Children with diabetes
Data updates
25/02/22 – In the Data section, updated data related to children with diabetes are presented in Data tables: Australia’s children 2022 - Health. The web report text was last updated in December 2019.
Key findings
- In 2017, around 6,500 children aged 0–14 had type 1 diabetes, a rate of 141 per 100,000 children.
- The prevalence of type 1 diabetes among children remained stable between 2013 and 2017.
- Aboriginal and Torres Strait Islander children were less likely than non-Indigenous children to have type 1 diabetes (89 compared with 137 cases per 100,000).
Diabetes is a chronic condition in which the body cannot properly use its main energy source—the sugar glucose. This is due to a deficiency in insulin (a hormone made by the pancreas to control blood glucose levels), or the inability to use the insulin available.
Diabetes is marked by an abnormal build-up of glucose in the blood and can have serious short and long-term effects, including:
- ketoacidosis
- kidney failure
- loss of eyesight and limbs
- disability
- premature death.
People with diabetes can control and reduce their risk of complications by ensuring that blood glucose levels remain within the normal range. Death due to diabetes is extremely rare among children aged 0–14. In 2014–16, there were fewer than 5 deaths from diabetes (AIHW 2018).
There are 2 main types of diabetes that occur in children—type 1 and type 2 (Box 1). Type 1 diabetes is the most common form of diabetes among children.
Box 1: Types of diabetes affecting children aged 0–14
Type 1 diabetes
This is a lifelong autoimmune disease that develops when the immune system destroys the insulin-producing cells of the pancreas, and usually has onset in childhood and adolescence (AIHW 2015). A person with type 1 diabetes needs insulin replacement to survive and, except in cases where a pancreatic transplant occurs, insulin will be required every day for the rest of their life. They must also maintain a careful balance of diet, exercise and insulin intake (AIHW 2015).
Type 2 diabetes
This is the most common form of diabetes among the Australian adult population and it occurs when the body becomes resistant to the insulin being produced by the pancreas and/or the amount produced is inadequate to meet the body's needs (AIHW 2017). While involving a genetic component, type 2 diabetes is largely preventable by maintaining a healthy lifestyle. Modifiable risk factors that can lead to type 2 diabetes include insufficient physical activity, saturated fat intake, obesity, and tobacco smoking (AIHW 2017).
Difficulties with determining the number of people with type 2 diabetes, including undiagnosed cases, misdiagnosis and misreporting mean there are currently no reliable national estimates of type 2 diabetes among children (AIHW 2014).
Type 1 diabetes It is the focus of this report, with data drawn from the National (insulin-treated) Diabetes Register (NDR) (Box 2).
Box 2: Data sources on type 1 diabetes
Data for this report come from the National (insulin-treated) Diabetes Register (NDR), a database of Australians who use insulin to treat diabetes. It was established in 1999 to monitor the incidence of insulin-treated diabetes in Australia, and aims to record all cases of people who begin to use insulin to treat their diabetes.
The NDR includes people with type 1 diabetes, insulin-treated type 2 and gestational and other types of diabetes. Data for the NDR are sourced from the National Diabetes Services Scheme and the Australasian Paediatric Endocrine Group’s state and territory registers.
For those with type 1 diabetes, age at first insulin use is used as a proxy for age of diagnosis.
How many children have diabetes?
Overall, 6,527 children had type 1 diabetes in 2017, a rate of 141 per 100,000 children.
Girls were slightly more likely than boys to have diabetes (144 compared with 138 per 100,000, respectively). This difference was greatest in children aged 10–14, with 288 per 100,000 girls and 273 per 100,000 boys.
In 2017, the prevalence of diabetes increased with age, with rates among 10–14 year olds 11 times as high as 0–4 year olds (280 compared with 26 per 100,000) (Figure 1).
Figure 1: Prevalence of type 1 diabetes among children aged 0–14, by age group and sex, 2017
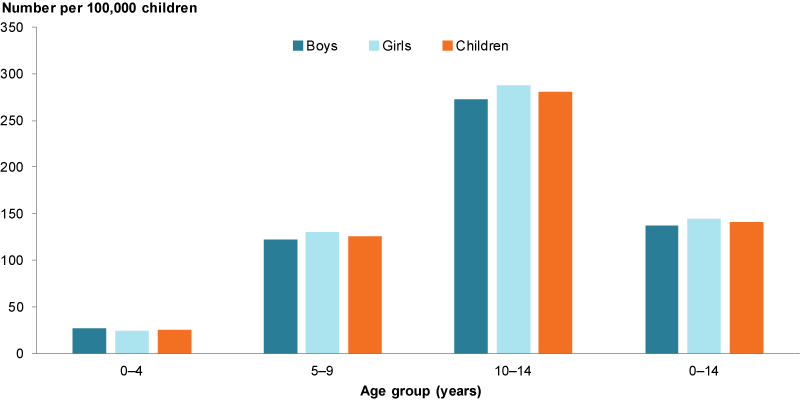
Source: AIHW analysis of 2017 NDR.
Has the rate of diabetes improved over time?
The prevalence of type 1 diabetes among children aged 0–14 remained stable between 2013 and 2017, at around 142 cases per 100,000 children (ranging between 140 to 143 cases per 100,000).
Is the rate of diabetes the same for everyone?
In 2017, the prevalence of type 1 diabetes was highest among children aged 0–14 living in Inner regional areas (169 per 100,000). This was followed by children living in:
- Outer regional areas (149 cases)
- Major cities (134 cases)
- Remote and very remote areas (86 cases per 100,000).
Non-Indigenous children were also more likely than Indigenous children to have type 1 diabetes (137 compared with 89 cases per 100,000).
Children born overseas were slightly more likely to have type 1 diabetes than children born in Australia (147 compared with 133 cases per 100,000).
The rate of type 1 diabetes among children aged 0–14 was similar across low and high socioeconomic areas (137 compared with 133 cases per 100,000) (Figure 2).
Figure 2: Prevalence of type 1 diabetes in children aged 0–14 by selected population groups, 2017
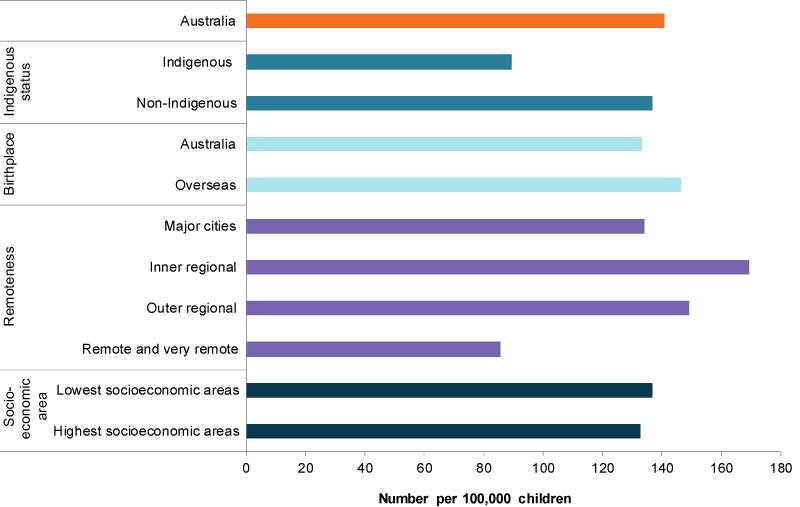
Source: AIHW analysis of 2017 NDR.
Data limitations and development opportunities
Australian research suggests that the diagnosis rate of type 2 diabetes in children is increasing, likely due to the increase of childhood obesity (NDSS 2019). Data development is being undertaken to enable reporting of accurate estimates of type 2 diabetes among children; however national data are not reliable enough for reporting on the very young at this time.
The number of Indigenous children with type 1 diabetes may be underestimated by the NDR, as identifying as an Indigenous person on both data sources of the NDR (Box 2) is voluntary (AIHW 2019).
Rates of type 1 diabetes may also be influenced by the lower capture of people living in Remote and very remote areas in the NDR data.
Where do I find more information?
For information on:
- type 1 diabetes in children, see: Incidence of insulin-treated diabetes in Australia and Prevalence of type 1 diabetes among children aged 0–14 in Australia, 2013
- complications associated with diabetes in childhood, see: Diabetic ketoacidosis among children and young people with type 1 diabetes
AIHW (Australian Institute of Health and Welfare) 2014. Type 2 diabetes in Australia's children and young people: a working paper. Cat. no. CVD 64. Canberra: AIHW.
AIHW 2015. Prevalence of type 1 diabetes among children aged 0–14 in Australia, 2013. Cat. no. CVD 70. Canberra: AIHW.
AIHW 2017. Diabetes. Canberra: AIHW. Viewed 9 May 2019.
AIHW 2018. General Record of Incidence of Mortality (GRIM) books: GRIM0403 Diabetes 1907–2016. Cat. no. PHE 217. Canberra: AIHW.
AIHW 2019. Incidence of insulin-treated diabetes in Australia. Cat. no. CDK 11. Canberra: AIHW.
NDSS (National Diabetes Services Scheme) 2019. Type 2 diabetes in children and young adults. Viewed 11 October 2019.
- Year of first insulin use is a proxy for year of diagnosis.
- Incidence rates of type 1 diabetes may be influenced by the lower capture of Indigenous Australians and people living in Remote and very remote areas on the primary data sources of the National (insulin-treated) Diabetes Register.
- Remoteness is classified according to the Australian Statistical Geography Standard 2016 Remoteness Areas structure based on postcode of current residence.
- Socioeconomic groups are classified according to population-based quintiles using the 2016 Index of Relative Socio-Economic Disadvantage based on Statistical Area Level 2 of current residence.
- For data quality information see the National (insulin-treated) Diabetes Register 2016; Quality Statement on Meteor.
For more information, see Methods.


