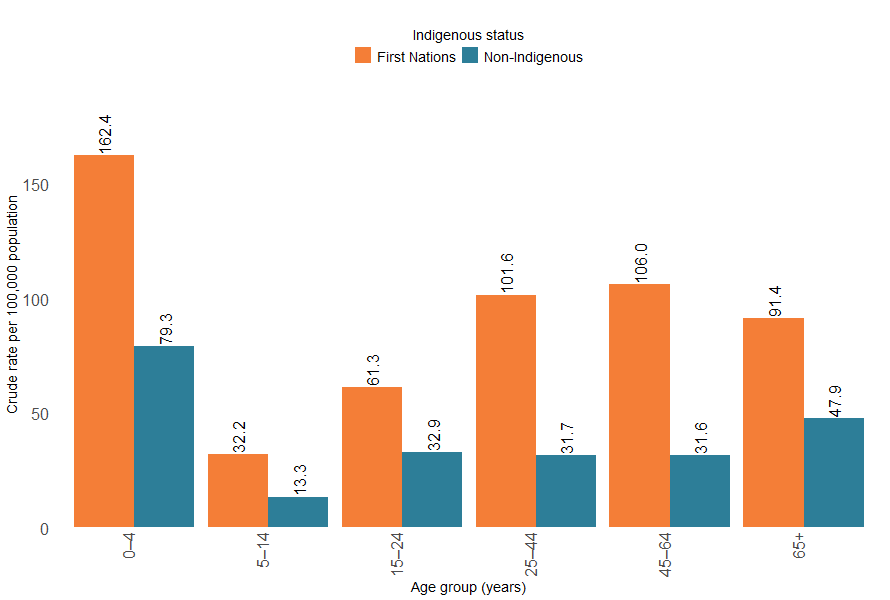
Notes:
- Rates are age-standardised per 100,000 population.
- ‘Non-Indigenous people’ excludes cases where Indigenous status is missing or not stated.
Source: AIHW National Hospital Morbidity Database, ABS Estimates and Projections, Aboriginal and Torres Strait Islander Australians.
For more detail, see accidental poisoning supplementary data tables.
States and territories
The states and territories with the highest rates of accidental poisoning hospitalisation in 2023–24 were:
- Northern Territory (49.0 per 100,000)
- Queensland (47.5 per 100,000)
- Western Australia (42.6 per 100,000) (Figure 12).
The states and territories with the highest rates of accidental poisoning deaths (where available) in 2022–23 were:
- Western Australia (8.9 per 100,000)
- Australian Capital Territory (6.7 per 100,000)
- Victoria (6.4 per 100,000) (Figure 12).
Figure 12: Age-standardised rate of accidental poisoning hospitalisations (2023–24) and deaths (2022–23), by state of usual residence, Australia
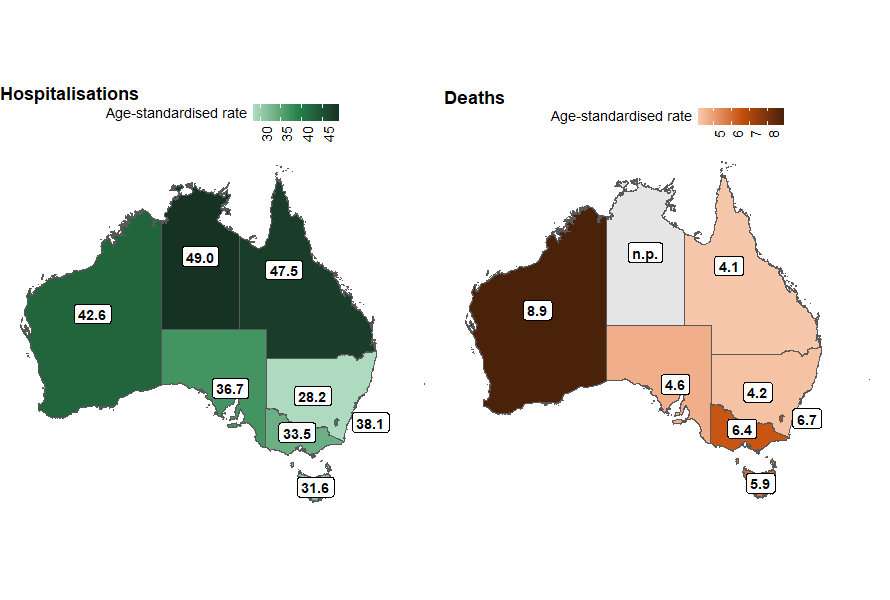
Notes:
- State and territory refers to the state and territory of usual residence for the individual.
- Age-standardised rate per 100,000 population.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database, and ABS National, state and territory population.
There are some differences in trends across states by type of substance involved (Figure 13). As compared to the previous 5-year average, 2023–24 saw an increased percentage of hospitalisations due to other and unspecified drugs, medicaments and biological substances across all states and territories except the Northern Territory. In 2022–23 there was an increase in overall poisoning death rates in the Australian Capital Territory and Tasmania.
Figure 13: Percentage difference in age-standardised rates of accidental poisoning injury hospitalisations (2023–24) and deaths (2022–23) compared to the previous 5-year average, by state or territory of usual residence, Australia
The rate of hospitalisation for accidental poisoning increased by 8.5% in Tasmania, and decreased in every other state and territory.
Notes:
- State and territory refers to the state and territory of usual residence for the individual.
- Age-standardised rate per 100,000 population.
Sources: AIHW National Hospital Morbidity Database, AIHW National Mortality Database, and ABS National, state and territory population.
For more information see the geography dashboard.
Remoteness
Remote areas of Australia tend to have higher rates of hospitalisation from injury due to accidental poisoning than less remote areas. People living in Remote areas had the highest rate of hospitalisation in 2023–24 (49.8 per 100) and were 1.5 times as likely to be hospitalised for accidental poisoning as people living in Major cities (Figure 14).
For most substances, the rates of accidental poisoning hospitalisation increased with remoteness (Figure 14). However, for poisoning caused by antiepileptics, sedatives and psychotropics, as well as narcotics, opioids and hallucinogens, the highest hospitalisation rates in 2023–24 were observed in Major cities.
Figure 14: Age-standardised rates of accidental poisoning hospitalisations, by remoteness, type of substance and financial year, Australia
For all types of substances, rates of hospitalisation for accidental poisoning increase with remoteness.

Notes:
- Age-standardised rate per 100,000 population.
- ASRs where the numerator is less than 20 are not shown due to data volatility.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
For information on how statistics are calculated by remoteness, see the technical notes.
Socioeconomic areas
People living in the most socioeconomically disadvantaged areas of Australia, compared to the least socioeconomically disadvantaged were:
- 1.7 times as likely to be hospitalised for accidental poisoning in 2023–24 (46.5 compared to 26.6 per 100,000 population) (Figure 15)
- 1.8 times as likely to die from accidental poisoning in 2022–23 (7.3 compared to 4.0 per 100,000 population).
Figure 15: Age-standardised rates of accidental poisoning hospitalisations, by socioeconomic areas, type of substance and financial year, Australia
Interactive graphs displaying trends in accidental injury hospitalisations over the past decade by selected type of substance and socioeconomic status of area of usual residence

Note: Age-standardised rates per 100,000 population.
Sources: AIHW National Hospital Morbidity Database and ABS National, state and territory population.
The following are recent publications that include information on accidental poisoning. Search Reports for older publications.


