Demand reduction
Demand reduction involves ‘preventing the uptake and delaying the onset of use of alcohol, tobacco and other drugs; reducing the misuse of alcohol, tobacco and other drugs in the community; and supporting people to recover from dependence through evidence-informed treatment’ (Department of Health 2017).
Examples of demand reduction initiatives include:
- information and awareness campaigns
- education and early intervention
- restrictions on the marketing and advertising of tobacco, alcohol and prescription drugs
- drug treatment programs
- programs focused on building protective factors and social engagement.
The National Drug Strategy Household Survey (NDSHS) provides national estimates of the use of tobacco, alcohol, and other drugs among the general population in Australia. The 2022–2023 NDSHS shows that tobacco and alcohol are the substances most commonly consumed by people in Australia (AIHW 2024b).
While there has been a long-term downward trend in tobacco smoking in Australia and many drinkers consume alcohol responsibly, a substantial proportion of drinkers consume alcohol at a level that increases their risk of alcohol-related harm (Figure HARM 2).
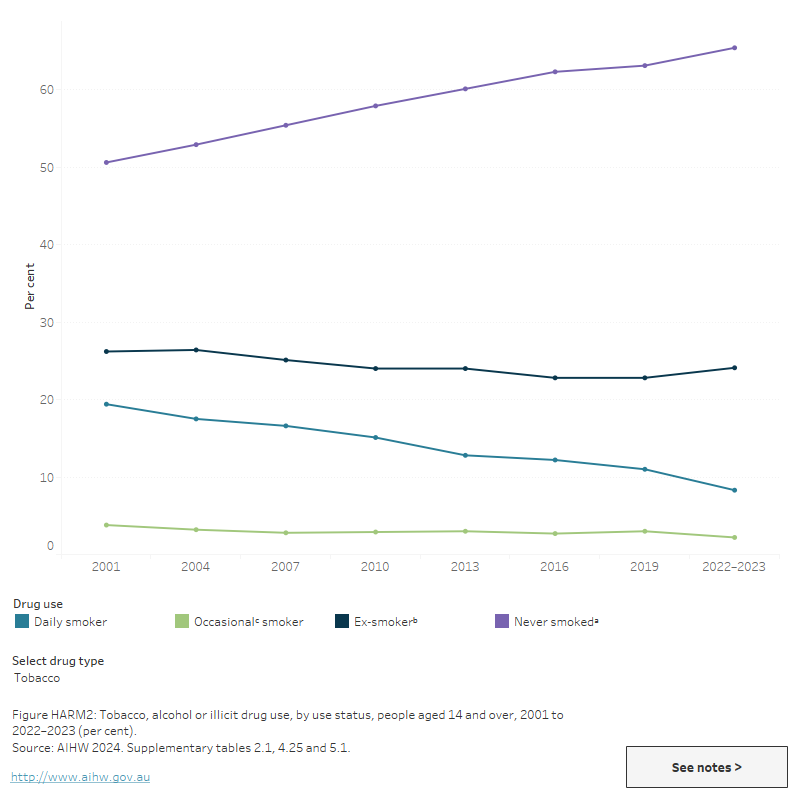
Figure HARM 2: Tobacco, alcohol or illicit drug use, by use status, people aged 14 and over, 2022–2023 (per cent)
This line graph shows that the proportion of Australians aged 14 and over who smoke daily declined between 2007 and 2022–2023 while the proportion who had never smoked increased. The proportion of people who were not at risk of alcohol related harm remained stable and was consistently higher than the proportion who consumed alcohol at risky levels or who abstained from alcohol. The graph also shows that the proportion of people who have used any illicit drug in their lifetime increased gradually between 2007 and 2022–2023 while recent use remained stable.
An illicit drug is defined as any drug which is illegal to possess or use or any legal drug used in an illegal manner (AIHW 2024b). The proportion of people who had used an illicit drug in their lifetime has been gradually increasing in Australia since 2001 (Figure HARM 2). In 2022–2023, 47% of people aged 14 and over in Australia had illicitly used a drug at some point in their lifetime and 17.9% had done so in the last 12 months (AIHW 2024b, table 5.1).
Cannabis is the most commonly used illicit drug in Australia (AIHW 2024b, Table 5.2), which is consistent with international data. The latest World Drug Report indicates that in 2021:
- Cannabis was used in the past year by 4.3% of the global population aged 15–64 (219 million people). According to qualitative assessments, cannabis cultivation has trended upward for a decade.
- Cannabis legalisation in parts across the world appears to have accelerated daily use and related health impacts (UNODC 2023).
For detailed information on the harms, availability and consumption of tobacco, alcohol and other drugs in Australia, see the separate section for each of the Drug types.
Treatment
Alcohol and other drug treatment services assist people to address their substance use through a range of treatments. Treatment objectives can include reduction, stabilisation or cessation of substance use, as well as improving health and social wellbeing. Treatment services can include:
- support monitoring and case management/ care co-ordination
- withdrawal management and rehabilitation programs
- brief interventions, counselling and group therapy including relapse prevention and cognitive behavioural therapy (CBT)
- pharmacotherapy treatments (AIHW 2024a).
The Alcohol and Other Drug Treatment Services National Minimum Data Set (AODTS NMDS) provides information on treatment provided to clients by publicly funded AOD treatment services, including government and non-government organisations. In 2022–23, AOD treatment services provided around 235,500 treatment episodes, to around 131,500 clients (AIHW 2024a).
Client engagement with a treatment service is limited by the accessibility of the service. The location of a service is a factor which impacts accessibility, particularly for clients who live in Remote and very remote areas. In 2016–17, clients who sought treatment in Regional and remote areas travelled 1 hour or longer in 28% of treatment episodes, compared with 10% of treatment episodes for clients in Major cities (AIHW 2019).
AIHW (Australian Institute of Health and Welfare) (2019) Alcohol and other drug use in regional and remote Australia: consumption, harms and access to treatment 2016–17. Cat. no. HSE 212. Canberra: AIHW.
AIHW (2024a) Alcohol and other drug treatment services in Australia: early insights, AIHW, Australian Government, accessed 16 April 2024.
AIHW (2024b) National Drug Strategy Household Survey 2022–2023, AIHW, Australian Government, accessed 04 March 2024.
Department of Health (2017) National Drug Strategy 2017–2026. Canberra: Australian Government. Viewed 12 January 2018.
UNODC (United Nations Office on Drugs and Crime) (2023) World Drug Report 2023. Vienna: UNODC, accessed 25 October 2023.


